Polytrauma whole-body CT in the shock room
Optimised scan protocols reduce radiation exposure
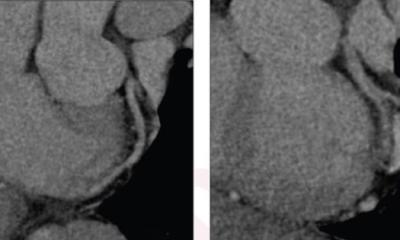
Whole-body CT scans during shock room treatment of polytrauma patients are on the increase since their advantages are obvious: they are a fast and comprehensive examination that allows immediate therapy-relevant decisions.
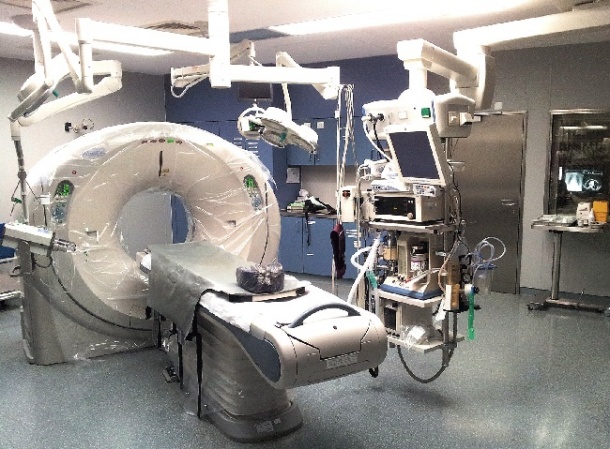
For his doctoral thesis Stefan Reske evaluated the whole-body CT scans of trauma patients performed at the Clinic for Imaging Diagnostics and Interventional Radiology at Bergmannstrost hospital in Halle, Germany. ‘We decided on an interdisciplinary level that trauma patients who fulfil certain criteria upon admission undergo a whole-body CT scan in order to exclude severe internal trauma which may cause decompensation later on. Since not every patient admitted to the emergency department suffers from severe – meaning life-threatening – injuries we as trauma radiologists have a particular responsibility to make every effort to reduce radiation dose as far as possible during diagnostic imaging. Time is of the essence in trauma care as about every three minutes mortality increases by one percent,’ explains Stefan Reske, assistant physician at Bergmannstrost hospital in Halle which features a renowned trauma centre where radiologists, trauma surgeons, anaesthetists and neuro-surgeons work hand in hand.
An extremely tight whole-body CT protocol had existed for several years when, in 2010, Stefan Reske was asked to review all patients to whom the protocol had been applied and to determine radiation exposure during the scan. ‘The result was a rather high effective dose of on average 45 mSv for a whole-body scan from head to toe. The completely automated protocol comprised basically two mandatory scans: firstly a native head and cervical vertebrae scan followed by a contrast-enhanced scan from the base of the scull to the pubic bone in order to detect injuries of the vessels and the internal organs. When upon initial exam of a patient the trauma surgeon suspected injuries to the legs an optional third scan covering the legs and feet followed,’ Stefan Reske explains.
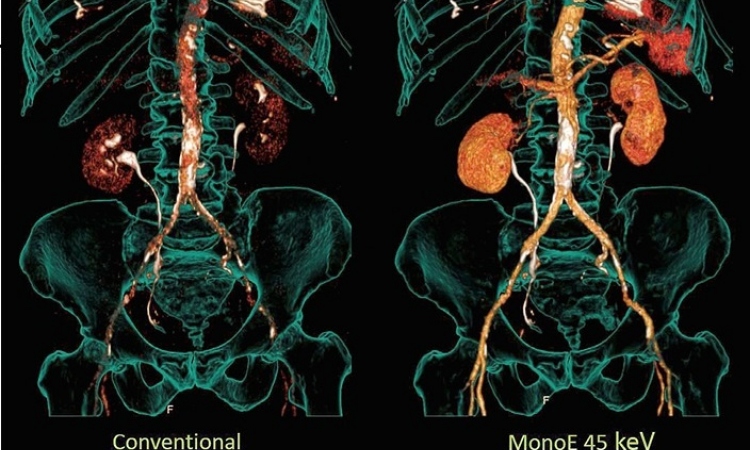
‘Today, modern CT scanners feature an iterative reconstruction function which allows a significant reduction in dose – a technological option that unfortunately had not been available to us. Therefore in the course of my project we adapted the original protocol and are now using two differently weighted ones,’ the young physician points out. In addition to a time-optimised protocol, which apart from some minor technical changes is identical to the original one, there is now also a dose-optimised protocol. The crucial modification of the dose-optimised version is the fact that the arms are positioned behind the head. The interdisciplinary shock room team decides which protocol will be used. If the patient is stable and there are no indications of a trauma on the upper arms and shoulders the dose-reduced examination is performed. With instable and severely injured patients the time-optimised protocol will be used.
‘Compared to the old protocols the new time-optimised one can reduce effective dose to 31 mSv while the dose-optimised version may decrease dose by approximately 40 percent to 26 mSv. In the meantime further potential to reduce dose by optimising the protocols has been identified. Realising this reduction is a major task in my current project,’ Stefan Reske reports.
PROFILE:
Stefan Ulrich Reske MD first trained as a paramedic before his medical studies at Friedrich Alexander University Erlangen-Nürnberg. After his 2007 graduation he joined the Delitzsch district hospital as an assistant physician, but in 2010 opted to take up radiology, since serving at the Imaging Diagnostics and Interventional Radiology Clinic at Bergmannstrost hospital in Halle (Saale). A Dresden native, Dr Reske is emergency physician and participates in the emergency service in the German Federal State of Saxony-Anhalt.
18.11.2013