Article • Minimally invasive
Computer Assisted Surgery: navigation leads to completion
Computer Assisted Surgery (CAS) has made its way into a variety of surgical disciplines. The term includes concepts that support surgical interventions with the use of computer technology from the preoperative to the postoperative phase. This comprises image-guided surgery as well as surgical navigation systems or the more critically viewed robot-assisted surgery.
Report: Melanie Günther
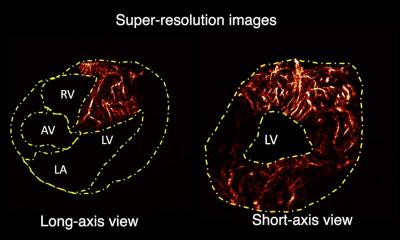
High-resolution data sets in the millimeter range can be reconstructed three-dimensionally.
Professor Markus Kleemann
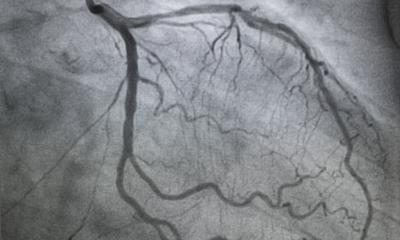
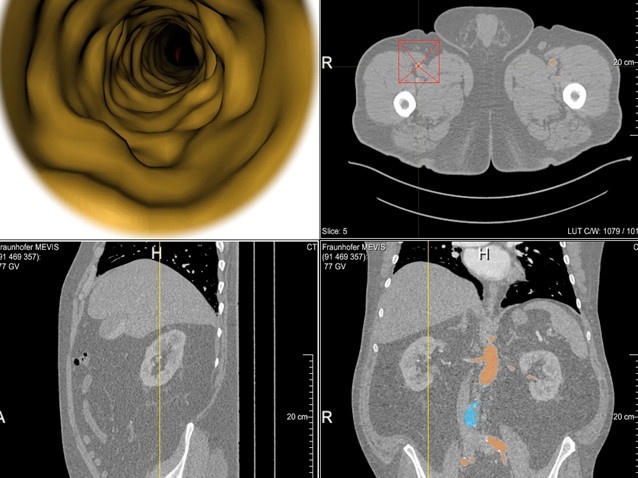
The basic prerequisite for CAS is an accurate model of the patient. To accomplish this, various image formats - whether it’s CT, MRI or PET/MRI scans- are prepared and combined with the help of software during the preoperative planning phase. Professor Markus Kleemann, Division Chief of Vascular and Endovascular Surgery at the University Medical Center Schleswig-Holstein, explains. “High-resolution data sets in the millimeter range can be reconstructed three-dimensionally. This image is subsequently transferred to the patient. The reconstruction conveys a more intuitive view of the findings, for instance, regarding the location of a tumor or vascular disease. Thanks to this visualization technique, today we have the chance to calculate distances, diameters or volumes prior to the intervention and accurately specify the surgical strategy.” The implementation during the surgery assumes that the information collected from the image data can be transferred to the surgical settings.
In some cases, a 3D model of the operable organ or bone is produced after the image reconstruction. In doing so, stents or implants can be positioned on a trial basis or accesses simulated to be able to operate as minimally invasively as possible. Based on these types of custom-made models, implants can also be custom-fit in some instances.
CAS is primarily used in specialized clinics since the technique only lends itself to more complex cases. The generated CAS data can be transferred between individual clinics and hospitals. This is important in patient transfers or teleradiology consulting when the goal is to save time and gain information.
