The flying magnet
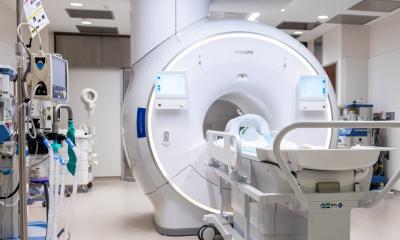
When Professor PD Dr Dr Marcos Tatagiba operates the recently installed five ton, ceiling mounted MRI scanner in the operating theatre at the Neurosurgery Clinic in University Hospital Tubingen, he will be using systems technology currently unique in Europe.
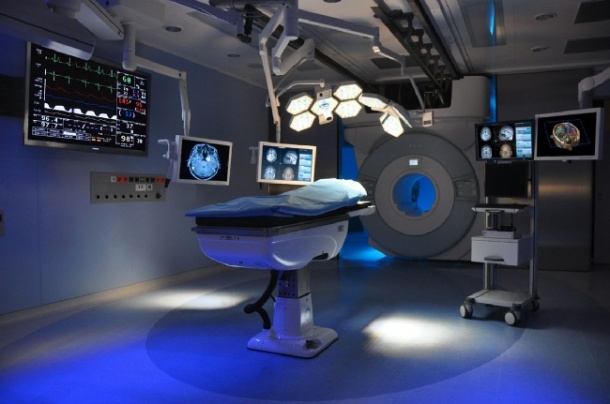
Carrying out around 3,200 surgical operations annually, the hospital ranks among the largest in Germany and, since 2004, it has seen continuous modernisation to provide most up-to-date medical technology. In spring this year, following a complex installation that began in October 2010, this was complemented by the intra-operative MRI scanner. ‘Despite the high-tech equipment in the clinic the patient always remains at the centre of things,’ Prof. Feigl pointed out.
The new iMRI system includes an HF cabin, which protects the operating theatre from interfering frequencies from outside, and a steel frame on which the 1.5-Tesla magnet runs in 90 seconds from the opened magnet bay (called the ‘garage’ by the Tubingen team) to the operating table.
15 April saw the official opening of the iMRI unit with the IMRISneuro system, and the €5 million operating theatre, named after Prof. Garnette Sutherland.
Since then the team has been operating on one patient per day. The main indications for treatment are primary brain tumours, Professor Feigl explained. ‘Low grade glioma, in particular, do not absorb contrast media. Visually the tissue often looks just like normal brain tissue. Previously, until the point where the first post-operative image was available the day after surgery, there was no absolute certainty that the tumour had been completely removed but, with the new system, we are now the first neurosurgical clinic in Europe able to monitor during surgery, whether or not the resection was successful, without the need to move the patient, which is what needs to be done with stationary magnets.’
Today, the neurosurgeons carry out everything directly in the operating theatre, from planning imaging procedures to postoperative imaging, all in close cooperation with the neuroradiology department under medical director, Professor U Ernemann. This has particular advantages for brain surgery, Professor Feigl said. ‘As soon as surgical access to the tumour is carried out, and then during the operation while the tumour tissue is removed, the brain moves – a process known as “brain shift”. The pre-operative images, which are required for neuronavigation, then no longer match with reality and must be updated.
‘After the operation, we produce a postoperative MRI image that would normally have to be carried out separately the next day. We then merge the pre-, intra- and postoperative MRI images into a before and after series at the workstation, which allows precise presentation of the outcome of the operation.’
Safety first
Before the steel door between the magnet bay and the operating theatre opens and the MRI scanner is moved to the special, non-magnetic operating table via a switch, the team carries out a standard safety check, for which they received special training. With the help of hard copy and soft copy checklists they ensure that all ferromagnetic instruments and equipment have been placed outside the five Gauss line. Three colour-coded Gauss lines around the operating table indicate which zones have which magnetic force.
The acquisition of specialist, non-magnetic operating theatre equipment is not necessary. When the magnet is ‘parked’ behind closed doors in the room next door -- the magnet bay -- all instruments can be freely used in the operating theatre.
Promising prospects
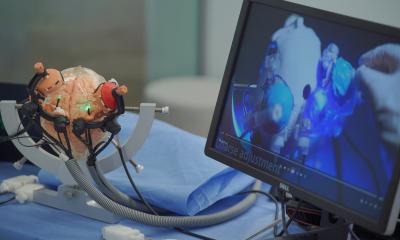
The iMRI unit in Tubingen has a special volumetric neuronavigation system (MedSurgical, Sunnyvale California). The difference from conventional navigation systems is that all image layers can be merged so that the entire volume of the skull can also be intra-operatively reconstructed in 3-D.
The system also makes it possible to make layers of tissue transparent. The neurosurgeon can look into the patient’s cranium with the system’s pointer before the cranium has even been opened to plan the safest surgical access.
Important functional data , acquired pre-operatively, such as information on cerebral areas relating to motor function and fibre tracts, are also shown to ensure that the smallest possible surgical access is carried out whilst full functionality is maintained.
In the future, the team also plans to carry out MRI imaging with the IMRISneuro system intra-operatively, because tumours in the central region of the brain can shift the normal anatomy to such an extent that the normal landmarks for certain functional areas in the brain lose their significance. It is also important to show the cerebral paths originating in these function- or motor specific areas as they also may have shifted.
Further areas of application are interventions for epilepsy, deep brain stimulation, surgery on the pituitary gland as well as surgery for vascular malformations such as aneurysms and AVM. ‘We are at the very beginning of our scope of experience with the new system,’ said the professor, adding: ‘We’re really just getting started.’
IMRIS arrives in Europe
IMRIS Inc. based in Winnipeg, Canada, has been offering image guided therapy solutions for neurosurgery, the neurovascular and cardiovascular fields since 2005. The mobile MRI scanner technology was developed in the 1990s by Dr Garnette Sutherland, neurosurgeon at the Foothills Hospital in Calgary, together with Dr John Saunders at the Canadian National Research Council (NRC) Institute of Biodiagnostics in Winnipeg.
50 customers in North America, the Asiatic-Pacific area and now in Europe are already working with the IMRIS systems, which are available in individual room configurations. The second neurosurgical installation will be carried out in September at the Clinatec Hospital in Grenoble, France, under Professor Alim-Louis Benabid. For the first time in Europe, Grenoble will have a two-room solution consisting of an operating theatre and a room for diagnostic imaging.
Report: Karoline Laarmann
02.09.2011