The hospital protocol for dealing with terrorism
By Cynthia E Keen
From 2000 to 2007, Israeli hospitals have treated the victims of 148 terrorist attacks.
At ECR 2008, radiologist Dr Ahuva Engel described the protocol developed to deal with such emergencies at the Rambam Medical Centre in Haifa.
When a suicide bombing or other multiple casualty incidents occur, more than 50% of the injured arrive at the hospital within five to 20 minutes. Immediately on notification, the Ramban Medical Centre cancels all scheduled radiology procedures. Portable X-ray machines and ultrasound machines are moved to the emergency department, as well as mobile PACS diagnostic workstations.
The medical staff identifies two distinct phases in dealing with victims. First, the emergency physicians and staff, radiologists and surgeons identify the most critically injured. Next, they treat non-life threatening injuries. Both stages require heavy use of diagnostic imaging equipment.
At the Centre, at least two radiologists go to work within the emergency department, along with as many radiographers needed to operate the portable diagnostic equipment.
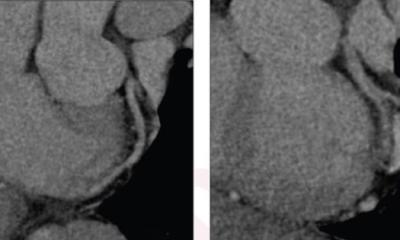
All front-line staff and physicians use walkie talkies for rapid communication. The objective is to determine who needs the most urgent care – particularly surgery. Chest radiography and focused abdominal ultrasound are the most commonly used imaging procedures in the emergency department. Computed tomography is also used to assess the abdominal injuries of more stable victims and to evaluate shrapnel localisation and detect unsuspected injuries. The most critically injured patients bypass X-rays in lieu of CT examinations.
CT angiography (CTA) helps radiologists and cardiologists to more accurately evaluate the vessels. Approximately 25% of the victims undergo this procedure, which reveals vessel stenosis, dilation, and pseudo-aneurysms. Conventional angiography is used if endovascular treatment is necessary.
According to Dr Engel, the most common injuries from explosions are damage to air containing organs (lungs or bowels). Victims thrown into the air, or hit by debris, may have a variety of broken bones and other orthopaedic injuries, cervical spinal injuries, or incur closed head injuries.
Penetrating wounds from numerous fragments of shrapnel are imaged to determine which may be life-threatening. For victims with numerous shrapnel pieces embedded, there is no way that all can be surgically removed during the initial frantic period. Their removal may need surgery over a period of weeks.
PACS workstations enable multiple physicians to evaluate examination results. The simultaneous availability of images has expedited surgery and treatment, because radiologists and surgeons can make their clinical assessments simultaneously. The use of 3-D reconstruction software helps surgeons to determine life threatening fragments.
‘Planning and practice of protocols to deal with mass casualties are critical for a hospital to respond effectively,’ Dr Engel emphasised. ‘No amount of medical experience prepares you for the chaos. Anticipating the worst case scenarios will help all medical staff to prepare for the aftermath of terrorism.’
* A large number of X-rays and CT scans of victims of terrorist attacks, obtained from two Jerusalem hospitals, have been compiled as an art exhibition currently touring galleries in the USA. These may be viewed online at: www.x-rayproject.org
30.04.2008