Tiny tools, big effects
imec, the European research centre for nanoelectronics, has linked with Johns Hopkins University in Baltimore, USA, to develop the next generation of highly miniaturised medical tools.
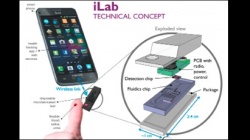
We asked Robert Bollinger, professor and director at Johns Hopkins School of Medicine, and Mark Shaver, senior director for strategic alliances at Johns Hopkins Medical, what are these ‘tools’ and where do they fit in future healthcare
Like so many medical people, Robert Bollinger is concerned about people with limited or no access to medical care. ‘For many,’ he points out, ‘it’s simply too expensive to go and see a doctor. In some regions there are no hospitals or healthcare providers, or they are too far away. And, for many, the social threshold to access the system is too high.’
Thus he welcomes all initiatives to improve access to diagnostics, particularly for chronic diseases such as diabetes. New infectious diseases, such as SARS, or bird-flu, or new drug-resistant diseases, also arrive. ‘Some cancers,’ he adds, ‘are becoming resistant to treatment. The challenge here is finding ways to identify when that happens and to select treatments best suited for each patient. Again, we’d need more high-quality diagnostic tests and individualised tests to be available anywhere.’ He is not idealistically unaware of that major issue – cost. ‘Success,’ he says, ‘will largely depend on how we can reduce cost. Our iLab-project promises to answer those challenges.’
Availabe for everyone
‘With iLab,’ explains Mark Shaver, ‘we want to integrate diagnostic tests on a chip – tests for which patients now go to medical facilities. iLab will allow them to do them at home. Our vision is a silicon chip with the ability to diagnose multiple diseases, integrating multiple laboratory tests, for under US$10, giving a result under 10 minutes, available and easy-to-use for anyone – anywhere in the world. We chose to start our collaboration with iLab because, as a concept, it’s most mature, and because we already have a pretty good idea how to make it.
‘Technically, we’re not going to push the edge on detection limits, or find new types of biomarkers. We’re going to miniaturise and integrate existing technology and tests, on a platform that can be mass-produced with standard chip-fabrication processes. We have selected a number of infectious diseases for which we want to develop better diagnostics, among them HIV infection. We’ve chosen these because they will push us to the limit of what’s possible with iLab. It will involve, for example, detecting and counting viruses, identifying proteins, quantifying metabolites, and identifying and separating types of cells.’
Changing HIV care
‘Just look at the current state of care for HIV and see what could be achieved with iLab,’ Robert Bollinger suggests. When someone is diagnosed with HIV, their eligibility to take medication and which suits them is assessed. When taking medication, another set of tests are run to see how the patient is responding to treatment, and whether there are side effects. ‘In much of the developed world, HIV patients have access to a wide range of diagnostic tests. Typically, we do a viral load test (counting virus numbers in a blood sample), a count of CD4 cells (specific type of immune cell), and the kidney and liver functions are measured.’
However, these tests, are not available for the majority of HIV patients worldwide. Without tests, he points out, it is difficult to monitor and optimise HIV treatment.
‘We envisage building a test kit with the form factor that may resemble a USB stick, to put into the hands of people who are HIV-infected. With the kit they can prick their finger and draw a tiny drop of blood to be analysed by the lab inside the kit. Ideally, this test kit would diagnose the viral load, CD4, liver function, kidney function all simultaneously. Then they can plug it into a smartphone and uplink the test results to their care provider – and in this way without even coming to the clinic, they can be diagnosed and managed at home, even in resource-limited communities.
iLab could not only change the way medical research is done, but also be a ‘game-changer’ e.g. in drug discovery, Robert Bollinger adds. ‘It’s extremely expensive to develop new drugs, particularly because clinical trials involve hundreds to thousands of people who have to be tested regularly. This technology could greatly speed up and optimise how clinical trials are done.
‘iLab could also be greatly beneficial for disease surveillance,’ he suggests. ‘A big issue with transmittable diseases, such as influenza, is to identify people who actually have the disease. Then we can link them with care and isolate them from others at risk. Right now, this is done with expensive and complex systems. Imagine having that ability with a low-cost chip that you can distribute throughout communities very easily.’
The iLab partnership structure
imec and JHU bring complementary expertise to the project. ‘Together, we will develop the building blocks of iLab, the platform on which to develop the actual diagnostic products,’ explains Mark Shaver. ‘We’re also having conversations with a number of potential partners who are willing to invest in the initial research in this first three-year phase. These will be leaders in the biotech industry, for example, who will help us identify quick pathways to new diagnostics. They will also define the products based on our platform and make them available to patients. We’ve worked intensively with imec over the last year, and discovered a really shared culture. Innovation and research is a primary driver of what we both do. So, we’re very confident going into this collaboration.’
What really drives JHU are developments that can have a positive impact in healthcare worldwide. Our goal is to have a transformative impact on health. This collaboration, starting with iLab, could ultimately transform healthcare. Not just in our communities, but globally. Epidemiology, public health care, research … could all be affected by results from this collaboration.’
Healthcare evolution in the next half century
‘I’m greatly interested in the notion of the point-of-singularity,’ Robert Bollinger says. ‘In our medical context, this is the point where we know enough about prevention and health to radically improve people’s long-term quality of life and health expectations. Imagine that you could reach the biological age of 25 or 30 and maintain that quality of health for another 60-70 years.
‘How will we reach that point? We still have to learn a lot about the mechanisms of ageing, but we know it will be crucial to individualise prevention and treatment for everyone. We’ll need individual and early prevention, diagnosis, and treatment.
‘It’s going to be all about the individual, and that individual will take much better care of him- or herself. We will diagnose our own diseases and receive our treatments at home for a majority of things; going to hospital or a clinic will be a last resort. The point-of-care is going to be where we are. We are already moving in that direction with the development of a tool such as iLab.’
PROFILE:
Associate director of the Johns Hopkins Centre for Global Health (Baltimore, USA), Robert Bollinger (right) is also a professor of infectious diseases in the department of medicine of the Johns Hopkins School of Medicine, and has a joint appointment in the department of international health of the Bloomberg School of Public Health.
The professor has more than 27 years’ experience in international public health, clinical research and education in a broad range of global health priorities, including HIV/AIDS, malaria, tuberculosis, leprosy and emerging infections.
As senior director of business development and strategic alliances, Mark Shaver (left) leads the unit within Johns Hopkins Medicine charged with the exploration, expansion, development, and management of collaboration with corporate and strategic partners. In this role, he works in partnership with a wide range of the Johns Hopkins faculty and senior leadership across the Johns Hopkins medical enterprise.
07.04.2014





