Aneurysm - Coil, surgery or clip?
A young singer leans against the mixing desk in a recording studio in a laid-back manner. She listens to songs just recorded for her new album, moving her lips to the sound. Suddenly she stops, reaches for her head and seconds later collapses, unconscious. On hospital admittance physicians discover that a previously undetected aneurysm in her brain has ruptured.
The syndrome, which affects around 0.01% of the population annually, is rare. Once a rupture has occurred neurosurgical or endovascular treatment is available. But which procedure is the right one? Professor Andreas Raabe, Director and Head of the Inselspital in Bern, Switzerland – in which about 120 aneurysms are treated annually -- explains how aneurysms are diagnosed, their types and treatment approaches.
"On the one hand there are risk groups such as patients with autosomal dominant, inherited polycystic kidney disease, or those in whose families there have been at least two close relatives who have suffered cerebral bleeds or had aneurysms diagnosed. Meanwhile, aneurysms are often detected purely by chance in many more patients with untypical symptoms, such as headache or dizziness, are examined via MRI. A non-ruptured aneurysm is detected in around 2% of people with this procedure. Because about 50% of patients die, or are left with severe disabilities after the rupture of an aneurysm, treatment should commence before a rupture can occur. However, not all aneurysms require treatment. Small aneurysms of the anterior circulation rarely rupture if they are smaller than 6mm in size; from 7mm onwards the risk of bleeding is higher.
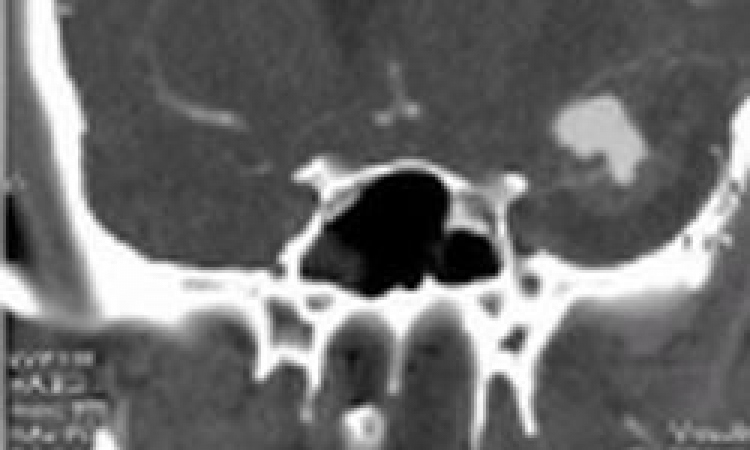
There are many types of aneurysms; mostly they show up as globular, lobed, fusiform or as protrusions – an aneurysm can basically have any shape. With an incidence of 2% they are most common in the head, but aneurysms are also common on the abdominal aorta. The only atypical aneurysms are necrotic or infectious aneurysms, which can develop in the vascular walls because of infection through bacteria or fungi.
There is no exact standard for when endovascular treatment or neurosurgery are indicated. The choice of procedure depends on how wide the neck of the aneurysm is and whether other vessels branch off the protrusion. The neuroradiologist and neurosurgeon then jointly decide how to manage treatment.
Coils
Randomised studies show that it is better to treat small aneurysms with a slim neck with coiling, as long as there’s no danger of the coil damaging the vessels. If, during coiling, it turns out that the coil does not hold, then surgery is indicated. On average, around 40% of patients undergo neurosurgery and 60% are treated endovascularly.
Clips
When coiling is not possible and the neck of the aneurysm is too wide, clips are used. These allow us to press the aneurysm together while leaving the vessel open. A clip is also the method of choice when vessels branch off the aneurysm and would be closed through the coil. But -- this requires opening the cranium. Despite this, however, the rate of severe complications for non-ruptured, incidental aneurysms is 2% of a total of 5% of all complications.
Apart from platinum coils there are also drug-coated ones, which promote stronger clotting in the aneurysm, as well as see-through coils, or those covered in hydrogel that can absorb water and swell. However, there are as yet no qualitative studies that substantiate improvements for any of these new devices and materials. Often, new technology replaces old technology before the results of long term studies have become available.
Aftercare
Only 3% of patients suffer a subsequent aneurysm within 10 years of subarachnoid bleeding (SAB) occurring, which is why there is no need for life-long screening. After endovascular treatment, patients are monitored once or twice because, in around every fifth patient, the coils can push together again. In half of these cases further treatment is required. However, in patients who have undergone surgery there is no need for special aftercare because the initial intervention resolves the problem once and for all."
21.11.2009