Increasing the range of minimally invasive tumour therapy
Surgery is no longer the automatic choice to eradicate malignant tumours.

For about a dozen years small tumours and metastases in the liver have been eliminated by heat generated at the tip of a catheter, a technique that began with liver tumours, has spread to the lung, and could be applied to breast and prostate cancers in the future.
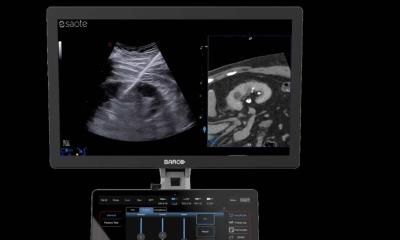
Whether using laser beams, high-frequency electrical current or, more recently, highly-focused ultrasound – direct image monitoring is used to control such procedures.
MEDICA 2006 is presenting a range of innovations in this area.
Magnetic resonance tomography (MRT) is considered one of the ideal tools for these less invasive procedures, not only because it is radiation-free, but also because it provides a continuous picture of temperature distribution.
The prognosis for patients with malignant liver tumours is poor, particularly for those with large tumours; following diagnosis, their average survival period is less than six months and, even for those with smaller tumours, estimates are that only one in four will survive beyond three years. Laser thermo-ablation, which involves destroying small tumours by applying localised heat, promises better survival rates.
Using this technique, at Frankfurt am Main University Hospital, Professor Thomas Vogl carried out tests on 80 patients. The results are impressive: 60% (compared with the usual 25%) reached a three-year survival period; around 33% survived for five years.
With twelve years’ experience in this area, Prof. Vogl now intends to use this therapy for tumours and metastases in the lung - an area of many complications. The frequency of this disease makes the less invasive procedure particularly desirable. Bi-polar high-frequency ablation could be combined with localised chemotherapy drugs to achieve success. To confine cytostatic substances within a tumour, magnetic particles have been added to them, so that when two magnets are applied externally, the iron particles – and thus the medication – cannot migrate.
Aiming to localise prostate cancer treatment, researchers at the Institute for Diagnostic and Interventional Radiology, in Frankfurt’s Johann Wolfgang Goethe University Hospital, are developing ‘galvanotherapy’. In this method, iontophoresis (or electromotive drug administration [EMDA]) is used. A DC current applied to the prostate gland draws the drugs to the cancer site.
The disadvantage in these therapies is that any tumour that is not totally destroyed will grow again - and more quickly than is usual, resulting in frequent aftercare.
Source: Medica
14.11.2006