News • Guselkumab vs Secukinumab
Psoriasis: New data point to improved treatment
The Janssen Pharmaceutical Companies of Johnson & Johnson announced results from the ECLIPSE study demonstrating that Tremfya® (guselkumab) was superior to Cosentyx® (secukinumab)* in treating adults with moderate to severe plaque psoriasis for the primary endpoint assessed at week 48.
Data from the multicentre, randomised, double-blind head-to-head Phase 3 study demonstrated that 84.5 percent of patients treated with guselkumab achieved at least 90 percent improvement in their baseline Psoriasis Area Severity Index (PASI) score at week 48, compared with 70.0 percent of patients treated with secukinumab (p<0.001).1 These data, presented at the 3rd Inflammatory Skin Disease Summit (ISDS) in Vienna, 12–15 December, mark the first-ever results from a head-to-head study comparing an interleukin (IL)-23-targeted biologic therapy (guselkumab) with an IL-17 inhibitor (secukinumab). ECLIPSE is Janssen’s fourth Phase 3 study for guselkumab in plaque psoriasis2-4 and is part of a comprehensive clinical development programme that also includes ongoing Phase 3 studies in psoriatic arthritis and Crohn’s disease.5,6
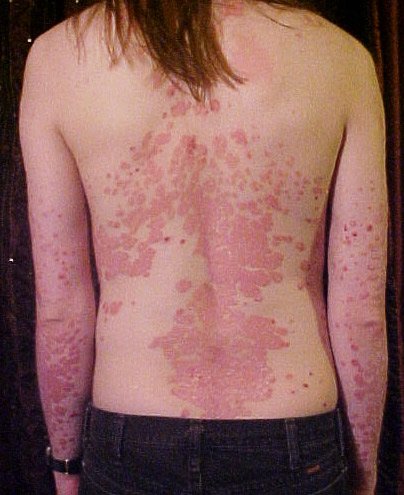
User:The Wednesday Island (of the English Wikipedia) [GFDL or CC-BY-SA-3.0], via Wikimedia Commons
“Psoriasis is a painful, debilitating and life-long condition, and those who suffer from it are in need of treatments that not only work well, but work well for a long time,” said Dr Jaime Oliver, MD, Janssen Therapeutic Area Lead, Immunology, Europe, Middle East & Africa, Cilag GmbH International. “The evidence supporting guselkumab shows that not only does this treatment offer patients high levels of skin clearance, but our current 3-year data shows a consistent maintenance of efficacy – something we hope to see continue as we gain more data.”
ECLIPSE incorporated six major secondary endpoints that used a fixed statistical sequence procedure to control for multiple comparisons and included both shorter and longer-term analyses. Guselkumab demonstrated non-inferiority to secukinumab in the first major secondary endpoint, with 84.6 percent of patients on guselkumab achieving a PASI 75 response at both weeks 12 and 48 versus 80.2 percent of those on secukinumab (p<0.001), however, it did not demonstrate superiority (p=0.062). Because superiority was not demonstrated for the first major secondary endpoint, p-values for all the subsequent major secondary endpoints were considered nominal.1
Three of the remaining major secondary endpoints evaluated efficacy at week 48, including achievement of a PASI 100 response and Investigator’s Global Assessment (IGA) scores of 0 (cleared), or 0 or 1 (cleared or minimal disease). At week 48, 58.2 percent of patients receiving guselkumab achieved a PASI 100 response, compared with 48.4 percent of patients receiving secukinumab; 62.2 percent of patients receiving guselkumab achieved an IGA score of 0 compared to 50.4 percent of patients receiving secukinumab and 85.0 percent of patients receiving guselkumab achieved an IGA score of 0 or 1 compared to 74.9 percent of patients receiving secukinumab (all comparisons with nominal p≤0.001).1
Fortunately for patients, there are many good treatment options available for plaque psoriasis today. However, to make the best recommendation for their patients from among these options, physicians need long term comparative safety and efficacy data
Newman Yeilding
The remaining major secondary endpoints assessed non-inferiority of guselkumab versus secukinumab at week 12. The percentage of patients achieving a PASI 75 response at week 12 was 89.3 percent for guselkumab and 91.6 percent for secukinumab (p<0.001 for non-inferiority); the percentage of patients achieving a PASI 90 response at week 12 was 69.1 percent for guselkumab and 76.1 percent for secukinumab (p=0.127 for non-inferiority).1 “The response-over-time curves show that maximum response rates with guselkumab are achieved after six months and are maintained over time through one year, achieving superiority at the primary endpoint of the study,” said lead study investigator Richard Langley†, M.D., FRCPC, Professor, Division of Clinical Dermatology & Cutaneous Science, Department of Medicine, Dalhousie University, Canada. “Results of the study confirm a slightly more rapid onset of response with secukinumab, but importantly in a chronic disease like psoriasis, these data provide new insights into comparative longer-term efficacy.”
