Urostation
Prostate diagnostics: increased accuracy
In mid-2015 the second generation of the ultrasound system H60 and the Urostation Touch was launched. At the Urology Department of the Hospital Fürth in Fürth, Germany the H60 and Urostation Touch are already being successfully used with 4 to 5 patients a week for prostate diagnostics.
Patients who present with increased PSA levels undergo an mpMRI scan of the prostate since MRI achieves higher sensitivity in the detection of cancer lesions than other imaging modalities. “I have been a radiologist for 35 years and have been watching the development of multiparametric Magnetic Resonance Imaging – mpMRI – of the prostate from the very beginning,” says Professor Josef Gmeinwieser, Medical Director of the Radiology Department at Klinikum Fürth. “Today, mpMRI yields much more reliable results than prostate ultrasound. While sonography has a 50 percent sensitivity in the detection of suspicious areas, diffusion and perfusion imaging multimodality MRI has been achieving a sensitivity of 80 to 90 percent.”
Hand in hand: radiology and urology
“However, if a mpMRI finding indicates that a biopsy is necessary, it is rather difficult to perform it using MRI. It is much easier with ultrasound if you know where to take the tissue samples,” explains Professor Gmeinwieser. Therefore these two modalities have been merged.
After an mpMRI scan was made, both the radiologist and the urologist assess the suspicious findings and decide on the areas to be marked for biopsy. Then the mpMRI scans of the prostate including the markings are loaded in the Urostation.
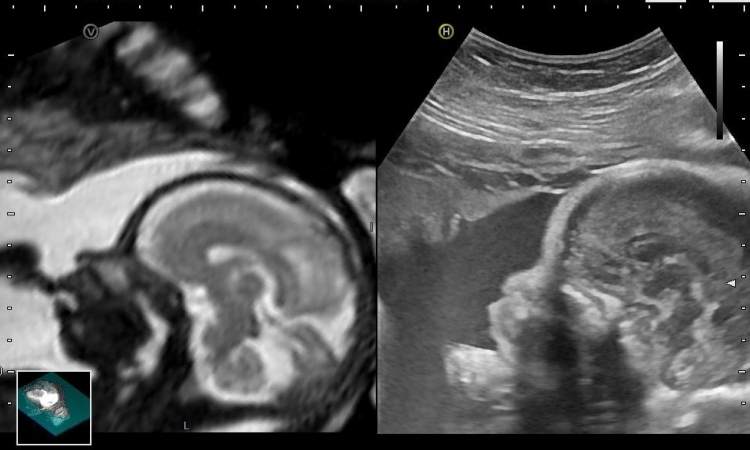
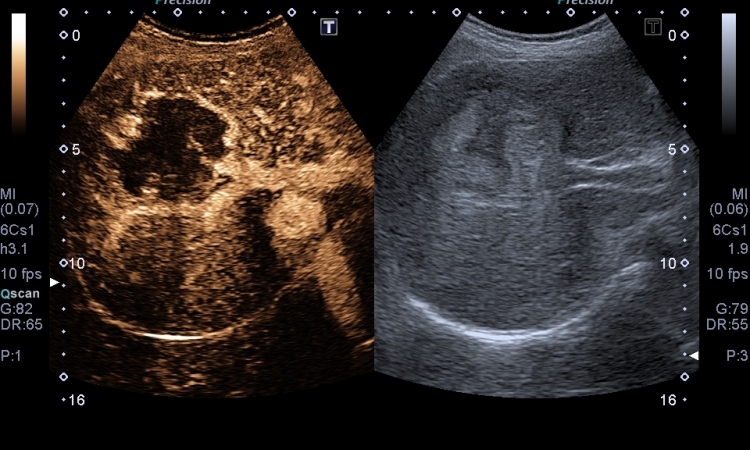
Using a 3D endocavity probe a 3D ultrasound image of the prostate is generated and sent to the Urostation where it is fused with the MR images. The 3D ultrasound image is used to guide the biopsy while the mpMRI data show the location of the tumours. As soon as the images are matched and fused, the physician performs a virtual biopsy using the ultrasound image to control whether he would really “hit” the suspicious areas. Once the target is confirmed the actual biopsy is carried out. While the biopsy needle is still in the prostate the 3D images are transmitted to the Urostation where they are displayed to check if the target was hit. “With the Urostation we achieve high accuracy in the detection of tumours, especially aggressive and dangerous ones,” says Professor Blana, who is Head of the Department of Urology at Klinikum Fürth.
Elastic fusion improve detection rate
The so-called Elastic Fusion technology matches the mpMR and 3D ultrasound images since the prostate shape changes despite its relative stiffness, firstly because the patient is in different positions during the ultrasound and the mpMRI scan and secondly because the 3D probe exerts pressure on the prostate.
No more superfluous biopsies
A biopsy is a stressful procedure for any patient. Therefore any technology that helps to avoid multiple or unnecessary biopsies is highly appreciated by patients and physicians alike. Professor Blana: “The Urostation allows us to avoid repeat tissue sampling. During an untargeted biopsy you often fail to hit the tumour – and then, after a few weeks, you have to repeat the procedure if you continue to suspect a malignant tumour. With the Urostation usually one biopsy is sufficient as we hit the suspicious areas right the first time.
“In addition to the targeted tissue samples we sample 12 further locations systematically in compliance with current German guidelines.”
Professor Blana moreover uses the Urostation as a tool for focal lesion therapy which requires extremely precise diagnostics. “Our experience with the Urostation is excellent,” Professor Blana underlines, “The biopsy results are highly satisfactory. More and more patients ask for biopsy with image fusion.”
To get to know our products, visit us at Medica Hall 9/C63 or visit our Website: www.samsung.de/hme
16.11.2015