Europe’s pressing need for transcultural competence
Patients with a migration background can create underestimated difficulties in healthcare systems in Western countries.
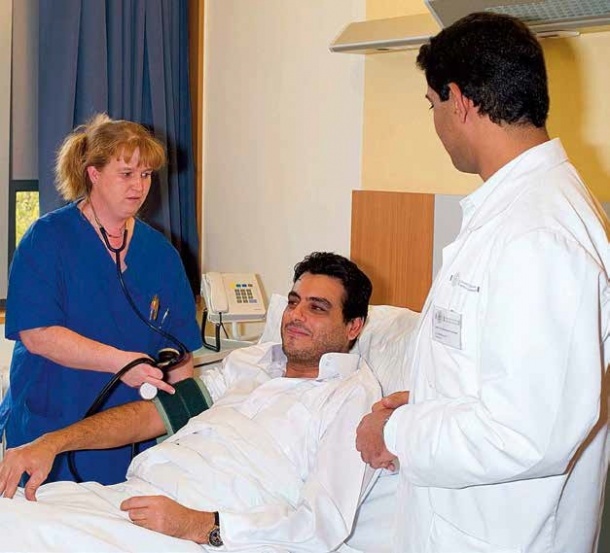
The issue is not merely a lack of language skills – interpreters can help – but the entire cultural, religious, social and therefore also psychological background of these patients.
Ostensibly, language barriers affect medical care and treatment, beginning at a general practitioner’s (GP) surgery. Many intercultural studies have revealed a multi-layered, complex connection between migration and health. Results from pain therapy, for instance, show that patients with a migration background are at risk of receiving insufficient treatment.
The language barrier also leads to non-observance of follow-up examinations and appointments, a larger number of diagnostic examinations being carried out, lower therapy compliance as well as lower patient satisfaction. Language problems result in significant healthcare costs, due to longer hospital stays, for example.
Trans- or inter-cultural competence in a hospital is therefore a health-political mandate that healthcare institutions should satisfy, so that migrant patients also receive the best possible care. However, this is about more than language problems.
At the 11th European Healthcare Congress in Munich, the German-Turkish Health Forum focused on the fact that mainly cultures dominated by religion need a different approach to illness. In hospital, this begins with food requirements, the observance of prayer times and a different way of relaying negative diagnostic results.
Women are also subject to different treatment criteria than men. The need, therefore, is not so much for an interpreter service, but for inter-cultural training for healthcare workers. To that end, an increasing number of workshops and seminars are on offer. However, at the congress, Dr Fuat S Oduncu MA EMB MBA, Head of Haematology and Oncology at the Medical Clinic and Policlinic IV in Munich University Hospital, emphasised that migrant patients always receive treatment based on Western European knowledge – and that a change of perspective is needed.
Knowledge helps healing
The medical staff needs inter-cultural competence to help understanding of migrants patients’ worlds. The number of multinational teams in healthcare is increasing. Knowledge of religious aspects and aspects of everyday life, along with awareness of one’s own cultural views is essential.
More and more hospitals provide foreign language hotlines and multilingual information brochures about the hospital as well as brochures published by pharmacological companies and medical device manufacturers. Employees from different countries and lay interpreters act as points of contact.
In seminars for inter-cultural competence, staff can learn more about the religious background and cultural customs of Muslims. They are, for instance, taught that the face of a deceased Muslim needs to be positioned to face towards Mecca – i.e. Southeast – immediately upon death. Specific rituals during birth are also explained. Germany is not the only country increasingly trying to accommodate the needs of Muslims in this way. In the USA, for example, the River-View Hospital in Detroit has succeeded in accreditation for ‘Islamic Health and Human Services’ by the Islamic Healthcare Service.
However, the debate continues over whether there should be Islamic hospitals in Western Europe in the future. The affected target group appears to have very different views.
Studies have shown that increased stress amongst migrants manifests itself as psychosomatic illnesses. Conversely, studies have shown that patients who feel understood and can communicate have a significantly higher chance of being cured – and surely this is what it should be about for all involved.
08.01.2013





