Big data
Multiparametric imaging
The vast amounts of data accumulating in breast diagnostics require new methods to extract clinical information in a practical way. When dealing with large amounts of data that is too big or too complex to be analysed with traditional data processing applications, the talk today is of ‘Big Data’. The data volume accumulating in breast diagnostics has become increasingly complex over recent years: multiparametric MRI including diffusion imaging and MRI spectography, positron emission tomography (PET) and tomosynthesis (3-D mammography) along with the various ultrasound procedures, generate such vast amounts of data that its evaluation is turning into a Herculean task.
Report: Karoline Laarmann

‘It’s becoming ever more difficult to view and sort all the data and finally to make a diagnosis for the individual radiologist,’ according to Associate Professor Dr Pascal Baltzer, at the Clinic for Radiology and Nuclear Medicine, Medical University of Vienna, who lectured on Big Data in Breast Diagnostics at the 96th German Radiology Congress.
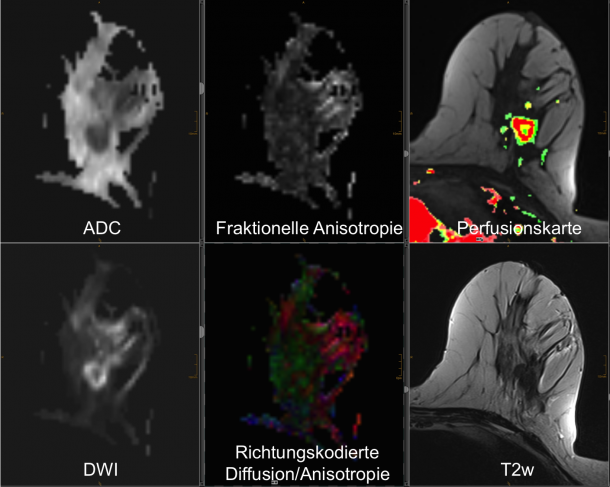
Multiparametric MRI for instance – Baltzer’s specialist area of research – delivers a multitude of results. Based on blood pressure measurements alone, through signal changes caused by contrast media injected, different distribution volumes and perfusion parameters can be calculated with pharmacokinetic models (such as perfusion rate of tissue, extracellular distribution volume). ‘If you then add the other technologies, all of which show different functional aspects of a tumour – be it biochemistry, microanatomy or perfusion – you obtain a very comprehensive but also very complex image of the tumour,’ Baltzer explains. However, this also raises a number of questions: What does the parameter measured mean in an individual case? How should individual parameters be combined? Could a parameter that proved meaningful in a study also extract usable information under clinical conditions and with other devices?
‘There is significant demand for empirical data acquisition that not only validates the above mentioned technologies multicentrically, but also examines them as to which data is required and which isn’t,’ he points out, turning to a dilemma that arises. On the one hand we’d like to visualise the tumour in any possible biochemical and molecular way but, on the other, the images obtained also need to be converted into a practical concept. Radiologists in practices outside academic settings obviously need to be able to use the data,’ he emphasises. Therefore he believes that the order of the day is data mining. ‘This means disposing of the data ‘waste’ within the ‘mine’ of data whilst extracting the diamonds.’ By using methods of machine learning and multivariate statistical models, the flood of data is reduced and patterns are recognised. This obviously requires a correspondingly large database – containing many hundred or even thousands of multiparametric sets of data. ‘This is only available in very few facilities,’ Baltzer regrets. The Medical University of Vienna, where she carries out her research, is one of those facilities. The point of this undertaking is solid: Whilst the approach with other organs, such as the prostate, can be described as ‘active surveillance’ in breast cancer diagnostics there is a heated debate involving the terms ‘over diagnosis’ followed by ‘over therapy’. Baltzer emphasises: ‘We know from studies that a not insignificant number of tumours, and particularly precancerous conditions, grow so slowly – or do not develop at all – so it would be better to leave them be or to just actively monitor them.’
Multiparametric imaging makes it potentially possible to differentiate between aggressive and less aggressive tumours without a needle biopsy. The detailed information about the type of tumour is, of course, not only of great importance for diagnosis but also for treatment planning and monitoring. ‘As with all these procedures, a lot of ground work is needed,’ warns Baltzer. ‘You have to identify these procedures, test them, check their reliability and then validate them.’
08.07.2015