Simulation training in Europe
In many countries, simulation training is well-established as a core part of training for doctors and medical personnel.

In the UK, for example, a pilot study by the Nursing and Midwifery Council (NMC) on the benefits of simulation training concluded that the results were ‘overwhelmingly positive, and suggest strongly that simulated learning offers students opportunities to achieve outcomes that are not possible in the clinical setting’. Furthermore, the NMC now recommends that 300 hours of the 2,300 hours practice qualification component be given over to simulation training. Elsewhere, the picture is very different.
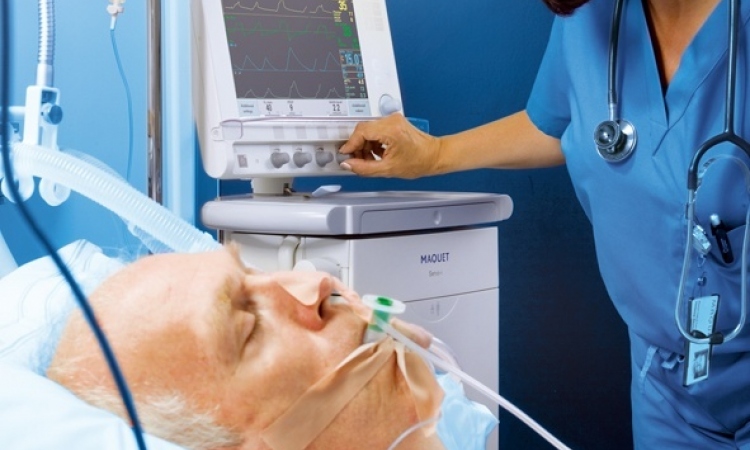
In Germany, although there is no general quality standard that stipulates patient simulation as a component of training, the simulation training centre at Erlangen Anaesthesiology Clinic is well established. Its latest acquisition is a SimMan 3G. Used for training and practice, this life-size model, is manufactured by the Norwegian firm Laerdal Medical. SimMan 3G is the newest model in its product range and this is its first use in Europe. ‘We have been successfully using Laerdal products in the training and education of our medical personnel for several years,’ explained Dr Georg Breuer, senior physician and head of the Erlangen simulation centre. ‘We chose the SimMan 3G to better prepare students and young doctors in particular for emergency situations. Thanks to its many realistic simulation characteristics, the newest model in the SimMan range is the ideal training aid.’
Laerdal has developed simulation product for many years, starting with Resusci Anne 50 years ago. Over the last 10 years the advanced patient simulators SimMan, SimBaby, SimNewB and ALS Simulator has been brought to the market. Other well known brands include the therapy products Heartstart, Q-CPR, Pocket Mask, Stifneck, and BaXstrap.
SimMan G is a fully independent patient simulator which can realistically simulate a large number of clinical scenarios, Laerdal added. ‘An integrated computer controls clinical events, attached sensors register treatment by the student and allow SimMan 3G to react accordingly. Bodily fluids, such as blood, urine and saliva, are also incorporated in the simulator and they are released in accordance with the simulated illness.’
Speaking with Gabriela Eriksen (European Hospital) about the firm’s 50-year history and recent developments, Laerdal’s CEO Tor- Morten Osmundsen said: ‘The idea was to make medical training realistic and focusing on the core competence. That was based on our entrepreneurship and curiosity, with key doctors in the US to support a new therapy on CPR. From our point of view, what has changed in the last ten years is that there is far more knowledge, research and information about the need to enhance hospitalised patients’ safety, and in the education systems to support a better quality in training and outcome to improve patient survival.’
A decade ago, he pointed out, a USA report showed that over 100,000 patients died annually due to systematic errors, communication errors and to some extent to the lack of the right competences. ‘This showed the need for a better and more efficient type of education, and at the same time a good culture for implementing competence-based and outcome-based hospital care. Of course everybody is aiming for that and wants to get that but there is research that shows there are new avenues to reach that point.
‘We believe simulation is a way of being able to practice and repeat and get feedback on difficult situations. You are able not only to train your practical skills but also your communication and leadership skills. You can learn in a team to handle critical situations and secure good leadership, resource management. So, why simulation - why not train as before? First, we think, because it is not easy to spend time with a patient. When you are being educated, or coming into a hospital system, the time available to communicate or be part of a difficult situation is rare. Patient contact and feedback is needed early in the education, but today these practical experiences come too late – when you are entering real hospital life. That is a lack of proficiency. Simulation needs to start early in an education course, to train in a real situation in a hospital/patient scenario. You can communicate with the patient, practice your skills, receive feedback, work in a team and can repeat what you did. You can prepare your team on a patient and in a critical situation and help to prepare the whole response team.’ Simulation can have several levels, using simple or advanced tools depending on the learning objective, he pointed out.
Speaking of cross-border healthcare activities in Europe, he said that comparable standards in education are needed. ‘Simulation is also used to measure competence and validate competence in the initial education phase, as well as later in a career. You used to be able to standardise an approach to the competence level you needed at a particular hospital, but today you don’t know what training doctors have gone through, or how they deal with patients. With simulation you can standardise and help to lift the competence level and get people quickly into good practice.’
Simulation, which was first adopted in the USA, has now begun to be used in the UK. ‘All European countries are doing great things now to raise their standards, but we have a fair way to go before we can talk about synergies, similar systems and standards.
Wireless technology, he added, is promising for enabling in situ simulation and mobility practices, and also to provide scenarios and patient cases in a curriculum to help bring new personnel into practice sooner. It also could be envisaged that a doctor presenting international experiences via a simulation could assess students, and much more. ‘Our vision is also to make simulation cases available on a e-learning basis so that students can practice on those cases at home with a tutor and can recognise the same scenarios when they join a team.’
01.07.2009