Molecular US therapy, computer diagnosis and customized medication
Renowned Experts Discuss the Future of Medicine in Bremen
Which technological advancements can we expect to see in the field of medical technology? How well can diagnosis and therapy be customized for each patient?
And how much automation can medicine handle? To help answer these fundamental questions, the Fraunhofer MEVIS Institute for Medical Image Computing will hold a symposium entitled “Disruptive Innovations in Medicine” on September 4, 2013 at Jacobs University in Bremen. The occasion for the symposium is the farewell of Prof. Heinz-Otto Peitgen, founder and long-time institute director of Fraunhofer MEVIS.
Medical science is at a point of transition. Established diagnostic methods such as ultrasound, X-ray, and MRI are continually being improved. These methods can now deliver extremely detailed imagery and information. In addition, new methods are constantly being developed, including the combination of MRI and PET scans for cancer diagnosis. At the same time, the spectrum of therapy options is always growing: new medications for specific patient groups are now being marketed. Operating room methods are becoming more refined, and the number of minimally invasive intervention options is ever expanding.
However, these advancements carry enormous demands and these new options increase complexity. Next-generation CT and MRI deliver images with data size many times those made by older devices. In addition, a current trend is to combine the images and information from many different methods to obtain more reliable diagnoses. This results in a true flood of various image data. “These data gluts reach the limits of what even specialized clinicians can absorb in their daily routine,” says MEVIS institute director Horst Hahn. “Often, they are barely able to incorporate all available information into their therapy decisions.”
In the future, computers could offer useful support. Researchers have already developed programs to employ patterns to search lung and breast x-rays, helping doctors during early detection of cancer. Preliminary studies have shown that the abilities of computers using pattern recognition often match those of humans, or, as in the case of suspected microcalcification in mammography, exceed them.
There are still outstanding problems to solve in computer-aided diagnosis (CAD), such as the number of false alarms. Experts also estimate that the growing amount of data will not be able to be handled without the use of intelligent diagnosis software. “We are not seeking to replace doctors with machines, but rather to create an optimal team of both humans and computers,” said Hahn. “Computers and humans feature contrasting strengths and weaknesses, requiring us to think broadly about how much automation is reasonable for medicine.”
A further focus of the symposium is ‘personalized medicine.’ Until now, this has meant using genetic testing to find out whether a patient could benefit from a certain medication. However, it is now becoming clear that diagnostic methods can be customized for individual patients or certain symptoms, as seen in positron emission tomography (PET), a highly sensitive method used in tumor detection. To mark tumor cells, only a small amount of 'tracers' are presently used.
In laboratories, experts have already developed a number of tracers, although these must still pass extensive approval procedures. This growing array of options is also available in other fields of image-based diagnosis. However, these stand in opposition to the efforts of medicine to verify every new method based on large, randomized studies. "Thus, we must thoroughly reflect upon a responsible approach towards the quickly growing spectrum of diagnostic and therapeutic options and which roles computer support could play," said Hahn.
Finally, the session will tackle new and revolutionary therapeutic approaches for radiotherapy and particle therapy, among others. The novel term 'theranostics' is now being used to describe the close relationship between diagnosis and therapy in a combined, patient-specific approach.. An even newer method directly links ultrasound diagnosis and therapy. Using this method, clinicians administer a special ultrasound contrast medium to the patient to record imaging of an organ, such as the kidney. The contrast medium serves not only to help depict tumor tissue, but also to deliver the medication.
The moment an image shows an abscess, the clinician could use a focused ultrasound signal to burst the microscopic bubbles that make up the contrast medium. This would discharge the medication that immediately surrounds the tumor, providing organ-preserving therapy with few side effects. "These new types of therapy are very promising," said Hahn, "but we must thoroughly investigate each new method to determine whether their benefits truly affect the clinical routine and whether they are economically feasible."
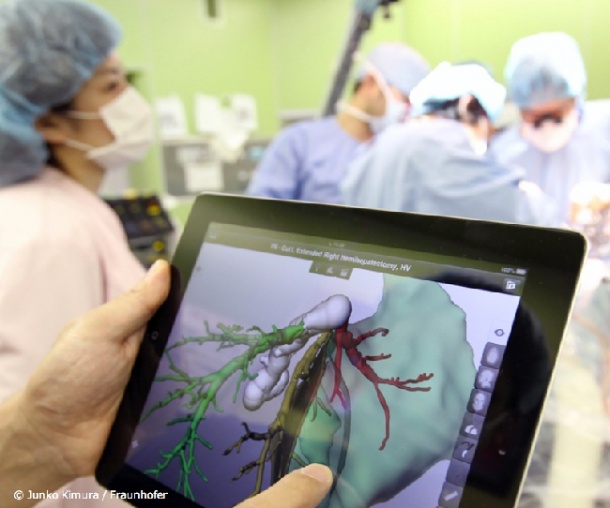
On the day following the symposium, the event will move to the MEVIS's institute facilities. Interactive demonstrations by MEVIS researchers will clearly demonstrate how the computer support of the future could take shape for fields such as breast cancer, lung, and stroke diagnosis as well as navigated, minimally invasive tumor therapy. A further demonstration will feature a new tablet app to support liver operations. In August, this app was tested for the first time during an operation in Germany. Media representatives are welcome to attend.
September 4: Symposium - "Disruptive Innovations in Medicine" at Jacobs University.
September 5: Open House at Fraunhofer MEVIS, 9 to 13:30. Visitors are very welcome to attend.
28.08.2013