The safety profiles observed for guselkumab and secukinumab in ECLIPSE were consistent with the known safety profiles seen in the respective registration trials and current prescribing information. Similar percentages of patients receiving guselkumab (77.9 percent), and secukinumab (81.6 percent) reported at least one adverse event (AE). Serious AEs were reported in 6.2 percent of patients receiving guselkumab and 7.2 percent of patients receiving secukinumab. Serious infections occurred in six patients receiving guselkumab and five patients receiving secukinumab.1
“Fortunately for patients, there are many good treatment options available for plaque psoriasis today. However, to make the best recommendation for their patients from among these options, physicians need long term comparative safety and efficacy data. We’re proud to have conducted this important trial to help guide clinical practice and continue to build on the robust database of clinical information that we’ve been able to generate on guselkumab, the first IL-23 inhibitor,” said Newman Yeilding, M.D., Head of Immunology Development, Janssen Research & Development, LLC.
*Cosentyx (secukinumab) is a trademark of Novartis AG.
†Dr Langley is a paid consultant for Janssen. He was not compensated for any media work.
References:
1. Langley, RG et al. (2018) 3rd Inflammatory Skin Disease Summit 2018, 12–15 December;Vienna, Austria: LB4.
2. Blauvelt, A et al. (2017) Efficacy and safety of guselkumab, an anti-interleukin-23 monoclonal antibody, compared with adalimumab for the continuous treatment of patients with moderate to severe psoriasis: Results from the phase III, double-blinded, placebo- and active comparator-controlled VOYAGE 1 trial. J Am Acad Dermatol. 76(3):405–17.
3. Reich, K et al. (2017) Efficacy and safety of guselkumab, an anti-interleukin-23 monoclonal antibody, compared with adalimumab for the treatment of patients with moderate to severe psoriasis with randomized withdrawal and retreatment: Results from the phase III, double-blind, placebo- and active comparator-controlled VOYAGE 2 trial. J Am Acad Dermatol. 76(3):418–31.
4. Langley, RG et al. (2018) Efficacy and safety of guselkumab in patients with psoriasis who have an inadequate response to ustekinumab: results of the randomized, double-blind, phase III NAVIGATE trial. Br J Dermatol. 178(1):114–23.
5. ClinicalTrials.gov. A Study Evaluating the Efficacy and Safety of Guselkumab Administered Subcutaneously in Participants With Active Psoriatic Arthritis. Identifier NCT03158285. Available at clinicaltrials.gov/ct2/show/NCT03158285. Last accessed December 2018.
6. ClinicalTrials.gov. A Study of the Efficacy and Safety of Guselkumab in Participants With Moderately to Severely Active Crohn's Disease (GALAXI). Identifier NCT03466411. Available at: https://clinicaltrials.gov/ct2/show/NCT03466411. Last accessed December 2018.
Source: Inflammatory Skin Disease Summit (ISDS)
13.12.2018