Peripheral arterial occlusive disease Long balloons are the gold standard
Every year, around 80,000 lower extremities in Europe have to be (partially) amputated as a result of peripheral arterial occlusive disease (PAOD). Half of the affected patients die within five years of the amputation.
As Dr Christina Plank, Consultant at the Department of Cardiovascular and Interventional Radiology, University Clinic for Radiodiagnostics, Medical University of Vienna, points out: ‘This is a very bad prognosis. Therefore, preserving the extremities is the primary objective in the treatment of peripheral arterial occlusive disease’
As in many other medical fields, surgical and radiological interventions are in competition here: The dangerous occlusion of the leg arteries can either be treated via bypass or through dilation of the occluded vessel. ‘With the treatment of critical ischemia in the lower thigh, dilation with a large balloon has developed into the gold standard,’ Professor Plank reported during the Interventional Radiological Olbert Symposium (IROS 2012) held in January in Salzburg, Austria. Compared to surgery, percutaneous transluminal angioplasty fares equally well, although the general state of health of many patients means that surgery cannot be carried out with a general anaesthetic. Moreover, fitting a bypass is expensive and also has more risks for the patients, she added. ‘When it comes to PAOD, it’s a case of giving priority to any treatment that can be carried out endovascularly.’
PAOD develops through a constriction or occlusion of the arteries that supply the extremities. Diabetes, generalised arteriosclerosis, high blood pressure, high cholesterol levels and obesity are the triggers of the disease, which is commonly divided into four stages: In the first stage the affected patient does not notice any symptoms resulting from the constriction or occlusion; during the second stage the person will have increasing difficulties walking; in the third stage critical ischemia develops and the lower thigh turns white and immobile, and during the fourth stage chronic wounds develop on the feet. In the pelvic area and in the upper thighs peripheral arterial occlusive disease is treated in stages 2 and 3; the lower thighs are only treated once the chronic lesions develop.
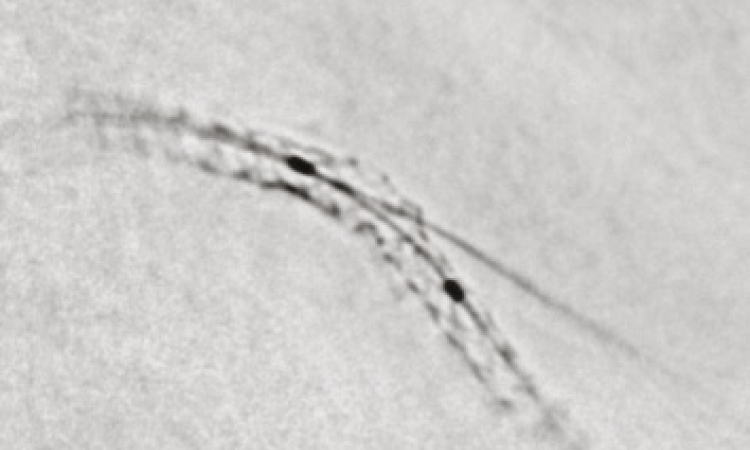
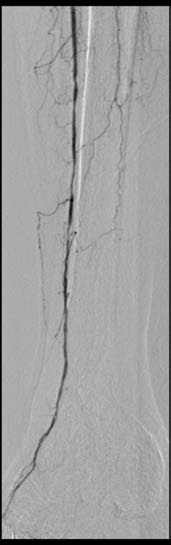
To heal these ulcers, which often necessitate amputation, the occluded blood vessels in the lower thigh are opened from the inside. Up to 22cm long, very thin, balloon catheters, which are inserted into the occluded area through the groin under local anaesthetic and then inflated with pressure, have proved very effective. ‘The occlusions in the lower thigh are mostly of long length and multi-segmental and can be dilated with long balloons in one go. This saves a lot of time,’ Prof. Plank explained, referring to the advantage of long balloons compared to conventional ones.
It takes two to five minutes to dilate a blood vessel. Any possible remaining short-length stenoses can be dilated straight afterwards with short, high-pressure balloons. Although this does not guarantee permanent revascularisation, the partial restoration of blood flow suffices to heal the chronic wounds. ‘Healing the ulcers is the primary treatment objective’ she stressed.
‘The use of long balloons to dilate vessels in the lower thigh is indicated when critical ischemia is present, i.e. when it is a case of preserving the extremities,’ confirmed Dr Florian Wolf, Consultant at the Department of Cardiovascular and Interventional Radiology, University Clinic for Radiodiagnostics, Medical University of Vienna, stressing: ‘The important issue is to bear in mind the principle of angiosomes.’
An angiosome is a block of tissue, all of which is entirely supplied by just one source artery. A foot consists of six angiosomes. Healing an ulcer therefore requires the opening of the exact vessel that supplies the affected area with blood, Dr Wolf explained.
* A satellite symposium held during IROS 2012, sponsored by medical devices manufacturer Cordis
23.02.2012