Medical devices are not scrutinised enough
Investigators call for tighter regulatory controls
Report: Brenda Marsh
United Kingdom – A call has been made for tighter regulatory controls to ensure the safety regulation of medical devices, following joint investigations carried out by the British Medical Journal and the Channel 4 TV programme Dispatches, which were televised and published online at BMJ.com this May.
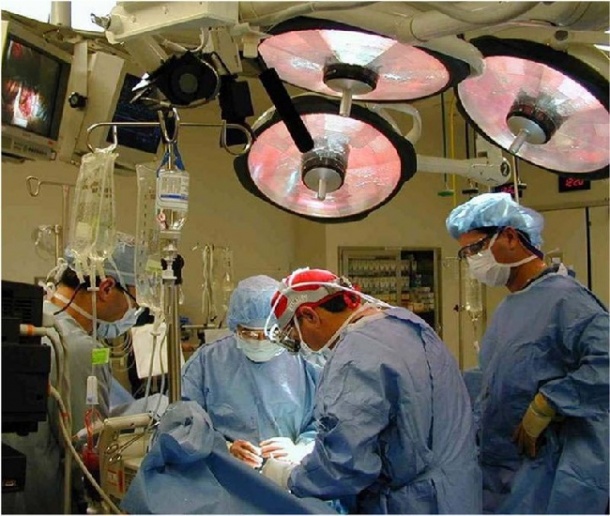
According to the investigators, thousands of people face painful and expensive surgery to remove failing medical devices such as metal hip replacements and cardiovascular implants.
They raise serious concerns about the regulation of medical devices and ask how well these high-risk devices are tested before they come onto the market.
The investigators explored a European approval process negotiated by private companies behind closed doors and revealed a worrying lack of public information about the number of devices being used and their potential risks.
They also discussed links between surgeons paid to design devices and the companies promoting them.
‘The investigations findings are clear: The current system is not fit for purpose and we urgently need better regulation to protect patients,’ the investigators state.
There are thousands of medical devices on the market and, worldwide, the industry is worth over £200 billion a year. Yet, the investigators report, the approval process is far less stringent than for drugs, particularly in Europe. ‘What’s more, it is the manufacturer’s responsibility to monitor the performance of their devices once they are on the market. But rather than have large post-marketing studies, manufacturers may rely simply on doctors and patients to report problems. And,’ they add, ‘there is no publicly available central register of adverse effects to allow early detection of emerging problems.
The Dispatches programme revealed examples of failing devices that have remained on the market, despite companies being aware of problems. In the case of articular surface replacement (ASR) metal hip implants, the manufacturer, Depuy, waited until 2010 to take its hip fully off the market, despite repeated warnings from doctors as early as 2007, the investigators point out.
Other examples include the case of a patient who had a combined pacemaker/defibrillator fitted in his chest that misfired over thirty times in one day. The manufacturer recalled it after reports of five deaths and well over 600 reports of a broken component inside the device.
The programme also revealed another emerging problem with artificial hips, this time with large head metal on metal implants. Some surgeons are now raising concerns about these. Whilst one manufacturer has agreed to fund costs associated with the recall of its ASR hip, it is unclear who will pick up the bill for this new looming health crisis if all large diameter metal on metal hips require revision operations,’ the investigators point out.
When the BMJ/Dispatches team asked companies for data to support the safety and effectiveness of their devices, access was denied on the grounds that it was ‘company confidential information’.
Even Freedom of Information requests made to the UK regulator, the MHRA, for data on adverse events for two different kinds of hip implants and one model of cochlear implant were refused as ‘overriden by medical device legislation’.
The MHRA has concerns about the lack of transparency and variable standards in the current system, but they said, ‘if we were to inhibit innovation by imposing a more burdensome regulatory regime we would have to have some extra evidence that the burden actually provided a greater degree of patient safety’.
‘This story shows the power that companies have in deciding the fate of their devices, their hold over surgeons, the lack of regulatory power in Europe, and the lack of premarket clinical studies that may well have picked up some of these problems earlier,’ said Dr Deborah Cohen, Investigations Editor at the BMJ. ‘We have still not learned from past failures,’ she added.
‘Nearly 20 years ago, the BMJ highlighted the dangers of early failure of unproved implants, yet the NHS is currently picking up the bill for faulty devices,’ Dr Cohen pointed out. ‘Unlike kettles and toasters, which come with warranties, when devices do not last as long as they ought to companies are not necessarily held financially responsible.’
Dr Carl Heneghan, a GP and Clinical Reader at the University of Oxford added: ‘Patients should have access to the evidence about the nature of their devices, the true benefits, the true harms. At the moment that’s not happening and patients are acting as guinea pigs and that’s not good enough.’
Professor Nick Freemantle at the University of Birmingham agreed ‘Rather than devices being subject to an inferior regulatory model, we should extend and strengthen the approach taken for pharmaceuticals,’ he said.
* Investigation contributors included Dr Carl Heneghan, Director of the Centre for Evidence-Based Medicine & Clinical Reader, University of Oxford; Nick Freemantle, Professor of Clinical Epidemiology and Biostatistics, University College London; Tony Nargol, Orthopaedic Surgeon, University Hospital of North Tees, Hartlepool; Alan Fraser, Reader in Cardiology, Wales Heart Research Institute, Cardiff University; David Langton, Surgical Registrar and Researcher, University Hospital of North Tees and Newcastle University; Peter Wilmshurst, Consultant Cardiologist, Royal Shrewsbury Hospital.
Picture Credit: Smith & Nephew
16.06.2011





