Article • Documentation & QC
Breakthrough law to insist on video cameras
Should video cameras record surgical procedures? Athletes and sports teams review videotapes of their performance to learn how to make improvements. Could surgeons and operating theatre teams use videotapes for quality improvement and to increase patient safety and clinical outcomes by identifying and reducing errors or bad practice? Or would this be an intrusion, a distraction for a surgical team?
Report: Cynthia E Keen
In addition to the expense of installing and maintaining sterile video cameras, videotape reviews would create their own set of issues and costs. Who would review? What protocols would be used to identify and report possible problems? At a time of lean budgets, from where would funding come to pay for this? These are unanswered questions, but video cameras in surgery are making the news.
Characterising ‘near miss’ events in complex laparoscopic surgery using video analysis
Root cause analysis of surgical complications are of high importance to ensure surgical quality, but specific details on technical causes often remain unclear.
Teodor P Grantcharov MD PhD
Teodor P Grantcharov MD PhD, a professor of surgery at the University of Toronto and a staff surgeon at St. Michael’s Hospital in Toronto, Ontario, has been recording his surgeries with a ‘black box’ he designed that works with laparoscopic procedures. The device records conversations in the operating theatre and records the video feed from the surgical camera being used, as well as a wide-angle view of activities within the room. Dr Grantcharov, also the Canada Research Chair in Simulation and Surgical Safety, meets with his surgical colleagues at St. Michael’s Hospital every week to review the collected data.
‘Root cause analysis of surgical complications are of high importance to ensure surgical quality, but specific details on technical causes often remain unclear,’ Dr Grantcharov said. ‘Near misses – situations that have the potential to result in an injury or adverse outcome – may not be captured by retrospective reviews of archived charts or malpractice claims. However, by identifying them, they allow protective measures to be taken to avoid future adverse events.’
Dr Grantcharov and colleagues conducted a study to analyse 54 unedited recordings of bariatric laparoscopic procedures. Their findings have been published in BMJ Quality and Safety.
66 events in 38 surgeries were identified, the majority of which were minor bleeding and haematoma. Bariatric surgeons rather than trainees caused the majority of these events and the most common injuries were due to basic surgical tasks.
‘The opportunity to learn from errors represents a valuable source of information that can be used to teach surgical decision making, risk management, and error recovery mechanisms. The current study highlights the benefits of detailed video analysis to create a database of common injury mechanisms and video clip repository that can be used in tailoring future training interventions, the study authors wrote, adding that understanding the casual relationship between minor errors and intraoperative events is essential to be able to develop effective error rescue mechanisms for future cases.
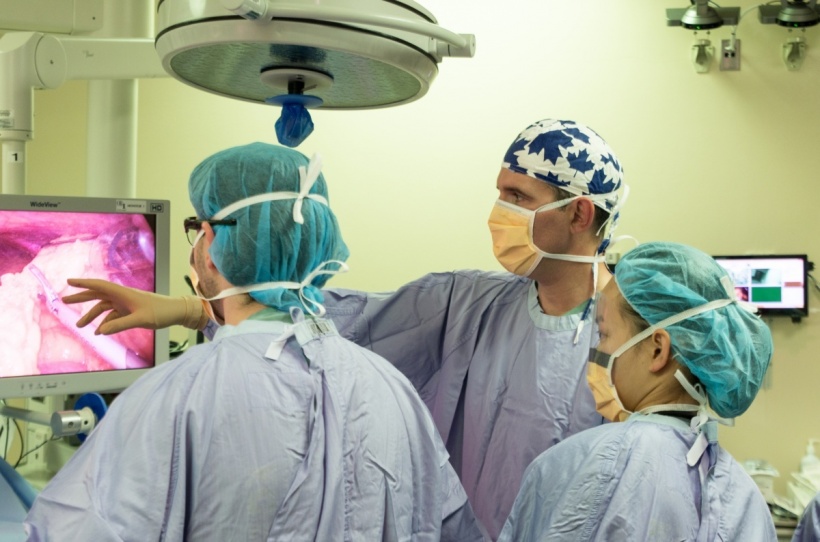
The ARIBO Project: a French study recording OR staff behaviours to reduce infection
In France, a multicentre prospective study is underway to record the behaviour of medical staff performing surgeries in 20 operating suites in 12 healthcare facilities used for cardiac and orthopaedic surgery. Motion tracking, using a video tracking system, is being used to assess the behaviours of surgeons, anaesthesiologists, nurses, and other clinicians entering operating rooms to determine their impact on surgical site infection risk during surgical site procedures.
Surgical site infection is a major public health problem, which substantially increases the severity of illness, length of hospital stay, mortality risk to patient, and related costs of treatment.
The study’s principal investigator Dr Gabriel Birgand of the University Paris Diderot and colleagues are trying to determine if movement in and out of the operating room during a surgical procedures and specific behaviours of clinical staff may be linked to the source of contamination of a surgical wound.
High-tech video tracking systems can obtain comprehensive and systematic data that is impossible to collect by human observers. However, the tracking systems do not actually record videos of the surgical procedure but rather the positions of the surgical staff. The number and length of times doors are opened and shut are also being analysed.
The study’s objectives are to assess best-practice guidelines in a surgical suite, to assess correlations between movements of the surgical team and surgical site infection risk, and to assess the correlation between the particle count and the microbiological contamination in the air. Additionally, the researchers are observing changes in practice by clinical staff when they know their movements are being videotaped.
Government legislation aims to protect patients from surgical errors
The introduction of video cameras in operating theatres could also be the result of government legislation designed to protect patients from accidental errors made during surgery. In April 2015, a bill requiring hospitals to install video cameras in operating rooms was introduced in the Wisconsin State legislature. The proposed legislation would require hospitals to offer videotaping to patients, or their guardians, of surgical procedures, and would also allow surgeons themselves to request this if the patient had no objections.
Milwaukee-area State representative Christine Sinicki introduced the bill so that plaintiffs in medical malpractice cases would have visual documentation. If the act is passed by the State legislature and signed by Wisconsin’s governor, the Julie Ayer Rubenzer law – named for a woman who died from an overdose of anaesthesia while undergoing breast implant surgery – will be the first of its kind in the USA.
The proposed legislation sparked a national debate about the merits of taping surgeries. Patient advocate organisations, such as the National Organisation for Medical Malpractice Victims, which represented the estimated 400,000 individuals who die annually in the USA from medical errors and oversights, consider this breakthrough legislation. To date, professional medical associations declined to comment.
13.11.2015