Protein DART
New shock-and-kill strategy against HIV
A unique molecule developed at Duke Medicine, the University of North Carolina at Chapel Hill and MacroGenics, Inc., is able to bind HIV-infected cells to the immune system’s killer T cells. It could become a key part of a shock-and-kill strategy being developed in the hope of one day clearing HIV infection.
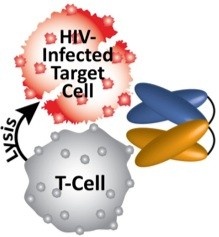
The molecule is a type of bi-specific antibody known as a Dual-Affinity Re-Targeting protein, or DART. It was engineered by MacroGenics, using HIV-targeting antibodies discovered at Duke. Employed increasingly in cancer research, bi-specific molecules have shown effectiveness in helping the immune system recognize and clear tumor cells. In this case, pre-clinical models demonstrate that DART creates a fatal union between HIV-infected cells and killer T cells.
When Julia Sung, M.D., lead author and clinical assistant professor in medicine at UNC, used DART molecules in combination with additional agents that wake up latent reservoirs of the virus hiding in the body, the approach showed early promise as a way to clear HIV infection.
“This is an exciting approach that has the potential to clear a pool of cells that are so hard to get rid of -- virus that lies silent and hidden in the host,” said Barton Haynes, M.D., director of the Duke Human Vaccine Institute and a senior author of a study describing the molecule in the Journal of Clinical Investigation. “These drugs would be combined with other drugs that activate expression of HIV in the cells,” Haynes said. “As soon as they are awakened, the DART molecules hit them and causes the killer T cells to destroy the virus.”
Haynes and colleagues at UNC, the University of Alabama-Birmingham, and MacroGenics report that the DART strategy was highly effective in clearing HIV in laboratory experiments.
To try to model what might happen if patients were treated with DART molecules to clear persistent infection, lymphocytes were taken from patients on HIV therapy. These cells were then re-infected with different HIV virus subtypes, and with viruses previously recovered from the same patient’s latent viral reservoir. When the patient cells expressed these various viral strains, DART molecules facilitated CD8 “killer” T cell clearance of the infected cells.
In another pre-clinical modeling experiment in the laboratory, exposing HIV-positive patients’ cells to HIV latency reversing agents –- drugs which are under development to force dormant HIV out of hiding -- the DART molecules showed potential to be effective immunotherapeutic weapons to clear these latent HIV reservoirs.
“A similar approach is being tested to cure some forms of cancer," said David Margolis, M.D., co-corresponding author and professor of medicine, microbiology and immunology at UNC. “This idea is being repurposed for curing HIV with our partners at Duke and MacroGenics. This paper shows that DART molecules can recognize different strains of HIV, bind to cells, and clear and kill the virus in many different scenarios.”
"While the research into DART molecules is still in early stages, it is very exciting to see how these molecules can turn otherwise ineffective T cells into potent killing machines against HIV latently infected cells,” Margolis said.
The researchers said the DART approach is especially promising because the molecule recruits from a large pool of T cells, regardless of specificity, creating a broad attack that is not dependent on targeting any single HIV strain.
“Because we are targeting a region of the virus envelope that appears in all mutations of the virus, we think it will make it much easier to be broadly utilized -- at least from our laboratory data,” said co-corresponding author Guido Ferrari, M.D., associate professor of surgery and molecular genetics and microbiology at Duke. “These DART molecules will facilitate the recognition. We are eager to see how this translates to human studies.”
“This is a great opportunity for MacroGenics to expand our DART platform for therapeutics applications beyond oncology and autoimmune disorders and into infectious diseases,” said Scott Koenig, M.D., Ph.D., president and CEO of MacroGenics. “We are encouraged by our proof-of-concept studies that show HIV DART molecules to be potent immunotherapeutic agents with the potential to reduce HIV reservoirs in patients.”
Source: Duke Medicine
13.10.2015