Personal shear rate therapy
In 1839 Richard Thoma was the first to observe that arteries respond to flow: he identified a fundamental relationship between blood flow and arterial calibre.
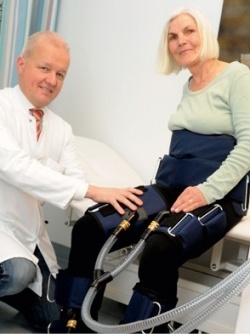
This important physiological mechanism currently has a renaissance in vascular medicine: Enhancing arterial flow and flow velocities rather than pressure is an important activating mechanism in the growth of biological bypasses (arteriogenesis). This can be achieved non-invasively by externally compressing arteries after a systolic pulse wave in such a way that a diastolic augmentation is achieved.
This involves fitting cuffs around the calves, lower and upper thighs and buttocks, which are then inflated and deflated by a compressor. Whereas researchers believed that the haemodynamic changes in blood pressure would be the underlying mechanism of clinical improvement, it is now shown that this mechanism is far more complex, according to Dr Ivo Buschmann, a specialist in vascular medicine at the Charité Clinic in Berlin: ‘The effect of blood volume redistribution is probably overestimated, however blow flow is accelerated, in a similar way to what would happen during a gentle run, without a significant increase in heart rate. The objective of this personalised shear rate therapy is the induction of arteriogenesis – a rescue mechanism of the vascular system during occlusion or stenosis. It stimulates pre-existing but not fully developed collateral vessels across the entire coronary circulation to grow.
In a prospective study, 23 patients aged 61+2.5 years with stable coronary disease (CHD), and at least one haemodynamically relevant stenosis, were split into two groups. Sixteen patients in the therapy group received 35 one-hour treatment sessions of external counterpulsation over seven weeks; the seven patients in the control group did not. In the therapy group, the collateral flow index (CFlp) increased from 0.08 + 0.01 to 0.15 + 0.02 and the fractional flow reserve (FFR) also increased significantly from 0.68 + 0.03 to 0.79 + 0.03; P = 0.001; however, no change was observed in the control group [source: Eur J Clin Invest. 2009;39:866-75].
Tailored treatment
‘The extent of volume shift from the legs towards the heart is not really that important,’ Dr Buschmann explained. This also might be the reason why Cochrane and the FDA do not recommend an older system such as enhanced extracorporeal counterpulsation (EECP). Potential risks, in particular due to high pressures, can be harmful. However, it is not the compression ratio in the cuffs that is decisive, but the velocity impulse which results from the inflation of the cuffs. This impulse changes the flow profile in the blood vessels. The flow not only increases, but also the shear rate across the arterial walls. This sets off morphological and biochemical processes and eventually leads to a proliferation of the vessels [source: Development 2010].
That impulse is shown graphically on a novel vascular ultrasound ‘tachometer’ to measure blood flow, volume and pulse rate being developed in connection with the Herzhose® (literal translation heart pants – describing the cuffs system) which serves as a basis of calculation for the correct setting of this personalised shear rate therapy. Each treatment is individually adapted to the patient.
Given one-hour training sessions, the heart requires three to six weeks to develop the growth of natural bypasses sufficiently. This period of time depends largely on the individual blood flow acceleration of each individual patient, Dr Buschmann explained, adding: ‘We now know that the effect lasts for around a year, so repeated training is needed – an ideal passive addition to active cardio exercise.
Health insurers in Germany have started to cover this personal shear rate treatment, but not all; it has neither NUB (new examination and treatment procedures) status nor does it qualify for an additional reimbursement. Meeting the costs is always negotiated on an individual basis.
However, there is considerable interest. Apart from the Charité, another 20 clinics – in Germany, Austria and Switzerland – plan to offer this patent protected personal shear rate treatment this year.
The procedure is suitable to treat stable CHD and particularly diffuse CHD, i.e. patients who cannot be revascularised interventionally or surgically. In addition, patients with peripheral vascular disease (PAD) also benefit from the treatment, especially if they are also diabetics. Several clinical trials are currently being initiated to confirm the beneficial effects in larger patient cohorts.
The system can also be used to treat erectile dysfunction, a disease estimated to affect every other male over the age of 40 and which can frequently be a precursor of systemic vascular disease.
Profile:
PD Dr Ivo Buschmann studied medicine at the University of Hamburg, where he also began his career in the cardiology department with Professor Thomas Meinertz. Awarded a Max Planck Society scholarship he moved to Prof. Wolfgang Schaper’s group, where he participated in several high impact papers in the field of therapeutic arteriogenesis. With a grant from the Volkswagen Foundation’s excellency programme (2000 – 2006) Dr Buschmann continued his research at the Albert Ludwigs University of Freiburg. In 2004 his research group initiated the Richard Thoma Laboratories (RTL) for Arteriogenesis at the Charité Berlin in the Centre for Cardiovascular Research (CCR). The focus of the RTL is the generation of molecular experimental data and translation of the latter into clinical practice.
Clinically, Dr Buschmann directs the interventional angiology at the Charité Berlin (Campus Virchow) and is a founding member of ESVM – the European Foundation for Vascular Medicine.
03.09.2013