Article • High tissue contrast, spatial detail, complete tissue characterisation
MRI shows cardiac diagnostic value
Cardiovascular magnetic resonance (CMR) imaging has become faster, simpler and more widely available in recent years because it has evolved to deliver effective assessment and diagnosis of a range of heart conditions with expanding guideline indications.
Report: Mark Nicholls
‘MRI is the reference test for anatomical imaging of the heart, for quantifying chamber sizes and function,’ explains Professor Sven Plein, British Heart Foundation Professor of Cardiovascular Imaging and Professor of Cardiology at the University of Leeds, United Kingdom.
Over recent years, with his Leeds team he has conducted extensive research on MRI – significantly in the cardiac arena – and in particular on the cardiovascular effects of diabetes using MRI and in developing quantitative MRI methods. ‘Cardiovascular MRI,’ he points out, ‘is a non-invasive and safe imaging test with the main benefit of providing high tissue contrast, spatial detail and comprehensive tissue characterisation. Recent developments in parametric mapping and automated perfusion analysis are continuing to move MRI from visual analysis to quantitative description of pathology.’
MRI vs CT
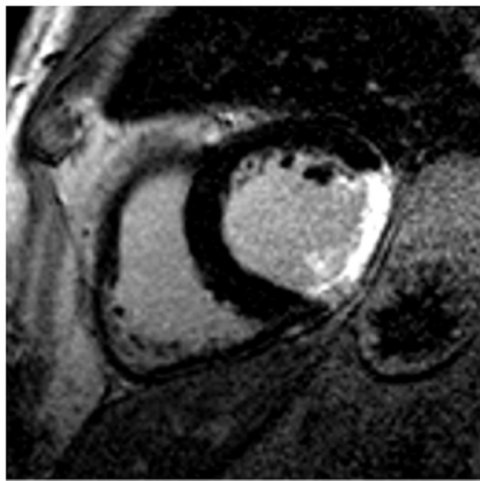
Whilst MRI offers a number of benefits over CT, he emphasises that the two modalities should be regarded as complementary rather than competing. ‘CT is the method of choice for imaging the coronary arteries, while MRI is most powerful for functional imaging of the myocardium,’ Plein adds. ‘Of course, CT exposes patients to a small dose of X-ray radiation, while MRI doesn’t, and MRI contrast agents are generally safer than CT contrast agents. In practice, however, both tests are increasingly used to replace invasive methods for different indications.
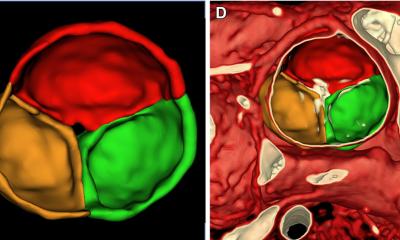
‘In congenital heart disease, MRI is the “go-to” test to figure out complicated anatomy, and plan and assess the effectiveness of complex surgery. In children in particular, we need to avoid repeated exposure to X-rays, so would always aim to use MRI as the first line test. Increasingly, cardiologists are using MRI not just to take anatomical pictures, but also to assess tissue composition and tissue characteristics of heart muscle.’
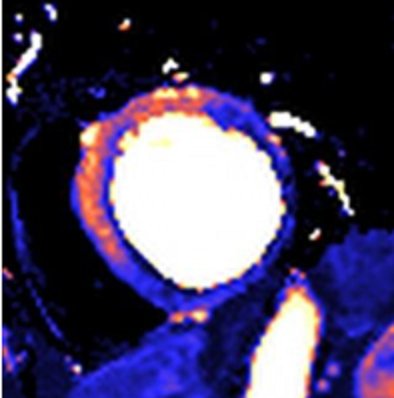
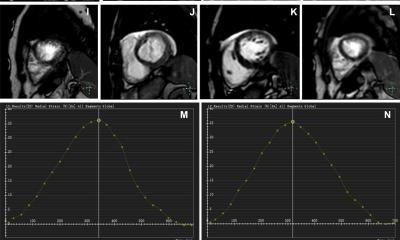
Plein outlines the benefits of parametric mapping as an important area of development and one that delivers a quantitative colour map output that encodes a range of tissue properties such as T1, T2 and T2* times. ‘We can map areas and create normal values for these parameters. Increasingly, these quantitative methods are used to describe the composition of the cardiac muscle and its content in terms of fibrotic tissue, fat and water content as well as abnormal loading with, for example, iron in thalassaemia patients.’
After several years of development, myocardial blood flow can now also be measured quantitatively with automated in line methods via MRI. That development – which is important in ischaemia detection – will shift the approach from the subjective observation of an experienced cardiologist assessing dynamic images of heart muscle enhanced by contrast, to a numeric quantification of blood flow from a colour-coded map.
Stress perfusion imaging
In daily practice MRI is becoming an indispensable test for patients with congenital heart disease, cardiomyopathy and heart failure, ischaemic heart disease and many more
Sven Plein
‘Techniques are now coming onto the market where software generates a colour map that shows the amount of blood flow through the heart muscle at rest and during stress – stress perfusion imaging – and whether there are any abnormalities,’ Plein continues. ‘These will soon be commercially available, offering another exciting addition to the growing quantitative MRI methodology.’
Magnetic resonance imaging continues to help improve understanding of heart disease. ‘MRI provides detailed information about cardiac and vascular function, presence of scar or fibrosis in the heart muscle, fat content, blood flow and much more,’ he points out. ‘In daily practice MRI is becoming an indispensable test for patients with congenital heart disease, cardiomyopathy and heart failure, ischaemic heart disease and many more. In research, MRI methods are in development to image the microstructure of the heart, visualise complex 4-dimensional flow, and heart metabolism. This helps us better understand the mechanism of heart failure and other conditions.’
Profile:
Sven Plein is British Heart Foundation Professor of Cardiovascular Imaging and Professor of Cardiology at the University of Leeds, where he leads a large interdisciplinary research group for development and clinical implementation of imaging methods. Key areas of research are on the cardiovascular effects of diabetes using MRI and in quantitative myocardial blood flow measurements. The professor also heads the Department of Biomedical Imaging Science, in the Leeds Institute of Cardiovascular and Metabolic Medicine, University of Leeds and is Consultant Cardiologist & Clinical Lead for Cardiovascular Magnetic Resonance at Leeds Teaching Hospitals NHS Trust.
02.09.2019