EADV Symposium
Dermatologists and Venereologists discuss refugee crisis
The 13th Symposium of the European Academy of Dermatology and Venereology, which opened its doors last Thursday 19th May and took place in Athens, Greece, came to a conclusion yesterday, after more than 2,000 participants benefited from a series of scientific sessions focusing on the latest developments in Dermatology and Venereology.
“It’s time to talk about the refugee crisis in Europe in relation to our specialty,” said Prof. Roderick Hay, Professor of Cutaneous Infection at King’s College London and Adviser to the International Foundation for Dermatology, who was the keynote speaker at the plenary session of the Symposium. “Skin diseases are common in the world's poorest and most disadvantaged communities leading to discomfort, disfigurement and further marginalisation. The unhygienic and overcrowded conditions in which refugees have to live, lead to the development and spread of skin diseases. However, many of these have simple remedies. It’s our responsibility as Dermatologists to provide care and also train the aid workers who work in refugee camps to proper diagnose and to use the simple cost-effective treatments and preventive measures that are available.”
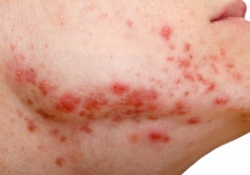
“Refugees and migrants often come from communities affected by war or economic crisis and undertake long, exhausting journeys that increase their risks for diseases. Therefore, at arrival, the most common skin diseases seen are infections related to poor hygiene and living conditions in overcrowded spaces, such as scabies, pediculosis and bacterial skin infections. Scald injuries and other infected traumas of the skin are also common, as well as dermatitis due to sun exposure and contact with sea water”, added Dr. Valeska Padovese, during her talk.
Dr. Federica Dassoni brought up the challenge of recognising skin diseases that are not common in Europe anymore. “We should be able to recognise, or at least suspect diseases that we are not used to seeing anymore, for example cutaneous leishmaniasis and cutaneous tuberculosis,” she highlighted.
“We should be vigilant and make sure we treat refugees and migrants for genetic and non-infectious skin diseases for their own benefit. We need to also keep in mind the need to protect them, in addition to the indigenous population, from possible infectious skin diseases, such as superficial mycoses, leprosy and yaws. Their syphilis serology may be positive even when they do not have or have had syphilis. This may be due to other infections than Sexually Transmitted Infections (STIs)” pointed out Dr. Bernard Naafs during his remarks.
Dr. Aldo Morrone elaborated on the issue of STIs: “Conflict and emergencies can disrupt HIV services; however, the prevalence of HIV infection is generally low among people from the Middle East and North Africa. Hence, there is a low risk that HIV will be brought to Europe by migrants from these countries. Despite a decline during the past decade, migrants still constitute 35 percent of new HIV cases in the European Union and the European Economic Area; however, there is increasing evidence that some migrants acquire HIV after their arrival. On the other hand, as many developing countries have a high burden of viral hepatitis, the increasing influx of refugees from highly endemic countries is changing the disease burden in Europe.”
When migrants and refugees are on the move, they often experience disrupted or uncertain supplies of safe food and water, as well as poor sanitation conditions, especially under difficult and sometimes desperate circumstances. Border or arrival points frequently lack sufficient numbers of sanitation facilities and washrooms; drinking water is often not available in sufficient amounts; hand washing with soap and personal hygiene, including laundry, is often compromised. Waste bins and regular removal of waste in reception centres are insufficient, posing additional health threats, such as flies, mosquitoes and rodents, which find breeding places in these areas and can transmit diseases or their bites can become infected.
“Refugees and migrants have a culture and a dignity that must be respected. They are not only individuals in need of help, culturally unable to get over a condition of misery. They are persons who have a lot to teach us in terms of solidarity, yearning for justice, and a wish to improve our society,” concluded Dr. Morrone.
Prof. Jan Gutermuth from the Vrije Universiteit Brussel (VUB, Brussels) explained that torture has been reported in ¾ of all countries around the world during the last years and refugees often stem from vulnerable groups. Torture survivors usually do not speak about their fate, even to medical doctors. They can show distinctive skin findings, which should be recognized, because even if the skin has healed, torture survivors often suffer from Post-Traumatic Stress Disorder, which has debilitating effects including anxiety, depression, self-isolation, withdrawal, memory and concentration impairments, nightmares and many more. In addition, neurologic or orthopedic complications can arise from torture and therefore it is important for health care providers to refer the victims to appropriate medical and psychological help.
Source: EADV
24.05.2016





