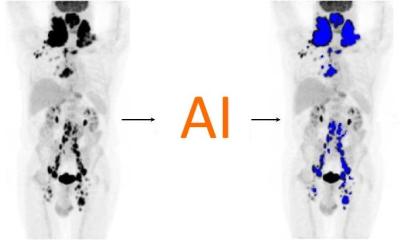
Interview • Nuclear imaging
SPECT-CT versus PET-CT: The 'little sister'?
Interview with Dr Torsten Kuwert, Director and Professor of Clinical Nuclear Medicine, Clinic of Nuclear Medicine, Friedrich-Alexander University Hospital Erlangen, Germany.

When it was suggested, during our interview with Dr Torsten Kuwert, Director and Professor of Clinical Nuclear Medicine, Clinic of Nuclear Medicine, at Friedrich-Alexander University Hospital, Erlangen, that SPECT-CT is the little sister of PET-CT, and that he might have preferred to install the ‘big brother’, Dr Kuwert pointed out the greater cost of PET, explaining: ‘The isotopes are more expensive than substances generally used for SPECT - at least in Europe. For example, the substance injected for a PET scan of the glucose metabolism costs from 300 to 500 euros. The substance used for bone scintigraphy is between 10 and 30 euros. Correspondingly, SPECT is a workhorse for nuclear medicine departments. For example, in Erlangen we perform 10 times more SPECT than PET examinations. At the university hospital we have a stand-alone PET and we want a PET-CT. But it is difficult to raise the funds. However, I’m sure we’ll have such a camera in the near future, because we our clinic will soon have a new building and the budget includes equipment.
For basic research, PET is the more flexible tool, because innovative tracers are more easily synthesised for PET than for SPECT. In addition, the spatial resolution of PET is better than that of SPECT - far better. This is due to the physical nature of nuclear decay of positrons. Scatter radiation can be calculated better and is less compared with SPECT. This is what happens: During the annihilation of the positron, two gamma rays are emitted that move at a 180º degree angle from each other, whilst with SPECT only one gamma ray is emitted. Consequently, in SPECT the scatter radiation is more difficult to reduce than in PET. This is just one difference. In general, one can say that the spatial resolution of SPECT is not as good as that of PET. But it is also true that PET requires more expensive substances than SPECT. That means, in the end, SPECT is, as I said, the workhorse. Maybe in ten years time that won’t be the case, but today there are far less PET than SPECT scans.'
Hybrid systems combine CT with SPECT or PET. The cameras’ CT component also differs, particularly in the number of CT detectors. How many slices should such a hybrid system have?
‘I think every user would answer that question individually, in terms of the particular needs of his or her department. A general answer cannot be given. In cardiology, for example, you need a 16 or 64 slice CT for coronary imaging; in oncology the lowest standard would be a two-slice, but probably a six-slice would be better. If you use the CT component just for attenuation correction and rough localisation of SPECT-positive lesions, a one-slice could be sufficient.’
By what criteria do you decide whether a patient should undergo a SPECT- or PET-CT scan?
‘There is no general answer, because, to a great extent, this depends on the indication. We can perform a SPECT following any nuclear medicine exam, but there are special PET indications in oncology. For example, with PET you can perform lymph node staging of a bronchogenic carcinoma, which you can’t do with SPECT. That’s a classic example, since SPECT cannot process the radioactively marked glucose solution used as a radiopharmaceutical. Nuclear medicine means that a radiopharmacological substance is injected, and there are many of these substances for a wide range of purposes. The choice depends on the individual patient and his condition and the situation, and then which imaging procedure is selected.’
Is that an empirically validated selection?
‘Yes. A further reason is that radiopharmaceuticals are specifically developed just like any other pharmaceutical. This means that the initial discussion is about which metabolic process would be interesting to image, then radiopharmaceuticals are developed that can “infiltrate” that process. Currently, for research into psychiatric illnesses, in co-operation with Professor Gmeiner from the Institute of Pharmaceutical Chemistry at our university, we are trying to visualise certain sub-types of the dopamine receptor, and we are trying to develop substances that dock on to these receptors - the so-called radioligands.
