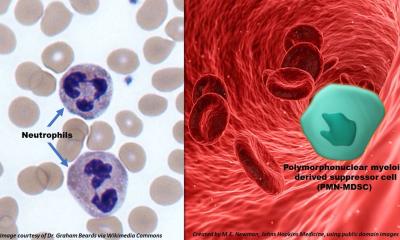
© University Hospital of Tübingen / Beate Armbruster
News • T-cell activator shows promise
"CoVac-1": Coronavirus protection for immunocompromised patients
Good news for patients with acquired or congenital immunodeficiency: The results of a clinical phase II study at the University Hospital Tübingen led by Prof. Dr. Juliane Walz and Prof. Dr. Helmut Salih show an effective activation of T cells against the coronavirus.
After positive results in healthy volunteers in the previous phase I, the T-cell activator "CoVac-1" was now able to reproduce these effects in cancer patients for the first time. The results have been published in the journal Nature Communications.
Even after the end of the Covid-19 pandemic, viral infections such as Sars-CoV-2 pose a serious threat to patients with weakened immune systems. This group includes, in particular, cancer patients who, due to their disease itself or due to tumor therapy, are unable to mount an adequate immune response following natural infection or with conventional vaccines. These patients often do not develop antibodies against the viral disease. For this reason, the Tübingen team has developed a vaccine with the aim of better protecting immunocompromised patients against infectious diseases. This vaccine specifically activates T cells, which are another important component of our immune system and play a decisive role in the defense against infectious diseases.
Recommended article
Article • Covid-19
Coronavirus update
Years after the first outbreak and spread of coronavirus Sars-CoV-2, its impact can still be felt in everyday life. Keep up-to-date with the latest research news, political developments, and background information on Covid-19.
For this purpose, the novel T cell activator CoVac-1 was used, which in itself is being developed for cancer immunotherapy, one of the main research focuses of the Tübingen immunologists. As early as 2022, CoVac-1 was successfully tested on healthy volunteers and showed good tolerability with very good immune stimulation, i.e. very strong activation of T cells.
This local reaction is expected and desired for our T-cell activator. It is an expression of the formation of a depot at the vaccination site, which prevents rapid degradation of the T-cell response and thus enables a long-lasting immune response
Jonas Heitmann
A total of 54 patients were vaccinated once as part of the study. Most of the study participants suffered from blood cancers and showed a significantly weakened immune system due to the disease itself or the tumor therapy. There were little to no side effects. Only a few mild complaints such as headaches and fatigue were reported. Local induration developed at the vaccination site in all subjects. "This local reaction is expected and desired for our T-cell activator. It is an expression of the formation of a depot at the vaccination site, which prevents rapid degradation of the T-cell response and thus enables a long-lasting immune response," explains Dr. Jonas Heitmann, one of the study's first authors.
The long-lasting effect is particularly noteworthy. Thus, even four weeks after vaccination, the broad and strong T-cell immune response was detected. In initial follow-up studies, these immune responses remained unchanged in strength. Even in severely immunocompromised patients, the T-cell responses activated by CoVac-1 are significantly more pronounced than in recovered individuals after natural infection and also more potent than the T-cell immunity generated by licensed mRNA or vector vaccines.
CoVac-1 is produced in the drug peptide laboratory and the so-called GMP unit of the University Hospital and Medical Faculty in Tübingen. Here, too, the long-standing experience and expertise in the production of vaccines for cancer patients is being drawn upon. The clinical evaluation of the T-cell activator is carried out in the KKE Translational Immunology, a unique facility in Germany in the Department of Internal Medicine of the University Hospital. It was established to test innovative immunotherapy concepts as quickly as possible in initial clinical trials so that patients can benefit from new research findings as quickly as possible. The study was also conducted under the direction of the University Hospital Tübingen at hospitals in Frankfurt am Main and the Charité in Berlin.
Based on these encouraging results, the team is already working on the development of vaccines using T-cell activators against numerous other infectious diseases that pose a threat to immunocompromised tumor patients. In addition, this study also provides an important contribution to the development of therapeutic vaccines for affected individuals, which are currently already being investigated in patients with various solid tumors and blood cancers.
Source: University Hospital of Tübingen
27.08.2023