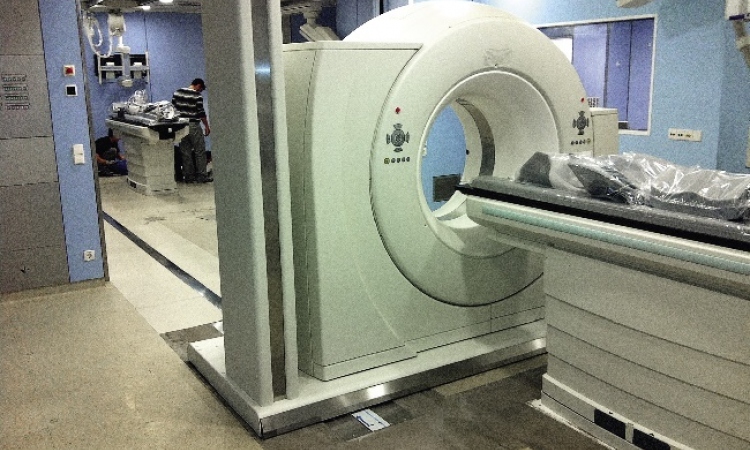
CT: Overuse in emergencies, but top value for trauma cases
By Professor Moshe Graif MD
Over the last three decades CT has become a premier diagnostic tool for the evaluation of the acute patient. Over the past ten years in Israel, we have seen an overwhelming increase in the volume of CT examinations in the emergency department (ED).
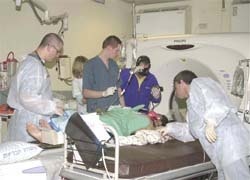
Data from the USA and Germany appear to yield similar results. A comparison of the number of CT studies performed per 1000 ED visits showed a five-fold increase over one decade! Particularly dramatic was the increased use of CT studies during the night shift. A particular increase in body CT studies in the ED (Renal Colic, appendicitis, acute abdomen, bowel obstruction) over neurological CT was also noted.
Surprisingly, the massive CT utilisation patterns had no significant impact on the consumption of other imaging services (such as X-rays). Expectations that examinations — such as acute abdominal series (AAS) which have limited clinical value in patients in whom CT or ultrasound is considered — will decrease, were not met. The five views skull radiographs so far appear to be the only example of an ‘extinct species’.
The ‘Golden Hour’ (Dg & treatment within 60 minutes) rule, which nowadays dictates the management of the trauma patient, favours CT, as a ‘one stop shop’, over the combination of several modalities. It also appears that clinicians may still feel more comfortable with CT images than with ultrasound. Emergency doctors prefer to use CT as the gold standard for imaging abdominal trauma and to reserve FAST (focused abdominal sonography for trauma) for unstable patients.
These trends boost healthcare costs. They also affect patients due to increased radiation exposure and more incidental findings that lead to further investigation (not always justified). They create queues of patients waiting for a CT examination (prolonging the average investigation time for each patient, particularly the clinically more justified cases).
Regarding radiation exposure, the 2007 report of the National Council on Radiation Protection & Measurements (NCRP) revealed that the collective annual population medical radiation dose increased between 1980 and 2006 by 7.5-fold. The number of CT scans performed in the USA has grown from 18.3 million in 1993 to 62 million scans in 2006.
As for the cost, a recent study has shown, for example, that cervical spine CT use shot up by more than 400% and the number of admissions rose by only 13%, while severity of injury and illness changed little. A cost analysis yielded an expenditure of
US$ 8,509 for each positive study.
It has also impacted on radiology teams. Over half of Emergency CT studies are performed during the shift hours, involving smaller and less experienced teams. Those teams are also subjected to the effect of prolonged, continuous working hours and accumulated fatigue. While the technical time per CT examination has decreased (Spiral CT exam time is shorter by 2.3-10 factor) which induces increased throughput, the radiologist reading time is prolonged because there are more images to read (69% more images per MDCT study on average), more reconstructions to perform, and change in procedure mix (more complicated studies such as CTA, abdominal studies, CT guided interventions).
A particular aspect of Emergency CT is related to its role in mass casualties events (MCE).
It appears that hospitals situated near to such events play a major role in trauma patient care. More than 50% of patients are evacuated to the nearest hospital within 5-20 minutes. This creates an immediately overwhelming overload on all hospital medical resources, including CT; it is therefore mandatory to have a hospital preparedness plan to be able to deal effectively with the situation. Generally two phases can be observed. The Initial Phase – when casualties are flowing in and chaos is at maximum. In this phase, the main objective is to identify the critically injured patients, who need to be treated first. From a radiological point of view it usually requires the use of abdominal ultrasound and chest X-rays. The definitive phase occurs when casualties are no longer arriving. At this point, the main objective is to provide optimal care, which involves more skeletal X-Rays, CT work up and angiographies.
The clinical nature of the cases that involve blast and/or shrapnel injuries requires special CT protocols. This includes whole body scans to identify foreign bodies missed on a radiography and triple contrast regime (via naso-gastric tube, intravenous injection and rectal contrast administration). There is also a routine use of CT angiography and 3-D reconstructions in every case of a penetrating object and/or suspicion of vascular involvement.
In those situations, CT now offers a quick mode to evaluate the extent of injury, shrapnel localisation and the detection of unsuspected injuries. The rapidity of the modality makes patient co-operation less necessary. The availability of PACS, and heavy duty workstations, enables simultaneous evaluation of a complex injury by several specialist teams.
The velocity of execution and accuracy make CT an ideal tool for emergency use, and is replacing traditional radiological studies. Utilisation is likely to increase. The development of techniques designed to reduce radiation are constantly under intensive consideration.
Careful use of the guidelines may help to reduce the unnecessary studies. In the future, more radiologists and technicians will be needed, and residency programme planning measures should be taken at national level to ensure the proper future availability of a professional workforce.
* I would like to thank Dr. Ahuva Engel, Dr. Dorith Shaham, Dr. Ofer Benyaminov, Dr. Jacob Sosna, Dr. Osnat Luxenburg, Dr. Arie Blachar, Dr. Eli Konen, Dr. Arnon Makori, Prof. Pinhas Halpern, Ms. Sharona Vaknin and Mabel Zelikovitz Msc for their help in providing scientific data for this report.
03.03.2008