Prevention
Next step in preventing diabetes
A team of scientists at Helmholtz Zentrum München, in collaboration with Technische Universität München and the German Center for Diabetes Research (DZD), have shown in a preclinical model that specifically modified insulin mimetopes may lead to an immune tolerance. The results, published in ‘Nature Communications’, may be a step to improved prevention of type 1 diabetes.
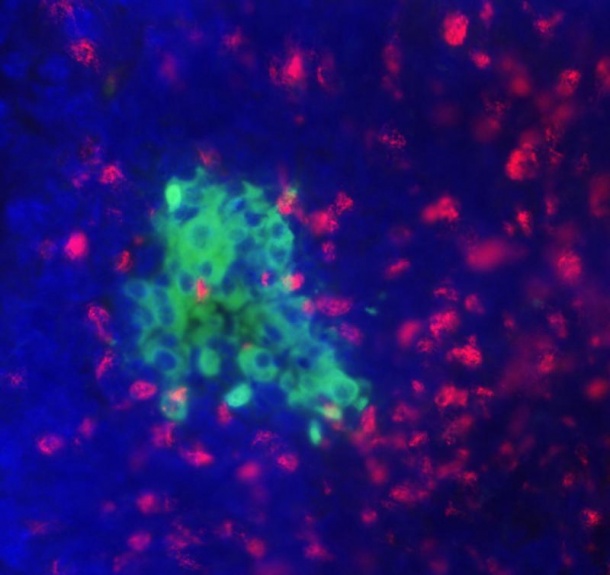
Type 1 diabetes affects 30,000 individuals throughout Germany and is the most common metabolic disease in children and adolescents. To halt the ever-increasing incidence, the young investigator group “Immunological Tolerance in Type 1 Diabetes” at the Institute of Diabetes Research directed by Prof. Dr. Anette-Gabriele Ziegler is exploring new strategies to prevent the onset of the disease.
In the current study, the scientists investigated the effect of specifically modified insulin mimetopes on the immune system. “In particular, we wanted to find out whether we can induce the protective regulatory T cells to produce a tolerance of the body against insulin, if we bring them into contact with our novel peptides,” said Dr. Carolin Daniel, who leads a young investigator group and directs the study.
Optimized mimetopes curb the immune system
The study is based on findings Daniel made several years ago at Dana Farber Cancer Institute and Harvard Medical School in Boston. There she showed that insulin mimetopes she optimized were significantly more efficient in inducing a tolerance through regulatory T cells towards insulin than their natural counterparts (epitopes). In young mice, the induction of insulin mimetopes at low doses completely halted the development of type 1 diabetes.
The next step was achieved in the study that has just been published: In a so-called humanized mouse model, whose immune system is very similar to that of humans, the scientists were able to confirm the results – an important indication for the effectiveness of the optimized human insulin mimetopes.
“In fact, we were able to show that the new vaccine efficiently stimulates the regulatory T cells, which then can impede the attack of the immune system on the insulin-producing cells,” said lead author Isabelle Serr, who was involved in the study within the framework of her dissertation.
In the long term Daniel and her group want to further develop the method for preventive treatment of children at high risk for type 1 diabetes. “An important step will be to test the new therapy clinically – that is our vision“, said Daniel with regard to the future.
Source: German Research Center for Environmental Health, Helmholtz Zentrum München
17.03.2016



