Article • Disruptive technologies
No way to stop the waves of change, but radiologists can learn to surf
Technological change is a major part of change management in radiology and it is inevitable. Artificial intelligence (AI) has slipped into every area of life including the hospital, and is already making decisions in radiology systems. The good news is that radiologists could win on two fronts, provided they play their cards well, a leading USA radiologist told delegates at a recent congress in Spain.
Report: Mélisande Rouger

Frank Lexa, a professor of radiology at the University of Arizona and recognised speaker on medical leadership, believes there is no way to stop the waves of change brought by disruptive technology including artificial intelligence (AI), but radiologists can learn to surf. ‘AI already helps us with scheduling and with image display protocols. Stopping technologic change is not an option,’ he told delegates at the Triángulo Radiológico meeting, held in Valencia in January.
Three types of technology have impacted on humans over the past hundred years. Incremental technology is an improvement of the existing technology and something of which radiologists are usually very fond. ‘It’s one of the reasons that I became a radiologist. Every year, things get better, CT scanners get faster, MR scanners have higher resolution and we obtain more information,’ Lexa explained. ‘But there is no change in customers and it doesn't displace any other technology.’ Transformative technology, on the contrary, is where one technology replaces another due to quality, performance and/or cost advantages. The cassette player, for example, replaced the vinyl record, and later was replaced by digital music.
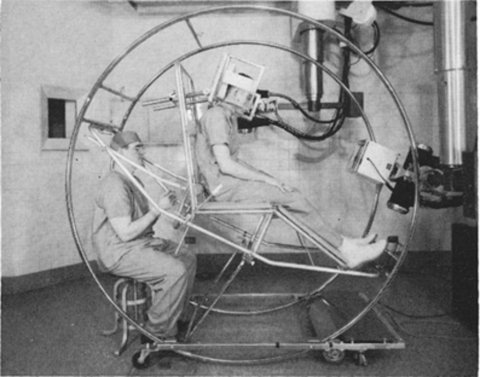
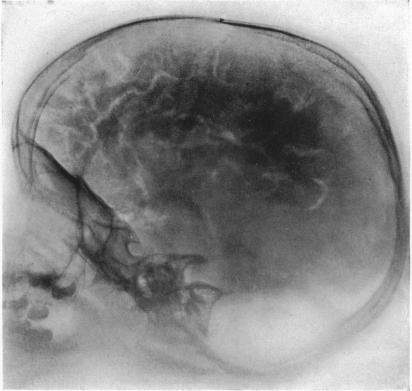
In radiology, many technologies have replaced others in the blink of an eye (5-10 years). The pneumoencephalogram is something most radiologists have never heard of, yet it was all the rage just over 40 years ago. ‘It looks like somebody who is training to be an astronaut. In the US, CT almost immediately replaced the pneumoencephalogram. Some people used it for amusement through the holidays, but they were no longer using it for patients. In the space of a couple of years, it was completely replaced,’ Lexa pointed out.
AI is part of disruptive technology, which, as first described by Clayton Christensen and Joseph Bower from Harvard University (Disruptive Technologies: Catching the Wave, Clayton Christensen and Joseph Bower, Harvard Business Review, 1995), consists of adopting an innovation that is lower cost and lower quality. ‘It's often worse quality, but it changes the market and expands it. Disruption changes who the market is and how you work,’ Lexa explained. This happened to radiologists when imaging systems were developed for non-radiologists. Many ultrasound machines created recently have worsened image quality, but made the technology more available to all medical specialists. ‘How many years did some people train, including myself, to learn how to use ultrasound? Now, it's like a stethoscope. Everyone who goes through medical training now thinks that they can do ultrasound; that's a true disruption,’ he pointed out.
Another example is the extremity MR system, which produces worse images than a traditional MR scanner launched 20 years ago. Physicians buy worse, but more affordable equipment. ‘You can put this anywhere. You don't need to block out the rest of the building; it's cheap, and means you can pretty much have MR wherever you want.’
A lot of disruptive technology gets better after some time. This is happening with ultrasound, small mobile CT scanners and, soon an MRI system, will fit in the back of a car, Lexa predicted. ‘Anyone who doesn't believe me, anybody who wants to take that bet, I'll have dinner in Chicago with. Prepare for it!’
In spite of all the disruption, the traditional value that only the radiologist does the consultation, supervises imaging, interprets and does form of management has not been broken up. However, with AI tools improving at the speed of light, it’s unclear whether radiologists will keep on playing this role. It’s only natural that they feel threatened by AI. ‘I'm scared by AI as well. It does make me wonder sometimes what we're training for,’ Lexa exclaimed.
‘The future belongs to the brave’
If you don't like being reviewed by other humans, I don't know how much you're going to like being reviewed by a robot. This is not something that's deep in the future. This is all happening now
Frank Lexa
In the future, more and more machines that allow non-radiologists to do imaging will emerge, and also more machines that don't need a technologist to be used. Machines that provide a preliminary read are already available. Computer systems that can extract information from imaging scans that human eyes and brains can’t easily see are also already available. Right now, in the USA, the most popular thing for residents is intervention, and part of this is the worry that it's going to be easier for software algorithms to do most of the rest of diagnostic radiology. However, robots will also assist or perform interventional procedures.
AI systems that can aggregate genomic imaging and clinical information are already available, and so are phone apps that will read a chest X-ray and AI systems that can do peer review for radiologists. ‘If you don't like being reviewed by other humans, I don't know how much you're going to like being reviewed by a robot. This is not something that's deep in the future. This is all happening now.’ The challenge for radiologists is how do they deal with these new scenarios? First, they must face that issue. ‘If rads don't face it, non-radiologists will. The choice for us, is change or be changed, disrupt or be disrupted, lead or be led,’ Lexa advised.
Radiologists should make the most of disruptive technology. The optimistic solution will be to leave the sorting out of cases and eventually the boring cases to the computer, so that radiologists only read the interesting ones. ‘A computer that ensures I don't make a mistake because it has high sensitivity, I would like that, particularly if it's late at night and if I'm working too many cases that day.’ Rads can ‘merge’ with computers to become ‘centaur radiologists’, a combination that would help them have the best of both worlds. ‘It's the notion where you have a horse's body and a human's upper body, a computer and a radiologist working together to read the images.’ Building value will prove essential to the task, and so will the attitude, Lexa believes. ‘The future belongs to the brave.’
Profile:
Frank J Lexa MD MBA FACR is an academic neuroradiologist and currently a professor and Associate Chief and Vice Chair of Strategy and Leadership, in the Department of Medical Imaging at the University of Arizona. In his book ‘Leadership Lessons for Success in Health Care’ he takes a systematic approach to developing medical leadership skills.
26.02.2019