The vascular bypass revolution
Coronary or peripheral bypasses are the most frequently performed vascular operations. Although one million patients per year and around the world, undergo this intervention, its failure rate reaches 50%, because of poor vessel healing, leading to vessel graft occlusion. To improve the outcome of bypasses, researchers from the University of Geneva (UNIGE) work together with medical doctors from the Lausanne University Hospital (CHUV). They developed a gel containing microparticles –‘GeM’, enabling the controlled release of a drug inhibiting cellular over-proliferation. Administered locally, directly on the bypass graft during surgery, this preventive treatment will reduce the risk of obstruction reoccurrence.
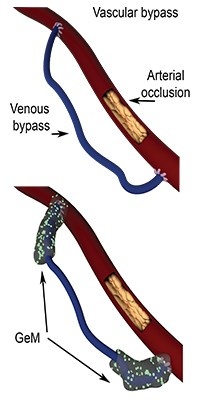
The vascular bypass allows a blocked artery to be bypassed by implanting a vessel removed from the patient, and this is done in order to create a deviation in circulation. However, in 50% of cases, excessive vascular cell proliferation, called hyperplasia, occurs around the suturing site of the transplanted vessel. Hyperplasia then leads to a decrease in blood flow within five years following the operation, requiring a new surgery. Today, doctors prescribe atorvastatin (ATV) orally against hyperplasia. However, this route of administration is not adapted to this pathology.
This is why Doctor François Saucy’s team from CHUV joined forces with Florence Delie and Olivier Jordan, researchers at the Department of Pharmaceutical Sciences at UNIGE Faculty of Science. The goal: to find a way for local administration of ATV, that will remain available over a long time period, in order to overcome the disadvantages of high dosage taken orally. ‘We immediately thought of a gel mixed with ATV, being directly applied on the vessel during surgery. Being viscous, it remains in place and enables local release, explains Florence Delie. ‘But, we had an important challenge– doctors recommended the presence of the drug over a period of four weeks to avoid hyperplasia development, while the gel is only effective for three days’. Researchers from UNIGE have consequently added polymer microparticles containing ATV to the original formulation. These microparticles carry the encapsulated drug and gradually dissolve into the gel, therefore releasing ATV over one month.
The right dose in the right place
‘It is about a controlled release system: the right dose at the right place, with the correct release profile, emphasises Olivier Jordan. ‘We discovered that this formulation only works using the combination of, on one side, quickly released ATV mixed into the gel and on the other side, the microparticles, which act over the long term. There lies our innovation’, adds Ioanna Mylonaki, researcher at UNIGE. ‘Its use on patients is contemplated in five to ten years. Its efficacy would revolutionize the success rate of vascular bypasses.’
Source: University of Geneva
01.07.2016





