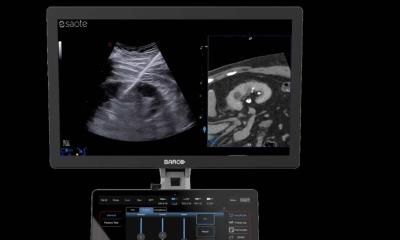
Ultrasound in trauma and orthopaedics
At October’s annual congress of trauma and orthopaedic surgeons in Berlin, the session Ultrasound beyond trauma and orthopaedic surgery – What can we learn from neighbouring disciplines? exposed the unexploited potential of ultrasound for trauma and orthopaedic surgery, EH correspondent Bettina Döbereiner reports.

Although ultrasound is clearly anchored in the German Regulations on Further Education, which governs specialist training for trauma and orthopaedic surgeons, ultimately it very much depends on personal engagement and commitment as to what extent the procedure is learned and utilised in daily clinical life, said Dr Gerhard Achatz, registrar at Ulm Military Hospital. This particularly applies in the case of ultrasound applications at the interface with other medical disciplines, he believes. Thus the session also focused on paediatric ultrasound, ultrasound of the heart, thorax, blood vessels and peripheral nervous systems, along with the more common abdominal ultrasound. Initially knowledge of all those applications did not appear essential for all trauma and orthopaedic surgeons equally; however, looking beyond one’s own medical field is certainly beneficial to pick up useful ultrasound examination procedures, which is definitely the case in pericardial effusion or pneumothorax diagnosis, he explained. The ability to make a differential diagnosis can be of great benefit for initial orientation and fast treatment – particularly when more specialised colleagues cannot be reached, whether in a pre-clinical setting, the resuscitation room, emergency unit or intensive care ward.
Other easy to learn procedures include the differentiation between chronic and acute right ventricular pressure, the assessment of the cardiac filling volume and the evaluation of global left-ventricular function. Diagnosis of valvular heart defects and stenoses, Dr Kühlmuss said, can be taught and learned comparatively quickly; intensive training for a week is sufficient. ‘The big advantage with cardiac ultrasound is that you can continue using the same transducer used for abdominal ultrasound,’ he explained. Although the transducer used for echocardiography is a little slimmer, this is not a problem. ‘You just need to visualise the image without the left and right border.’
Single-handed pneumothorax diagnosis?
Dr Thomas Berlet, interdisciplinary intensive care specialist at Bern University Hospital explained that standard ultrasound scanners are sufficient for thoracic ultrasound. Next to the differentiation of bruised ribs and fractures and a diagnosis of pleural effusion, he specifically emphasised the ability to consider or exclude a pneumothorax. It is now very easy to exclude a pneumothorax by documenting certain artefacts caused by the normally positioned, synchronically moving lungs on the ultrasound image. These three types of artefacts are called lung sliding, comet-tails, which are also named B-lines, as well as the lung pulse which is visible on the lung surface even when the lungs do not move. The application and interpretation itself is easily learned: 12 examinations under professional guidance suffice to safely exclude or diagnose a pneumothorax, he explained.
The 2012 recommendations from the International Consensus Conference on Lung Ultrasound classify ultrasound as a so-called grade A recommendation for differential diagnosis as well as for the exclusion of pneumothorax in emergencies and for point-of-care, as he pointed out. However, he added that, to date, information has been contradictory; a 2012 meta-analysis evaluating all clinical studies published on pneumothorax diagnosis with ultrasound concluded that sensitivity during scanning is higher than the specificity compared to conventional X-ray diagnostics.
With thoracic ultrasound he also resolves other issues in his daily work, including whether pneumonia or pulmonary oedema is present. He is convinced that, apart from pneumothorax diagnosis, these applications will soon be more common, particularly in the pre-clinical field, due to the increasing spread of the smallest portable ultrasound scanners.
Following graduation from Ulm University, internist and cardiologist Bernd Kühlmuss MD became a medical officer in the German army. At this time he trained in emergency medicine. From 1996 he worked in a number of cardiac centres across Germany and in the internal medicine departments in Ulm Military Hospital and Ulm University Hospital, focusing on cardiology, angiology and pneumonology. In 2002 he became Assistant Clinical Director at the Ulm Military Hospital and in 2003 became head of Cardiology.
Gerhard Achatz MD, registrar at the Department of General Surgery as well as Orthopaedics and Trauma Surgery at Ulm Military Hospital, Germany, studied medicine at Regensburg University, became a registrar in its surgery department for two years and then as an army doctor and flight surgeon. In 2011, at the same hospital, he became a research associate in the Department for Trauma and Orthopaedic Surgery, Reconstructive and Septic Surgery and Sports Traumatology, particularly focusing on ultrasound with contrast media. Since 2013 he has led the Ultrasound Working Group at the German Society for Trauma Surgery.
Thomas Berlet MD, consultant in critical care medicine in the of intensive care department at Bern University Hospital, Switzerland, studied in Heidelberg and Cologne, and gained his postgraduate medical education in anaesthesia and intensive care in the anaesthesia and critical care department at Cologne University Hospital and in anaesthetics departments at the Bristol and Oxford Schools of Anaesthesia, UK. When portable ultrasonic devices arrived, he specialised in point-of-care ultrasound for diagnostic and interventional purposes. He has been as consultant in critical care medicine at London’s Royal Free Hospital and as Clinical Director of Anaesthesia Department at a university-affiliated hospital in Herdecke, Germany.
12.11.2013