Article • Rising up
Anaesthesia is a story of great success
Technical innovations and the implementation of quality standards in anaesthesia have immensely increased patient safety.
Report: Michael Krassnitzer
‘Over the past 60 years, patient safety during anaesthesia has improved more than in any other medical discipline,’ according to Professor Achim von Goedecke MD MSc, Director of the Institute of Anaesthesiology and Critical Care at Landeskrankenhaus Steyr in Upper Austria. Good news, since anaesthesiology plays a crucial role in reducing perioperative mortality and increasing patient safety. Today, industrial nations report perioperative complications in three to 16 percent of surgical interventions; 0.4 to 2.0 percent of these cases result in permanent damage or death, as explained by von Goedecke at the annual meeting of the Austrian Society of Anaesthesiology, Reanimation and Critical Care (ÖGARI) in Vienna.

‘While each incident is one too many, the statistics reflect a remarkable success story: The number of anaesthesia-associated deaths dropped from 100/100,000 cases in the 1940s to the current level of 0.4/100,000,’ he says (see box), and adds that ‘a major improvement has been reported since the late 1980s, when further safety standards and improved training were implemented.’ In 2010, the European Board of Anaesthesiology (EBA) and the European Society of Anaesthesiology (ESA) jointly published the Helsinki Declaration on Patient Safety.
At the same time a special Task Force was founded to ensure implementation of the actions identified in the declaration. In 2013, a European platform was established that collects and publishes safety warnings and recommendations by the European incident reporting systems.
Anaesthesia-associated mortality per 100,000 surgery patients | |
1940s | 100 |
1960s | 80 |
1970s | 10-30 |
2016 | 0.4 |
Important as they might be, standards ensuring safety and quality in anaesthesiology as well as recommendations to manage critical clinical situations are only one success factor. The dramatic reduction of mortality and concomitant progress in patient safety are, to a large extent, due to medical technology innovation:
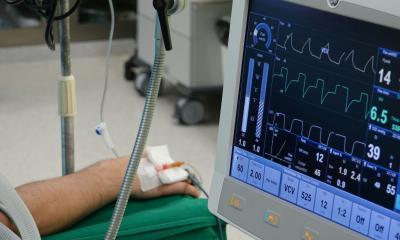
- Pulse oximetry. Continuous and non-invasive measurement of blood oxygen saturation is a parameter of respiratory function and the heart-lung system because it shows the peripheral pulse waves.
- Expiratory CO2 monitoring (capnometer and capnography) is a gas exchange parameter that provides data on the pulmonary and circulatory function as well as on the correct placement of the ventilation tube.
- Neuromuscular monitoring. Intraoperative relaxation monitoring of muscle function is important with regard to ventilation tube placement and in certain interventions, such as abdominal laparoscopy.
- Invasive haemodynamic monitoring allows, among others, intra-arterial pressure measurement, which in turn offers data on important cardio-vascular parameters.
‘In the past decades, these innovations have helped to save many lives and they are contributing significantly to patient safety,’ Goedecke underlines.
A slight perioperative mortality increase
Advances in medical technology have led to more difficult and complex interventions
Achim von Goedecke
‘Nevertheless, recent figures show a slight increase again in anaesthesia-specific and perioperative mortality in general. ‘This is not related to any deterioration of the safety standards but simply to the fact that more older and multi-morbid patients undergo anaesthesia and surgery,’ the expert points out. In Germany, the number of surgical patients over 75 years rose from 2.3 million in 2006 to 3.9 million in 2016, which translates into an increase from 18 to 23 percent of all patients. ‘In addition, advances in medical technology have led to more difficult and complex interventions. Today surgery, as such, is associated with many more risks,’ he explains. Among patients without relevant systemic diseases anaesthesia-associated mortality is stable at 0.0004 percent, whilst in patients with severe multi-morbidity the number increases by factor 100. The conclusion, von Goedecke says, is simple: ‘We have to put even more effort into patient safety.’
Profile:
Professor Achim von Goedecke MD MSc studied medicine at RWTH in Aachen, Germany. As a medical officer in the air force (1985-95), he became junior physician for anaesthesiology and critical care at the German Armed Forces Hospital in Berlin. He joined the Anaesthesia and Critical Care department at Philipp University Hospital, Marburg, Germany, in 1996, and completed his specialist training. In 2001 he became senior physician at the Anaesthesia and General Critical Care Clinic in Innsbruck University Hospital, Austria. Public health studies and his habilitation thesis were undertaken between 2004-2006. He has directed the Institute of Anaesthesiology and Critical Care at Landeskrankenhaus Steyr in Upper Austria since 2008, and is a board member of the Austrian Society of Anaesthesiology, Reanimation and Critical Care (ÖGARI).
10.04.2018