Connected to Heart
Fetal surgery successfully removes life-threatening tumor
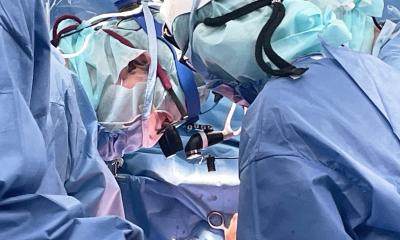
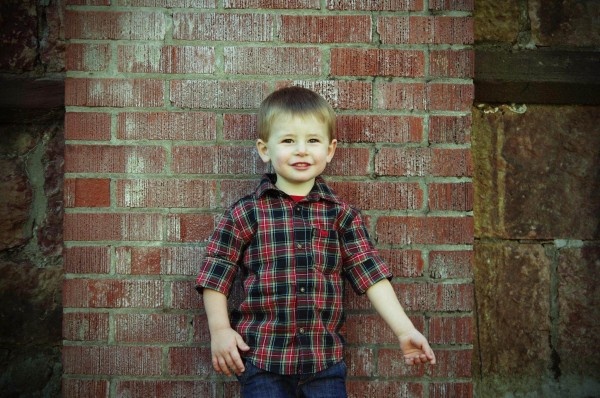
For the first time, fetal medicine experts have performed prenatal heart surgery to remove a life-threatening tumor, called intrapericardial teratoma. The patient, who underwent the operation at 24 weeks of gestation while in his mother’s womb, is now a healthy three-year-old preschooler. “We have shown that we can accurately diagnose and provide a prognosis for this rare condition in utero, as well as perform fetal surgery,” said co-study leader Jack Rychik, MD, director of the Fetal Heart Program at the Children’s Hospital of Philadelphia (CHOP).
Rychik, along with co-study leader Nahla Khalek, MD, of the Center for Fetal Diagnosis and Treatment (CFDT) at CHOP, and colleagues, recently published their findings online in the American Journal of Obstetrics and Gynecology. The research team, from CHOP and the Perelman School of Medicine at the University of Pennsylvania, reported a case series of eight fetuses with suspected intrapericardial teratoma seen at CHOP between 2009 and 2015.
Intrapericardial teratoma is an extremely rare, rapidly growing tumor that can be detected during the fetal period. Arising in the pericardium, the sac surrounding the heart, it is lethal if untreated. The current prenatal strategy is to drain pericardial fluid to buy time for the fetus to grow to a viable gestational age, followed by surgery to remove the teratoma shortly after delivery. However, rapid prenatal growth of the tumor, along with fluid around the heart, which inflicts dangerous pressure on the heart, lead to disruption of normal fetal circulation and fetal death.
Therefore, an ideal treatment is to perform surgery prenatally, before cardiac dysfunction occurs. The CHOP team is the first to perform this prenatal surgery resulting in a healthy live born neonate.
The case series in the current study covers eight fetuses evaluated for suspected intrapericardial teratoma at CHOP, two of whom were found to have other types of heart-related tumors. Of the six cases with intrapericardial teratoma, two survived, both following surgery. One underwent open fetal surgery at 24 weeks gestation, while the other underwent successful EXIT (ex utero intrapartum treatment) procedure at 31 weeks gestation. In the EXIT procedure, surgeons partially deliver the baby through an incision made in the mother’s uterus and perform surgery while the baby remains connected to the placenta.
Of the four cases of intrapericardial teratoma who died, none underwent fetal surgery, in some cases because referral was late and the fetuses were too sick to benefit from intervention. “Managing this type of teratoma presenting before birth is a challenge, but we show that survival with good outcome may be possible in some patients,” said Rychik. “It was the ability to bring so many different disciplines to the table that made us confident enough to take the leap to offer in-utero surgery on a fetal heart as a viable option,” added Rychik.
“The current era offers technological advantages, such as improved prenatal imaging, improved cardiovascular surveillance through fetal echocardiography, and fetal surgery techniques,” said co-study leader Nahla Khalek, MD, a maternal-fetal medicine specialist in the CFDT. “A crucial factor is implementing treatment before fetal heart failure occurs. Our findings underscore the importance of promptly referring these cases to a multidisciplinary fetal therapy center during the optimal window of opportunity for both the fetus and mother.”
“Removing a tumor from a baby’s heart in-utero present significant risks for both the mother and the baby. Timing and coordination early in the illness is vitally important,” added co-author Holly L. Hedrick, MD, attending pediatric and fetal surgeon in the CFDT. CHOP’s fetal surgeons, who have performed more than 1,350 in utero surgeries, are highly experienced in reducing those risks; their work has helped make complex prenatal surgery an option for a growing number of fetuses diagnosed with birth defects.
“The pioneering fetal surgery to remove a tumor from a baby’s heart is an incredible breakthrough and an innovation in the care that can be provided to a family who receives this devastating diagnosis,” said co-author J. William Gaynor, MD, a pediatric cardiothoracic surgeon at CHOP. “We need to constantly ask new questions and take our work in new directions by bringing the top experts in their fields to counsel and provide state-of-the-art care to our mothers and babies.”
Source: Children's Hospital of Philadelphia
31.10.2016