Computed tomography versus magnetic resonance imaging of the heart
Competitive or complementary?
By Florian Schwarz BS, Balazs Ruzsics MD PhD and U. Joseph Schoepf MD, of the Radiology and Medicine Departments, at the Medical University of South Carolina, Charleston, USA.
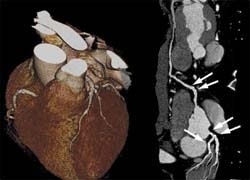
The rapid pace of technological developments both in cardiac Magnetic Resonance Imaging (MRI) and cardiac Multi Detector-Row Computed Tomography (MDCT) keeps revolutionising the field of cardiac imaging. In this contribution we intend to give a brief overview over the specific imaging capabilities of cardiac MDCT versus cardiac MRI and highlight some typical differential indications.
Multidetector computed tomography of the heart
In the last decade, the majority of clinical studies on cardiac MDCT focused on coronary artery disease (CAD), both in the acute and preventive setting.
Traditionally, the first approach in the evaluation of CAD with MDCT is the quantification of coronary artery calcification. The correlation between the extent of coronary artery disease and coronary calcification is supported by substantial clinical evidence. Various ways of reporting the calcium burden have been established (Agatston-Score, Calcium Mass, Calcium Volume). It has been shown that the extent of calcification has a high predictive value for subsequent coronary events, so that Calcium Scoring has been established as a tool for risk stratification in a preventive setting.
As there is no one-on-one relationship between coronary artery calcium and coronary artery stenosis, the detection of obstructive coronary artery disease requires assessment of the arterial lumen. This analysis has been traditionally performed invasively with coronary artery catheterisation. Recently, however, the value of CT Coronary Angiography (CTA) has been recognised, particularly owing to its high negative predictive value for non-invasively ruling out significant stenosis in patients with atypical chest pain or prior equivocal or non-diagnostic test results. Compared with conventional coronary artery catheterisation, recent clinical trials of CTA with 64-slice CT or later generation scanners report sensitivities approaching 100% and specificities of over 95% in the diagnosis of obstructive coronary artery disease. It has also been shown that CTA is a valuable tool for the assessment of coronary artery anomalies and coronary bypass patency.
With the advent of faster scanner generations, CTA is increasingly extended to detect coronary artery disease, pulmonary embolism, acute aortic syndromes, and other thoracic pathology with a single, ECG-synchronized contrast enhanced CTA study of the entire chest. This paradigm has been dubbed the ‘triple rule out’ scan and has been demonstrated in initial studies to be both, time- and cost-effective in the assessment of acute chest pain.
The combination of speed and spatial resolution provided by CTA is unprecedented, making it the premier non-invasive tool for the assessment of coronary artery lumen integrity. Increased research interest is currently directed at deriving information on myocardial perfusion and viability with advanced MDCT techniques. Similarly, since functional information is obtained with every retrospectively ECG-gated CTA scan, this ancillary information is ordinarily exploited to also assess cardiac function and segmental wall motion. For the latter applications, however, CTA is in strong competition with other imaging modalities, primarily nuclear medicine techniques, which have been traditionally used for the assessment of cardiac perfusion, echocardiography as the most commonly used tool for the evaluation of cardiac function, and MRI, which currently still exceeds the temporal resolution of CT for the assessment of cardiac function, enables the spatially resolved evaluation of myocardial perfusion and does not expose the patient to ionising radiation.
Cardiac MRI
Because of the limitations of other clinical methods (e.g. poor acoustic windows at echocardiography, limited spatial resolution and specificity of nuclear medicine myocardial perfusion scans), cardiac MRI is shaping up as the new reference standard for the assessment of myocardial function, perfusion and viability. Compared to MDCT, MRI has significantly better contrast resolution and, seen in isolation, in theory has better temporal and spatial resolution. Currently available cardiac MRI scanners and sequences, however, are unable to combine spatial and temporal resolution to match cardiac MDCT for the detailed assessment of the coronary artery lumen.
Our routine cardiac MRI protocol is designed to yield comprehensive information on cardiac morphology, function, perfusion and viability within a 40 min time-frame. For the routine MRI workup of the heart, contrast agent is administered to study two phenomena: First-pass kinetics (= perfusion imaging) and delayed enhancement of the myocardium. The perfusion scan is typically performed twice, after application of pharmacologic stress and at rest. In 4-5 representative sections of the heart the wash-in of the contrast agent is recorded in real-time. This allows for the reconstruction of a detailed perfusion map. Thus, rather than evaluating for obstructive coronary artery disease directly, such as with MDCT, the presence of significant coronary artery stenosis is indirectly deduced from the presence of perfusion deficits within the dependent myocardium.
A milestone in the field of cardiac-MRI in the ‘90s has been the discovery of the effect of delayed enhancement (DE). DE Imaging makes use of the fact that hyper-enhancement on DE Images (performed 10-12 minutes after contrast administration) represents irreversibly injured myocardium (due to any kind of heart disease). This way, important information on the likely success of revascularisation (e.g. via bypass grafts) can be objectively established.
Conclusion
For the responsible clinician it is important to recognise that both tomographic imaging modalities of the heart have their unique strengths and weaknesses which are currently intrinsic to the physical underlying principles and limitations, which will not be overcome in the near future. The primary strength of MDCT clearly is the morphological assessment of the coronary arteries, whereas ischemic sequelae and their effect on cardiac function, perfusion and viability are preferably evaluated with cardiac MRI. Therefore, pending future developments, we have come to discourage the notion of the often proposed “one-stop-shop” in cardiac imaging with a single modality. Both techniques are important, evaluate different manifestations of coronary artery disease and thus complement each other. It is our responsibility as physicians to judiciously choose the appropriate imaging modality for each patient and for each clinical scenario.
Contact: schoepf@musc.edu
01.03.2008