Article • Imaging investigation and diagnosis
Multiparametric ultrasound: the future of the modality
Multiparametric ultrasound will play an increasing role in imaging investigation and diagnosis as more subspecialities reap the benefits from the modality, Professor Paul Sidhu believes. The leading expert predicts that it will be more cost-effective and comfortable for patients and take point-of-care-testing onto a new level by embracing other parameters in the imaging process.
Report: Mark Nicholls

Photo: supplied
Professor Sidhu discussed the benefits, advantages and advances of multiparametric ultrasound over other modalities as part of his presentation “The future of ultrasound” at the British Institute of Radiology congress in London in late September. The expert, who is Professor of Imaging Sciences at King’s College London and consultant radiologist at King’s College Hospital, outlined the history of ultrasound and its evolving clinical use, and suggested that radiologists are “losing interest” in preference to other imaging modalities.
He pointed to sonographers and other subspecialty clinicians – such as obstetricians, gynaecologists, cardiologists, and physiotherapists – increasingly using ultrasound, and particularly multiparametric ultrasound. Point-of-care ultrasound, Sidhu notes, is used in A&E departments, and in medical schools as part of the curriculum for students to learn anatomy. He discussed how radiologists prefer MRI and CT, and in the UK perform only about 8-10% of ultrasound scanning, with the rest conducted by sonographers.
‘Using ultrasound to its full potential’
Ultrasound is practised elsewhere in the hospital, away from radiology departments, Prof Sidhu notes, seeing this development as a continuing trend. ‘In Europe, and in Germany in particular,’ he said, ‘ultrasound is used by many subspecialists: renal physicians, urologists, hepatologists, gastroenterologists, and general practitioners. It is not radiology-based, more is done by non-radiologists.’
So, how will the modality fare in a “radiology” context? The expert believes multiparametric ultrasound is the major evolution, measuring more than one parameter. ‘Other subspecialties outside radiology embrace multiparametric ultrasound much more than radiologists do,’ he said, ‘and are using ultrasound to its full potential.’
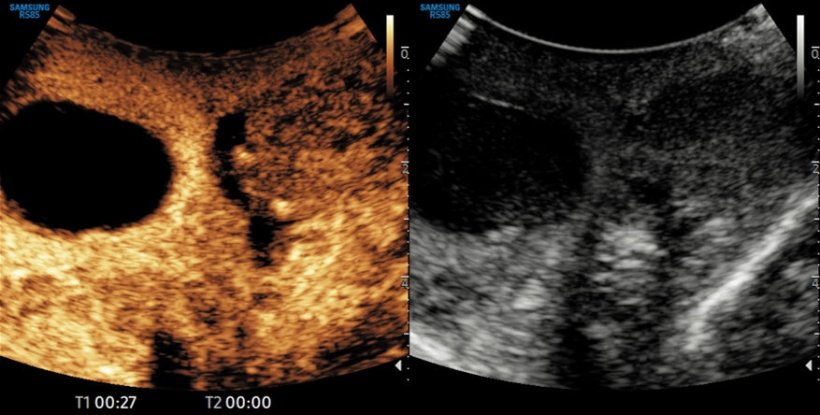
Image source: Prof Sidhu
An undersold modality
Prof Sidhu, who first coined the phrase multiparametric ultrasound a decade ago, believes that ultrasound is undersold, particularly in comparison to MRI, where investigations are also being termed as multiparametric. ‘Ultrasound is the pioneer in multiparametric imaging because you have B-mode, but there is also colour Doppler, spectral Doppler and power Doppler. Microvascular imaging gives imaging down to capillary level using very sensitive Doppler, while contrast-enhanced ultrasound has the ability to look at time intensity curves, wash-in and wash-out curves, and look at areas under the curve, assessing haemodynamics of the structure under investigation. This can monitor tumour response much more accurately than CT or MRI, is much cheaper, and it is better for the patient as well as they do not have to undergo a potentially invasive or uncomfortable investigation.’
Multiparametric imaging of the liver will become a one-stop clinic with every possible parameter imaged, recorded, and quantified using ultrasound; this is multiparametric at its premium
Paul Sidhu
In addition, he points to ultrasound with elastography to measure stiffness in the liver, and how the different techniques of elastography, including point and 2D shear wave, are useful in liver assessment and liver fibrosis. ‘Strain elastography gives a colour map of the areas of hardness,’ Sidhu said. ‘There are also techniques which quantify fat levels in the liver to the same level of accuracy as MRI but at a fraction of the cost and this will revolutionise imaging of the liver in the future. Multiparametric imaging of the liver will become a one-stop clinic with every possible parameter imaged, recorded, and quantified using ultrasound; this is multiparametric at its premium. Multiparametric is the strength of ultrasound imaging, and that is also the future for ultrasound. It brings all the techniques under one umbrella.’
Point-of-care imaging brings physicians closer to the patients
Patients benefit because the modality can be applied ‘quicky, smoothly, painlessly and accurately’ and physicians can be next to the patient to offer reassurance, Sidhu explained. He pointed to the example of finding a focal live lesion in a patient referred from primary practice, where findings are benign in 9 out of 10 cases. ‘Using contrast-enhanced ultrasound, you can make the diagnosis without uncertainty within 2-3 minutes and tell the patient that they have a benign lesion and they are fine, instead of waiting three months for a clinical appointment.’
Another advantage is the miniaturisation and quality of the ultrasound machines, and the ability to use a smartphone or tablet to perform an ultrasound examination. This transfers ultrasound to the point-of-care physician to diagnose at the bedside at minimal cost, maintain close contact with the patient, as opposed to CT or MRI, with that closer interaction with the patient at the time of examination making the diagnosis more secure.
Profile:
Paul Sidhu is Professor of Imaging Sciences at King’s College London and consultant radiologist at King’s College Hospital. His research interests include contrast-enhanced ultrasound, non-invasive liver imaging and dose reduction in children. He is an ex-President of the British Medical Ultrasound Society and European Federation of Societies in Medicine and Biology. He is Editor-in-Chief of Ultrasound in Medicine and Biology.
01.12.2022





