Blown Away!
Even though a lot of us don’t do it, let’s say you know that washing your hands is the first, and the best thing, you can do to stop sharing nasty bugs that are especially dangerous for patients.
And you know you should use soap, right? Because more than half the people who actually do rinse their hands in the washroom don’t bother using soap.
Congratulations if you know this, and thanks for your help on the front lines of infection control.
Now Roberto Berardi would like to tell you something you may not know. Drying your hands is not only the last step in this exercise, it is critically important way to be sure deadly pathogens do not leave the washroom when you do.
He will also tell you to step away from those high-tech jet-speed hand dryers, which he calls bluntly, ‘a disaster for hand hygiene’.
‘The first principle is that paper towels absorb pathogens, dryers spread pathogens,’ he said. ‘This is not a matter of opinion. Once your hands are wet, the water has to go somewhere. Either it goes into a tissue that absorbs it, or it is partly dried by a jet of air that necessarily blows away micro droplets that need to go somewhere. They go off your hands and into the air!’
Berardi is the Chairman for a group with the curious name European Tissue Symposium (ETS) that studies how people wash up after using the toilet. If you have seen people in white lab coats standing around the washrooms taking notes, that was the team from the University of Westminster who carried out a study on hand washing and drying behavior in public washrooms.
‘It is not simple to measure adherence to guidelines on hand hygiene,’ Berardi told European Hospital. ‘There is direct observation, of course, which remains the gold standard. We can conduct surveys. We can also measure how much soap has been consumed or the amount of paper towels used. Each of them has some merit, but there is also a lot of interpretation.’
Recently he introduced a more scientific approach for ETS by shifting its focus from people to the pathogens they rinse off in the sink. At the ISSA/INTERCLEAN Trade Fair for Cleaning Professionals in Amsterdam this Spring two leading microbiologists specialised in healthcare associated infection delivered their findings from a pair of studies commissioned by ETS.
Mark Wilcox MD, Professor of Medical Microbiology at the Uni-versity of Leeds & Leeds Teaching Hospitals, and Keith Redway from the Department of Biomedical Sciences at the University of Westminster, revealed the number of bacteria that remain on people’s hands after washing is markedly higher and that high-speed jet dryers contaminate the washrooms where they are installed.
Both studies have been submitted to peer-reviewed journals. As a result, Berardi said ETS is not able to yet share detailed findings from the studies. He did release some of the top level data in an announcement.
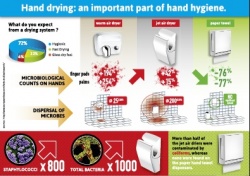
• Drying hands with conventional warm air dryers, the total number of bacteria actually was found to increase on average on the finger pads by 194% and on the palms by 254%.
• With jet-air dryers bacteria count increased on average on the finger pads by 42% and on the palms by 15%.
• Drying hands with a paper towel, the total number of bacteria was reduced on average on the finger pads by up to 76% and on the palms by up to 77%.
Blasting air at speeds of up to 500 kilometers per hour, jet air dryers blew micro droplets carrying micro-organisms up to two meters away. The model used to simulate viruses showed transmission from the hands up to three meters away.
Conventional warm air hand dryers spread airborne micro-organisms up to 25 centimeters from the dryer while paper towels showed no significant spread of micro- organisms, according to ETS.
Prof. Redway studied what he called vertical height dispersal patterns for hot air dryers where Zone One was at the level of an adult’s head.
‘We found that most of the contamination occurred in Zones Three and Four, which is where a child might be standing if it were waiting for its mother or father to dry their hands,’ he said.
ETS is continuing to support research in an effort to clear up what Berardi calls misconceptions about hand hygiene. As an example he cites a survey that showed men in England believe hot air is the most hygienic method because only clean air touches their hands after washing.
Hand washing is integral to breaking the cycle of transmission of harmful pathogens in healthcare from hospitals to nursing facilities to patient care at home, he said.
‘People say that they don’t have time to wash up before seeing patients, but the demands on their time will only increase if there is a cross contamination among patients,’ he said. ‘This excuse is far from acceptable. We need greater awareness, a fuller understanding of not adhering to these standards.’
Education is not a strong enough word for what Berardi would like healthcare administrators to do.
‘We need continuous internal marketing, posters everywhere inside the hospital,’ he said. ‘There is a good awareness among people working directly with patients, yet other people inside the hospital may need more convincing of the importance of this issue and that guidelines have been established.’
‘After that we need to monitor adherence, feedback on everything that is measured. What is not measured is not done,’ he added.
So watch for the people in the white coats, coming soon to a washroom near you.
28.07.2014





