The National Health Service Taskforce
A new organisation is formed to help end serious surgical errors
A taskforce has been set up in England after it emerged that more than 750 patients had suffered as a result of serious preventable mistakes in hospitals over the past four years.
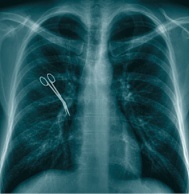
The incidents included cases of surgeons operating on the wrong part of a patient’s body or leaving surgical instruments inside after a procedure. Such incidents are categorised by the Department of Health as ‘never events’ because they are deemed to be so serious that ‘they should never happen’.
Now, the Royal College of Surgeons has stepped in to help take steps to ensure that such errors – which should never happen if national safety recommendations are followed by medical staff - are cut significantly. The President of the Royal College of Surgeons, Professor Norman Williams, said: ‘The recent survey of “never events” in hospitals in England shows unacceptable levels of preventable mistakes are still happening. However rare these incidents are, we believe never should mean never and avoiding such errors should be the priority of every surgeon.
‘Together with NHS England, we have formed a taskforce, which will look at ways to put an end to such errors. The group will be working with patients, individuals and organisations to learn from what has happened in the past to understand how to prevent them in the future.’
The number of incidents came to light following a Freedom of Information request to National Health Service (NHS) Trusts with findings that there were 322 cases of foreign objects left inside patients during operations; 214 cases of surgery on the wrong body part; 73 cases of tubes, used for feeding patients or for medication, being inserted into patients’ lungs; and 58 cases of wrong implants or prostheses being fitted.
In one example, a mother-of-four was left with seven-inch forceps inside her for three months following keyhole surgery to remove her gallbladder. The mistake was only discovered after the patient was sent for an MRI scan, which added to her agony when the magnetic field from the scan caused the metal inside her body to move.
As part of the on-going drive to reduce such incidents, the World Health Organisation’s patient safety checklist has also been adapted for use in hospitals in England and Wales.
Professor Williams added: ‘The World Health Organisation Surgical Safety Checklist is instrumental in reducing “never events” and we have supported its development and putting it into practice. Surgery is about team-working and the checklist allows all members of the theatre team to raise any concerns and is central to preventing avoidable mistakes.’
Dr Mike Durkin, director of patient safety for NHS England, has ordered a review and said that NHS England – which sees some 4.6 million hospital admissions for surgery annually - has already started to collate data to help educate staff on better practice and avoid such incidents. He said that the number of ‘never events’ occurring in English hospitals was too many, adding: ‘We need to understand what it is, in some systems and in some hospitals, that that team working hasn’t produced an effective outcome and a mistake, and a ‘never event’ has occurred. ‘This is not just the concern of one operating theatre in one hospital. It should be the concern of the leadership of that organisation, of the trust, so that they lead that trust and support both the staff in the operating theatres to work effectively, but also recognise their responsibility for leading safety across the whole of the trust.’
Profile:
Consultant colorectal surgeon Professor Norman Williams is President of the Royal College of Surgeons (since July 2011). He is Professor of Surgery and Director of Innovation at the Academic Surgical Unit of Barts and The London, Queen Mary’s School of Medicine and Dentistry and National Centre for Bowel Research and Surgical Innovation. His main clinical interests are sphincter preservation and reconstructive surgery, and his scientific interests are concentrated on GI motility and anorectal physiology.
26.08.2013