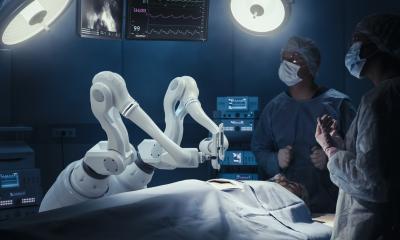
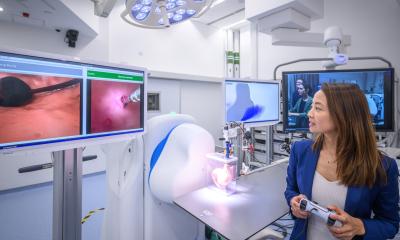
Google Glass goggles stream live surgery
Other beta test evaluation shows mixed result
Some time this year, exact date unknown, Google Glass – a miniature computer attached to a pair of glasses – is expected to make its consumer debut.
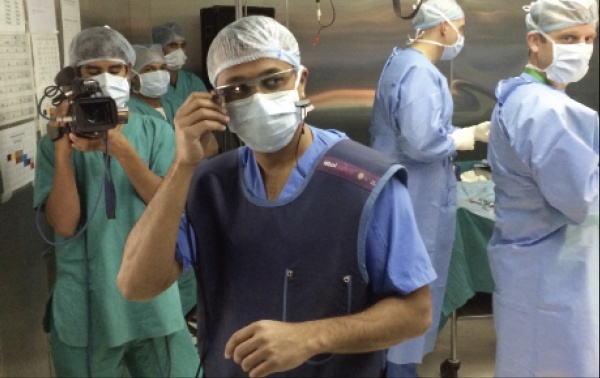
There’s a lot of interest by healthcare providers, some of whom are among thousands of Google-selected ‘explorers’ who paid $1,500 for the privilege of beta testing the preliminary system.
The Google Glass device is worn like a pair of glasses, but includes a computerised central processing unit, integrated display screen, high definition camera, microphone, speech recognition and dictation software, and has wireless connectivity. It will work with apps based on the Android operating system.
The reviews of Google Glass are mixed. Some perceive it as a gimmick and a patient privacy nightmare. Others are delighted. One medical school in California has even incorporated the use of Google Glass into its academic curriculum.
Interactive videoconferencing for consultation about patients and video streaming of treatment and surgeries are two of the most popular test applications.
In March 2014, Providence-based Rhode Island Hospital began a six-month long feasibility study to use a customised version of Google Glass containing a HIPAA security app in its emergency department, to stream live images of a patient’s dermatological condition to a consulting dermatologist. Emergency physician Dr Paul Porter, the project’s principal investigator, believes that the technology has the potential to make coordinated care easier and make interventions and treatment faster.
The New York Times has reported that Dr Paul P Szotek, a trauma surgeon at Indiana University Health, is currently developing an app for use by paramedics. Live feed streamed to the closest hospital emergency departments so that physicians can see accident victims at the scene.
He believes that wearable technology will be able to assess patients on the scene, give instructions to paramedics and better prepare for the patient’s arrival at an emergency department. ‘Google Glass has the potential to decrease the mortality associated with trauma significantly,’ he said.
Dr Selene G Parekh, an orthopaedic surgeon at Duke Medical Center and associate professor in the department of orthopaedic surgery at Duke University in Durham, NC, is planning to test the glasses to be able to stream his surgeries securely over the Internet to surgeons in India. While waiting for HIPAA privacy compliance to be established and for Duke Medical Center to approve this – anticipated in late fall of 2014 – he has been experiencing the use of Google Glass while performing surgeries.
Although videoconferencing using conventional equipment is commonplace to record surgeries, Dr Parekh believes that the technology will be more economical and shows tremendous potential. The surgeries will be streamed through Dr Parekh’s personal website at www.footonline.com and through the training website of the Parekh Family Foundation (www.footandanklecourse.com).
The foundation currently sponsors an annual Indo-US Foot and Ankle surgery Conference to disseminate and share techniques in foot and ankle surgery with surgeons in India and South Asia. Video streaming will enable surgeons around the world to join the video feed by using a secure website.
Dr Phi Haslan, a consultant interventional and uro-radiologist at the Freeman Hospital in Newcastle on Tyne, UK, also sees Google Glass as a way for an unlimited number of medical students and fellows to observe interventional radiology procedures without the necessity scrubbing up to stand in a crowded procedure suite and potentially be exposed to radiation. He also believes that the technology has potential to make image-guided procedures easier. The glasses with integrated computer technology may extend PACS image display as well.
Dr Oliver Muensterer, at the Division of Paediatric Surgery, New York Medical College in Valhalla, told European Hospital that he and his colleagues are planning a study to evaluate the head-up display of Google Glass for reading chest X-rays. Fifty radiographic images will be presented to surgeons to view on a conventional medical display PACS workstation monitor and on Google Glass.
The study’s objective is to compare the ability to identify the 25% of images with significant abnormal findings: pneumothorax, haemothorax and lung contusion.
Dr Muensterer et al. conducted the first formal systematic evaluation of the capabilities of Google Glass in clinical settings at Maria Fareri Children’s Hospital of Westchester Medical Center in New York. His team wore Google Glass for four consecutive weeks for hands-free photo/video documentation in clinic and in surgery, making hands free telephone calls, looking up procedure billing codes, and conducting Internet searches.
The beta version of Google Glass proved to be clunky. Its battery life is as short as 45 minutes when the video streaming application is used and several hours when it is not. However, some surgeries have a longer duration. The time it took to recharge the battery took hours.
The audio/speech recognition interface was inadequate except in a very quiet room. Some ergonomic features were awkward, and, when the researchers loaded PACS CT images into Google Glass, they discovered that the app displaying the images did not have a ‘rapid image scroll’ command.
Problems are to be expected in a beta test first generation version of any product. Other companies are starting to develop the technology as well. In his article published in the International Journal of Surgery earlier this year, Dr Muensterer concludes that ‘Google Glass has some clear utility in the clinical setting and foreseeably a great potential to impact medical and surgical practitioners in their daily activities.’
08.07.2014