Controversy
Who should manage intensive care?
The question of who should manage intensive care was hotly debated at the 35th Annual Meeting of the German Society for Thoracic and Cardiovascular Surgery (GSTCVS); not always essentially, frequently aggressively, sometimes even insulting says EH Correspondent Holger Zorn
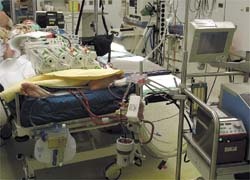
Since Diagnosis Related Groups (DRG) became the basis of accounting for hospital services in German hospitals at the expensive end of the market, university hospitals and other large hospitals have sought ways to optimise treatment processes. To save costs, following the example of central surgical areas plans are afoot to set up centralised intensive care wards (ICUs), which has been standard in primary and general care hospitals for a long time. Anaesthetists who have additional qualifications in intensive care usually run these wards.
Unlike many other surgical patients, cardiac and neurosurgery patients generally spend time on the intensive care wards following operations, which is why cardiosurgery and neurosurgery departments set up their own ICUs. Professor Thorsten Wahlers, Head of Cardiac Surgery at Cologne University Hospital and Board Member at GSTCVS, thinks that the proposed centralisation of intensive care will put patients at risk as ‘...an impairment of vital functions in these critically ill patients is always intrinsically linked to their underlying condition and their operations’. He sees intensive care as a ‘continuation of heart surgery’ and does not believe that anaesthetist colleagues are suitably qualified to supervise these patients’ care. ‘The patient comes to hospital for heart surgery, and to be treated by a cardiac surgeon, from the time when the diagnosis and treatment plan are made, followed by surgery, then intensive care, right through to the day of discharge.’
However, Prof. Joachim Radke, Head of Anaesthesiology and Intensive Care Medicine at the University Hospital Halle (Saale) and President of the German Society of Anaesthesiology and Intensive Care Medicine, retorted with the following figures: Whereas at the end of 2003, 2,237 anaesthetists had undergone advanced training in intensive care, only 54 cardiac surgeons had done so. And whereas there were 403 anaesthetists who were licensed to provide advanced training in intensive care, there were only 35 cardiac surgeons with this licence - in 79 hospitals! Surveys also show that, in purely surgical ICUs, some of the medical staff also carry out other duties, for example, work in the operating theatre (Muhl. E. Results of a survey on intensive care medicine at surgical university clinics in the first quarter of 2005. Chirurg BDC 2005; 7: M198-M203). In the surgical disciplines, additional training is limited to clinical images and disease patterns that are particular to that core medical field. Often, this part of training is given at the beginning of the advanced training period, before medics have actually gathered much surgical experience. However, in anaesthesiology, the additional training comprises the intensive, medical care of all critically ill patients in cooperation with those doctors treating their underlying medical conditions. Radke favours the interdisciplinary surgical intensive care ward where, with strict division of labour, shared legal responsibility and everything based on mutual trust, everybody works together with the motto ‘Let the best person do the job’.
‘Various training programmes for Surgical Assistants seem to tell us that medical jobs, for instance harvesting vessels, can be learned within a few weeks,’ a member of the audience remarked. ‘That’s why I’m not surprised some people believe that somebody who has had six months of advanced training can look after critically ill patients and head up an ICU in the same way that somebody would do after years and years of training.’
01.05.2006





