Dynamic volume CT - the impact on neuro-imaging
By Georg Bohner MD, Department of Neuroradiology, Charité University of Medicine Berlin, Germany
A 320-row CT scanner (Aquilion One, Toshiba Medical Systems Co., Tokyo, Japan) was installed for the first time in Europe, at the Charité University Hospital, Berlin, Germany, in November 2007. Its capability to cover the whole brain in a single rotation means this new type of scanner has the potential to impact strongly on the field of neuro-imaging.

Due to the limited detector width available in conventional multislice CT scanners dynamic imaging used for perfusions studies, or time-resolved angiography, was limited to partial organ coverage only (20 to 40 mm scan length). To overcome this limitation, repeated scanning in an adjunct region or table movement during examination was necessary, which limited time resolution in dynamic imaging studies.
For the first time, this limitation has been overcome by volumetric, time-resolved whole-brain imaging using the 320-row scanner with its high-resolution coverage of 160 mm during a single rotation.
Simultaneously morphological as well as functional image data are collected.
The dynamic volume CT uses a detector module arranged in a 320 x 0.5 mm configuration. There are 896 detector rows x 320 elements, with an element size of approximately 1 x 1 mm, which corresponds to a 0.5 mm (transverse) x 0.5-mm (longitudinal) beam width at the centre of rotation. The fastest gantry rotation time is 0.35 seconds and the data sampling rate is 2,572 views per second.
Within the first weeks of usage the following acquisition techniques were applied at the Charité for neuro-imaging studies using the dynamic volume CT: Single rotation cranial CT (SR-CCT), incremental cervicocranial CT-Angiography (3-D-CTA), time resolved intracranial CT-Angiography (4-D-CTA) and a combined whole brain 4-D-CTA and CT perfusion protocol (4-D-CTA/CTP).
Following the scan protocol for the combined angiography and perfusion scan will be addressed briefly. For the 4-D-CTA/CTP protocol we use a combination of intermittent and continuous scanning for a total examination time of 50 seconds, after having performed a test bolus scan to determine the circulation time. After injection of 50ml iodinated contrast agent, scanning is performed using an 80kV protocol that results in a dose length product of 2355,4 mGy x cm. Multiplied with the ICRP-factor (k=0.0023 mSv x mGy-1 x cm-1 for the head) this would result in a calculated effective dose of 5,4 mSv. This is in line with manufacturer’s phantom measurements where radiation exposure for the dynamic whole brain 4-D-CTA/CTP combination results in 6.4 mSv.
Indications for dynamic volume CT comprised, amongst others, trauma, acute stroke, chronic ischemia due to arteriosclerosis of cervicocranial vasculature as well as veno-occlusive disease.
Based on our initial experiences the scan speed of SR-CCT and 3-D-CTA protocols are the main advantages over conventional multislice CT scanners, with the potential to reduce motion artefacts in uncooperative patients.
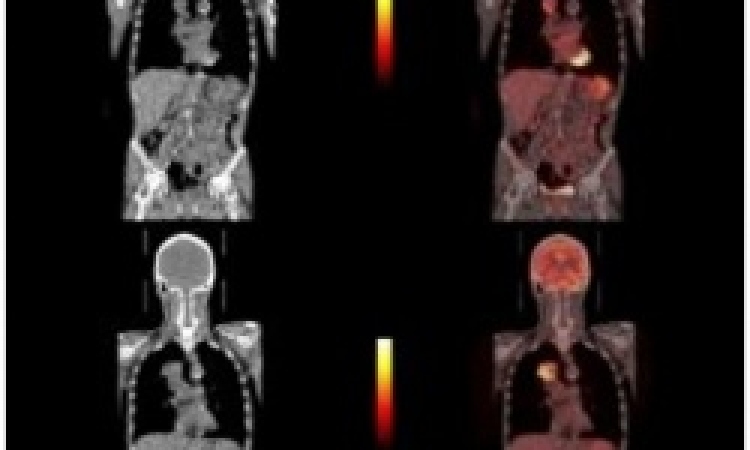
In stroke imaging, it is likely that the sensitivity of CT perfusion imaging will increase, especially with respect to infratentorial ischemic lesions, or lesions within the semioval centre and the frontoparietal cortex, although the clinical impact of such findings is still a matter of discussion. As illustrated here (Fig. 1), volumetric perfusion imaging enables whole brain coverage and calculation of high resolution parameter maps with 0.5 mm voxel size along the z-axis.
Especially when altered haemodynamics are suspected, the time resolution combined with the complete brain coverage provided by the
4-D-CTA and the combined
4-D-CTA/CTP protocols are interesting new scanner features. Up to now, no dynamic whole-brain angiography was available based on CT technology; thus assessment of circulation time changes in shunting vascular disorders, venous arterialisation or prolongation of venous outflow in the setting of veno-occlusive disease, especially in cortical vein thrombosis, remained limited using CT. All these neuroradiologically important issues can now be addressed directly and dynamically by whole brain 4-D-CTA.
However, with the new technique of dynamic volume CT not only the quality of information increases but also the quantity, as for a complete stroke examination, together with the postprocessed images, a total amount of up to 18,000 images can result. Not only high-end workstations for image reconstruction are needed to limit the time of data postprocessing, which can take up to 15 minutes only to calculate the parameter maps in stroke evaluation, but also high speed network connections and a powerful PACS system are needed to cope with the large amount of data.
10.03.2008