From preoperative planning to navigation
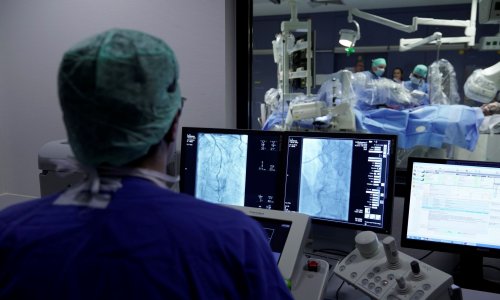
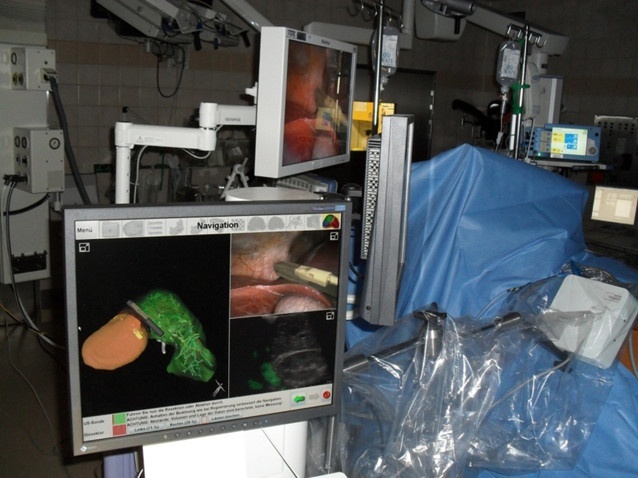
Minimally invasive surgical procedures have considerably increased in recent years and have also become gentler and more accurate. That’s why it is certainly no coincidence that the development of CAS as a navigation aid went along with the refinement of minimally invasive procedures. Surgical navigation systems give surgeons access to structures that would not be accessible without navigation. And they also enable them to work with more precision – all of it benefitting the patient.
Navigation systems are based on optical or electromagnetic tracking systems. Prof. Michael Nerlich, Director of the Department of Trauma Surgery at the University Medical Center in Regensburg, works with 3D stereo cameras in his specialty area. “The sensors of the camera system facilitate a precise spatial presentation that is directly transferred onto the screen. As a surgeon, I can see exactly where I am presently at with the respective instrument. This is especially helpful with spine surgeries where every millimeter is crucial. Thanks to the navigation aid, screws, wires or implants can be put in place by using minimally invasive techniques. “
Today’s commercially available navigation systems often use optical and electromagnetic tracking and combine the benefits of both techniques. The differences between interventions can be the mathematical model data set by which the tracking data is synchronized, that is to say, “registered“.
The University Medical Center Schleswig-Holstein currently studies the use of fiberglass navigation systems for vascular surgery. “Within the scope of further developing minimally invasive endovascular procedures, we try to subject patients to less radiation and contrast agents. Thanks to the integrated fiberglass in the catheter system, we are able to control the position based on intraoperative imaging and know exactly where our catheter is located in the vascular system, “adds Kleemann.
Navigation as a self-learning system
Yet even navigation systems sometimes reach their limits, namely when complex procedures are necessary that the software does not contain in its programming. “The systems are often geared towards standard procedures and cannot be used for complex malpositioned knee or hip prostheses. This is why it would obviously be desirable if these systems could act in a self-learning manner in the future based on artificial intelligence, “adds Nerlich.
Nerlich could also imagine for systems that are customized to the weaknesses and strengths of a surgeon to triumph. They could warn surgeons if the movement fluctuates. “Currently, there are studies on knowledge-based systems that adapt to the individual surgeon and allow for a customized surgical technique. There is still a wide, expandable potential for development in the CAS sector. “
Man vs. machine
Besides surgical navigation systems, robot-assisted surgery is another field that’s not new. Kleemann clarifies, “The misconception about robotic surgery is that the robot automatically performs surgery. That’s not quite the case. These are actually so-called master-slave robot systems with a surgical console and a patient-side cart with three or four robotic arms that ultimately performs the movement. “
The best-known system is the Da Vinci telerobotic surgical system, though there is no conclusive scientific data that proves an explicit benefit of the device for the patient, according to Kleemann. The high costs call for a clear marketing strategy. Nerlich also agrees with that statement. The “granddaddy“ among systems should have actually been revised and updated some time ago. According to Kleemann, newer developments are actually headed for haptic feedback as is the case with the MiroSurge robotic system, a research project by the German Aerospace Center; yet this does not solve the cost-benefit issue. “Although patients are very attracted to this technology, I don’t believe that the surgical profession will someday be replaced by robots.“ He adds that an evidence-based data analysis and facts that prove an actual benefit are still missing.
09.08.2016