The problem with psychiatric diseases is that, in most cases, there are no animal models. There is no such thing as a schizophrenic mouse. Therefore, we need to examine the brain of a schizophrenic patient. To do this we need, above all, imaging technologies that can visualise metabolic processes, and that means nuclear medical imaging: PET or SPECT. The diagnostic value of such scans depends on the radiopharmaceuticals used. The brain has many interesting metabolic aspects: receptors, transmitter metabolism, etc. The researchers’ task is to provide substances with which the metabolic steps in question can be visualised in a living patient. Hyperactivity disorder is a good example. We know that it is probably caused by a lack of dopamine and that it can be treated - at least sometimes - with dopaminergic medication. But we don’t know what exactly happens. We don’t know much about the receptor systems that are relevant in this context. Their function in the human brain as a whole is only marginally known, because it is difficult to research. It has to be done on the living person, it can’t be done only with a brain slice.
What is the Working Group on Correlative Imaging?
‘In general, correlating means that one tries to establish a relationship between different data. So, correlative imaging means that one tries to establish a relationship between different imaging data. In the case of the brain, PET and SPECT are usually combined with MRI but, on the other hand, this is usually done retrospectively - retrospective fusion - because presently hybrid cameras combining those modalities are not available.
Why can’t the SPECT problem be solved with fusion?
That’s a very good question, and one we’ve been thinking about a lot. We initiated a research project with Professor Hornegger at the Technical Faculty, which aims at developing intelligent fusion algorithms. The problem is that we have to deal with the different positions of a patient in the different camera systems. This is done by non-rigid transformations, but calculating them correctly is a major problem. For us, the Working Group on Correlative Imaging does not mean that we have a piece of equipment that we install and that that’s, but that we look at all existing research approaches. This is comparative imaging with the objective to match - to generate an image of a patient that has three-dimensional features that are matched with each other. Let’s say you have a certain region of the brain and you ask: What exactly does it look like? How does metabolic process X function in that region? Or metabolic process Y? and How can we match X and Y 100%? That is the objective of correlative imaging. There are many different approaches. Unlike ten years ago, we can now at least use the data of all modalities on one computer - thanks to DICOM. We can superimpose these data - but then we realise that unfortunately the patient was positioned differently in scan A and scan B. Then we have a problem. It still yields interesting results, no doubt, but that’s not the exact match that we had envisaged. The matching procedure could be done with a hybrid camera or with a good non-linear transformation, but that doesn’t exist yet.’
What is SPECT’s molecular task?
‘SPECT is a form of molecular imaging. Today, molecular imaging is a buzzword. As soon as you visualise a metabolic process in a living human being, that’s molecular imaging. The term has recently been a little overused in marketing efforts for the PET-CT. Molecular imaging is the old principle of nuclear medicine, initially developed by a Jewish-Hungarian scientist called von Hevesy, who received the Nobel Prize in 1943 for his discovery that metabolic processes can be studied with radioactive substances. So that’s not particularly new.’
In what situations would PET-MRI would be useful?
‘There are issues for which MRI and not CT is used clinically, let’s say the differentiation of liver tumours. If you combined that with a PET scan, differentiation of liver tumours might be easier. For such things, PET-MRI would indeed be useful. Basically, MRI is intensively used for brain examinations. However, I should add that, due to the fact that the brain does not change much between the different scans, a rigid retrospective image fusion will do. The brain undergoes no major changes in position and form, no matter how the patient is positioned. But if there were hybrids it would be more interesting to look at regions outside the brain. It seems that there are still hardware problems because PET detectors and magnetic fields don’t like each other. But I am sure it will happen one day. And let’s hope we are the ones to have that machine!'
07.08.2006