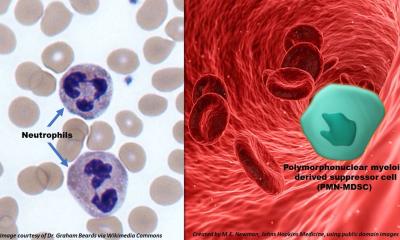
Image source: Shutterstock/Christoph Burgstedt
News • SARS-CoV-2 neutralising antibodies
Covid-19 immunity may last from days to decades
Scientists from Singapore found that antibodies against SARS-CoV-2 wane at different rates, lasting for mere days in some individuals, while remaining present in others for decades.
The study, published in The Lancet Microbe, shows that the severity of the infection could be a deciding factor in having longer-lasting antibodies. Individuals with low levels of neutralising antibodies may still be protected from Covid-19 if they have a robust T-cell immunity.
The team followed 164 Covid-19 patients in Singapore for six to nine months, analysing their blood for neutralising antibodies against SARS-CoV-2, T cells and immune system signalling molecules. They then used this data to establish a machine learning algorithm to predict the trajectories of peoples’ neutralising antibodies over time. "The key message from this study is that the longevity of functional neutralising antibodies against SARS-CoV-2 can vary greatly and it is important to monitor this at an individual level. This work may have implications for immunity longevity after vaccination, which will be part of our follow-up studies,” said Professor Wang Linfa, from Duke-NUS’ Emerging Infectious Diseases (EID) Programme, a corresponding author of the study.
This study reminds us that we all react differently to infection and that various people mount different protective immune responses. Understanding the basis of these differences will help build better vaccines
Laurent Renia
The team was able to categorise people into five groups depending on how long their antibodies lasted. The first group, who never developed detectable neutralising antibodies also called the ‘negative’ group, comprised 11.6% of the patients in the study. The ‘rapid waning’ group (26.8%) had varying early levels of antibodies that waned quickly. The ‘slow waning’ group (29%) tested mostly positive for antibodies at six months. The ‘persistent’ group (31.7%) showed little change in their antibody levels up to 180 days and, finally, the ‘delayed response’ group (1.8%) showed a marked rise in neutralising antibodies during late convalescence.
While this study focused on determining the levels of neutralising antibodies, which are part of the body’s comprehensive immune defence system, the other important aspect of an effective immune defence is T-cell immunity. The study found that the patients tested, including those from the ‘negative group’, displayed sustained T-cell immunity six months after initial infection. This shows that individuals may still be protected if they have a robust T-cell immunity when the neutralising antibody level is low. “Our study examines neutralising antibodies which are important in protection from Covid-19. We found that antibodies against SARS-CoV-2 wane in different people at different rates. This emphasises the importance of public health and social measures in ongoing pandemic outbreak response. However, the presence of T-cell immunity provides hope of longer-term protection which will require more studies and time for epidemiological and clinical evidence to confirm,” said Associate Professor David Lye, Director, Infectious Disease Research and Training Office, National Centre for Infectious Diseases (NCID), who is also a corresponding author of the study. “This study reminds us that we all react differently to infection and that various people mount different protective immune responses. Understanding the basis of these differences will help build better vaccines,” added Professor Laurent Renia, Executive Director, Agency for Science, Technology and Research (A*STAR) Infectious Diseases Labs.
The findings are important as policy makers design vaccination programmes and pandemic exit strategies. The rate of antibody waning suggests re-infection may occur in subsequent waves of infection. Also, if immunity provided via vaccinations wanes like naturally-produced antibodies, then annual vaccine administration could be necessary to prevent future outbreaks of Covid-19. Further research will be needed to clarify this as vaccine programmes are rolled out.
Source: Duke-NUS; National University of Singapore
25.03.2021