Sponsored • Manufacturers vs. bureaucracy
‘We will master this problem’
Report: Lena Petzold
Norms and directives are the backbone of medical devices manufacture. Frequent updates keep them current, but also often create unforeseen problems, especially for smaller and medium-size companies, because the bureaucracy is rarely considered.

No exception to this, the EU IVD directive, issued in May 2017, contains new definitions of requirements for in-vitro diagnostics. The new version stipulates more extensive documentation requirements than before. ‘This creates significant, additional expenditure for manufacturers,’ says Christian Hötzl, founder of Teco Medical Instruments, Production + Trading.
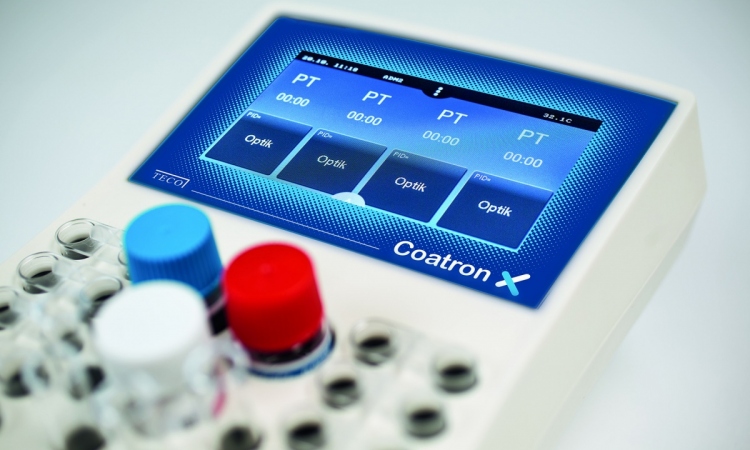
He knows this from his own experience with ISO 13485, a standard that governs requirements for medical products manufacture – its latest version came into force in 2016. ‘We are a company with 20 employees, which offers products and solutions for blood tests,’ Hötzl explains. ‘We have customers worldwide. Prior to the introduction of the standard, it was possible for an employee appointed as a quality management representative to take on the documentation requirements, i.e. the drawing up of protocols, writing of product descriptions and defining of workflows. The extension of the obligations has made it nigh on impossible for all the necessary steps to be managed by one person alone, especially as the risk assessment now includes the manufacture.’
This means that a comprehensive risk analysis must be carried out during the production process. ‘As a manufacturer we obviously always try to optimise processes and make them safe; but now we must document in writing that we have analysed and, if necessary, remove the possible risks involved in each and every step of the procedure.’
Coagulation diagnostics is an extremely sensitive field because incorrect treatment with anticoagulants can be life-threatening
Christian Hötzl
One particularly critical point is the expansion of the market surveillance obligations. ‘Manufacturers must document that they scrutinise the market extensively and that they react to any potential risks,’ Hötzl explains. Companies are asked to publish any notifiable errors without delay. These are published in central databases such as the BfArM (Federal Institute for Drugs and Medical Devices) portal. ‘We have to check these notifications and, if problems are reported for products in similar areas, such as competitors’ products in the field of coagulation diagnostics, we need to investigate without delay if these problems can potentially also occur with our products. If this is the case we need to take the necessary countermeasures at once, otherwise we are obliged to provide precautions to ensure that the problem cannot even arise.’
In the worst case, this can affect an entire series of devices and may necessitate a product recall. As we know from the automotive industry, this can quickly assume alarming proportions. However, this is not the only reason why accurate operation is a top priority. ‘Coagulation diagnostics is an extremely sensitive field because incorrect treatment with anticoagulants can be life-threatening,’ he warns.
The manufacturers’ responsibility not only extends to accurate operation. According to the standards, all manufacturers must take precautions to ensure that their products cannot predictably be misused. ‘Exactly what this means is not clearly defined in the standard, forcing manufacturers to comprehensively safeguard themselves in all directions,’ Hötzl emphasises. This includes the design of devices with long-term stability in mind. ‘We carry out extensive life-time measurements and test and record the stability of the measurement optics, the heaters and all other parts potentially prone to wear and tear,’ Hötzl explains. ‘However, it’s even more important to maintain good working relationships with distributors and customers to find out exactly how the products are being used on a day to day basis. Workflow differs from laboratory to laboratory, so it’d therefore essential to maintain communication and find out about any potential sources of error at an early stage.’
However, even this is not enough to guard against misuse. ‘We are also required to prevent so-called anomalous use. This includes, for instance, the use of cuvettes that are not licensed. Our quality cuvettes, devices and other consumer and wear parts are subject to the strictest quality standards. Products from manufacturers that are not licensed can be of lower quality and can block the devices or even falsify measurement results. Although we are not responsible for the potential use of any third-party cuvettes we can ultimately be made liable. From a legal perspective, as soon as we become aware of the existence of any such problematic cuvettes we may be accused of not having done enough against any predictable anomalous use.’
Therefore, the company has gone on the offensive and has developed a closed system for its own products. ‘Our devices only allow the use of certified, original cuvettes. After delivery to the end user these are scanned via a barcode system, or an RFID-tag. This identification prevents the use of other products.’ Risk analysis and safeguarding against misuse may amount to a heavy workload, but Hötzl is optimistic: ‘We have more than 25 years’ experience in the market and will master this, despite all the bureaucracy.’
Profile:
Christian Hötzl is founder and shareholder of Teco Medical Instruments, Production + Trading. Following an apprenticeship as a physics laboratory technician, he completed a degree course in medical technology at the Medical Technical Academy Esslingen, Germany. For the next six years, he worked for a medical devices manufacturer in Munich, initially as international head of service and later entered sales and development, his last role being acting production manager for coagulation analysers. In 1990, by buying the coagulation division, he founded Teco GmbH and has since successfully focused on worldwide distribution of his products.
08.02.2018