Celebrating the 60th birthday of a fabulous lifesaver
This May it will be exactly 60 years since the first extracorporeal circulation device to temporarily replace heart/ lung function was successfully used in a clinical setting.


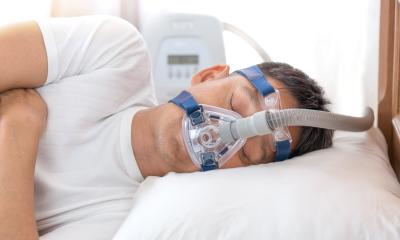
High time for a big cheer, says EH correspondent Holger Zorn, who recalls the anguish and excitement, high hopes and shattered dreams in medical history. Block aorta! Maximum vent!’ The tension in the operating theatre (OT) is on high voltage as surgeons, nurses and perfusionists approach the first critical moment in cardiac surgery. Terse commands fly about: ‘Cardioplegia on!’ The aorta is clamped, blood is drained from the heart and a solution is pumped into the coronary arteries. The heartbeat slows, flutters, and then lies entirely silent. It is also still. However, that flat green line on the monitor does not mean death, but hope. Bypasses are inserted, holes are closed and valves are repaired. The contraption that makes all this surgical wizardry possible is exactly 60 years old. On 6 May 1953, John Heysham Gibbon, a surgeon at Pennsylvania University in Philadelphia, repaired an atrial septum defect in 18-year-old Cecelia Bavolek using a heart-lung machine (HLM).
John Gibbons had taken almost a quarter of a century to develop the method and construct an apparatus to siphon venous blood from the large veins, remove the dioxide, enrich the blood with oxygen and return it, clean and filtered, to the human aorta. Up to six litres per minute, unfailingly, for hours. The saga began on 3 October 1930, when Dr Gibbon, then a young assistant physician, was asked by his boss to stay on night watch with a patient who suffered from severe pulmonary embolism. Without doubt, she was dying. It was impossible to simply cut open her heart and remove the thrombi. That night the young doctor had the idea to replace the heart, a muscle pump, with a mechanical pump for just a few hours, as long as the surgery would take.
Cat and fish
John Gibbon’s boss wouldn’t have any of it. But his assistant, Mary Hopkinson, was to become one of the young surgeon’s most important partners in research – and in real life. After their March 1931wedding, they began their experiments, first using cats lured off the street with fish. They occluded the pulmonary arteries and pumped the blood through a mechanical lung. On 10 May 1935 the first cat survived. It had been without its own heart function and kept alive by extracorporeal circulation. Mary and John prance about the lab, elated. World War II interrupted their work but, after the war, IBM supported their research and deployed engineers to construct three heart-lung machines. Model II brought success.
A biker’s life saved
1972, barely twenty years after Dr Gibbon’s pioneering feat, a 24-yearold man rode his motorbike through Santa Barbara, California, fell and suffered a closed thorax trauma. The lungs were compressed, aorta damaged. Four days after surgery his lungs failed. By that time Donald Hill and team, at the Pacific Medical Centre in Los Angeles, had significantly improved the heart-lung machine, particularly replacing the rotating discs of the gas exchanger by a membrane lung.
They transported the device to Santa Barbara, connected it to the patient and supported his circulation for three days. With an extracorporeal blood supply of 3.0 to 3.6 litres per minute, oxygen tension in the blood increased from 38 to 75 mmHg, oxygen in the tidal air was reduced from 100 to 60 percent and peak airway pressure was reduced from 60 to 35 cm H2O. Respiratory distress was relieved; the patient recovered.
Three years later, in 1975, a baby girl was born at the Orange County Medical Centre. Something was wrong. Her small lungs would not work properly. Despite the ventilation system, oxygen tension fell to 12 mm Hg. Robert Bartlett, pulmonary surgeon and co-developer of the membrane lung, brought a machine that had never before been used for a baby. The child’s mother tried to understand what she was hearing, signed the patient consent form with an X and disappeared, never to be seen again. Being an illegal immigrant from Mexico, staying in the hospital would have meant arrest and deportation. After three days of blood oxygenation the baby’s lungs were strong enough to work without mechanical support. The nurses had named the girl Esperanza - hope...
HLM going mobile
In 1997, again almost 25 years later, a 55-year-old surgeon collapsed in his own practice in Germany. The emergency physician arrived on the scene within minutes, but too late. He was the surgeon’s friend. If he had had an HLM, Georg Matheis was convinced he could have saved the surgeon. As a result, he founded a company to develop the world’s first really mobile heart-lung machine. Dr Matheis wanted the device to weigh only ten percent of a normal HLM – less than 20 kg. Whilst he quit the company he founded to pursue other goals, in 2007 the Lifebridge B2T proved its worth at the German Heart Institute in Berlin. In 2008 the machine received Europe-wide approval; FDA clearance followed in 2010.
Today, millions of people worldwide live on thanks to a heart-lung machine. However, it could not save its inventor. In 1973, during a tennis match, John Heysham Gibbon died of a heart attack. Recently Lifebridge Medizintechnik AG also needed reanimation and was acquired by ZOLL Medical.
13.05.2013