Article • Research
Testosterone clue to male heart deaths
As men appear to have higher risk of cardiovascular disease (CVD) than women of a similar age – with vascular calcification a strong predictor of mortality and morbidity from CVD – a team from the University of Edinburgh hopes that exploration of a link between gender and calcification could help unlock the pathway to new therapies. The researchers have been looking at whether sex hormones could be the common ground, focusing on testosterone as the primary and most well-recognised androgen in men.
Report: Mark Nicholls
They hypothesised that exogenous androgen treatment induces vascular calcification and could explain this gender disparity and that testosterone may be key in explaining why men have a greater risk of heart attack.
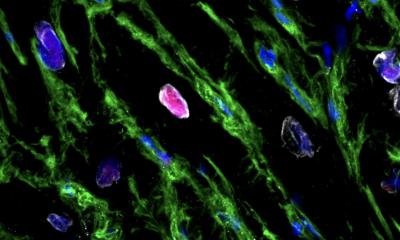
Initially the study focused on the effects of testosterone on blood vessel tissue from mice and found that the hormone triggers cells from the blood vessels to produce calcification, which causes blood vessels to harden and thicken. In addition, when the mouse cells were modified, by removing the testosterone receptor so that they could no longer respond to testosterone, the cells produced far fewer calcium deposits.
The researchers also looked at blood vessel and valve tissue from humans with heart disease who had undergone surgery for their condition. They found that cells from these tissues contained bonelike deposits and also carried the testosterone receptor on their surface, suggesting that testosterone may trigger calcification in humans.
The work was co-ordinated by Dr Vicky MacRae, Group Leader and Reader at The Roslin Institute and Royal (Dick) School of Veterinary Studies at the University of Edinburgh. ‘Vascular calcification, a pathological process which involves the deposition of hydroxyapatite crystals in cardiovascular tissues, powerfully predicts mortality and morbidity from cardiovascular disease’ she said. ‘This study addressed the hypothesis that testosterone induces vascular calcification. Our in vitro studies found that testosterone increases the calcification of vascular smooth muscle cells (VSMCs). Furthermore, testosterone-induced calcification was reduced in VSMCs lacking the androgen receptor (AR) through which the biological actions of testosterone are predominantly mediated.’

With androgens playing a role in inducing vascular calcification through the Androgen Receptor (AR), researchers suggest that androgen signalling may represent a potential therapeutic target for clinical intervention. ‘The prevalence of vascular calcification is sexually dimorphic, showing a relative increase in men compared to women, suggesting a hormonal influence,’ Dr MacRae added. ‘Our data showing a direct effect of testosterone on accelerating vascular calcification may therefore be key to explaining why men have a greater risk of heart attacks.’
At present, there is no comprehensive pharmaceutical treatment to inhibit the development of vascular calcification. However, the Edinburgh team say this study furthers existing knowledge of the basic mechanisms underpinning this pathological process, and highlights androgen signalling as a novel potential therapeutic target for clinical intervention. Research is on going to understand the pathways behind the process and whether the results have implications for patients with heart disease. ‘Calcification is particularly difficult to treat, as the biological processes behind the disease are similar to those used by our body to make and repair bone,’ Dr MacRae explained. ‘By finding this link between testosterone and calcification we may have discovered a new way of treating this disease and also reducing heart disease.’
Funded by the British Heart Foundation (BHF) along with the Biotechnology and Biological Sciences Research Council (BBSRC), this research focused on testosterone was a collaborative study across a number of different research groups within the University of Edinburgh in Scotland.
Profile:
Vicky MacRae PhD is Group Leader and Reader at The Roslin Institute and Royal (Dick) School of Veterinary Studies at the University of Edinburgh. Her group undertakes research on bone formation and vascular calcification, examining the mechanisms of differentiation and calcification in growth plate chondrocytes, osteoblasts, vascular smooth muscle cells and valvular interstitial cell
25.08.2016