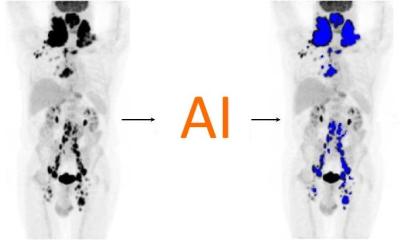
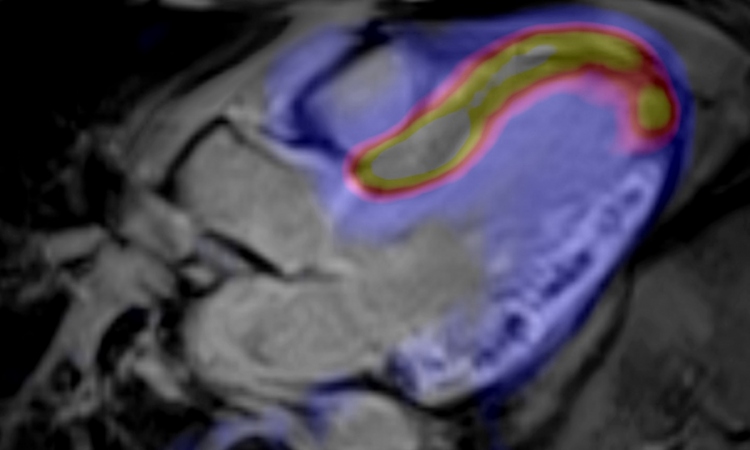
Hybrid imaging: Virtual FDG-PET/CT bronchoscopy
Virtual FDG-PET/CT bronchoscopy has been found to be a technically feasible tool for the detection of lymph node metastases in non-small cell lung cancer patients with good diagnostic accuracy, according to researchers at the Department of Diagnostic and Interventional Radiology, University Hospital Dusseldorf and Essen.

The team has been clinically evaluating a newly developed software application from Siemens Molecular Imaging and using a Siemens scanner equipped with a 2x64 slices CT scanner and high-definition PET for their research. Senior radiologist and team leader Dr Till Heusner, said: ‘This new tool enables physicians to virtually fly-thru the bronchus system from PET/CT scans and to see “hot spots” resulting from bronchial carcinomas or lymph node metastases underneath the morphological surface. Without the functional PET information, meaning by CT morphology only, these malignancies would not be detectable on a virtual fly.’
A factor in pursuing this line of research by the Dusseldorf radiology team, which collaborated with the University of Essen radiology and nuclear medicine departments, was the need to offer clinicians the most axially displayed radiologic information possible. ‘This may help them to more realistically plan interventions such as bronchoscopy-guided biopsies,’ Dr Heusner explained. FDG-PET/CT is an imaging modality in which a PET scanner and CT are installed ‘in line’ with FDG – a radioactively labelled glucose molecule – injected intravenously prior to the investigation. This accumulates in the vast majority of tumour cells and shows radiologists where tumour deposits are located in the body.
The researchers found that the software application was almost ready for clinical use. ‘It runs in a robust way and reaches a high diagnostic accuracy when it comes to the detection of FDG avid parabronchial or paratracheal lymph node metastases in nonsmall cell lung cancer patients. Even relatively small bronchi in the periphery of the lung can be reached by the virtual fly-through,’ said Dr Heusner, whose sub-specialities are hybrid imaging and interventional – vascular and oncologic – radiology, and who heads the university hospital’s oncological hybrid imaging working group.
Hybrid imaging is growing in importance all the time regarding primary staging, follow-up and early therapeutic control in a range of malignancies, he pointed out, adding that the next step from the FDG-PET/CT work is to look at MR/PET and the improved soft-tissue contrast it can offer. ‘One of the big advantages of hybrid imaging is the possibility to detect very early lymph node metastases. This mainly is the merit of PET – it is able to show us little amounts of tumour deposits when morphological findings suggesting malignancy are still missing. Since PET alone often cannot precisely locate lymph node metastases, the combination of PET/CT as well as MR-PET now can precisely tell us where the lymph node is localised.’ The technique allows radiologists to become much more confident in diagnoses and helps triage patients to the ‘most adapted, personalised therapeutic strategy to their disease stage’ and may enhance survival chances.
A range of other papers was presented during the session ‘Hybrid imaging: PET-CT and MR-PET’. Dr Paoletta Mirk (radiology department, Catholic University of the Sacred Heart, Rome) outlined her team’s work on the ‘additional value of dual-phase 18F-FDG PET-CT in recurrent gynaecological malignancies.’ They compared this with standard PET-CT and found it had higher sensitivity and higher accuracy. Dr Kazuhiro Kitajima (Department of Radiology, Kobe University), and team, compared low-dose non-enhanced CT with full-dose contrast-enhanced CT in integrated FDG-PET/CT studies to diagnose ovarian cancer. They discovered that PET contrast enhanced CT is an accurate modality to assess ovarian cancer recurrence.
A team from Padua, Italy, found that PET-CT was more accurate than CT in the detection of bone marrow metastases, while German researchers at the University of Tubingen showed that contrast-enhanced CT improved malignant lesion classification.
02.05.2012