Article • Elastography
3-D Endocavity probe knocks for targeted prostate procedures
The prostate remains the only organ where random biopsies are performed to find cancer, notes Jean-Michel Correas MD PhD, from the Necker University Hospital in Paris. If we proposed this approach to a woman to search for breast cancer, it would be outrageous, he said.

This is mainly due to the limitations of prostate TRUS (Trans-Rectal Ultrasonography) using conventional ultrasound imaging (B-mode and Colour Flow), which detects less than 30% of cancer. While systematic biopsy techniques improve the detection rate, more than 20% of the cancers are still missed. Multi-parametric MRI (mpMRI) is helpful for the detection of significant high-grade prostate cancer, but the vast majority of biopsies are performed under ultrasound guidance.
MpMRI with fusion to ultrasound imaging allows targeting of suspicious prostate lesion and should improve the biopsy detection rates; however, the overall cost of the procedure (mpMRI + TRUS + pathology) is high, and the availability of MRI is low in many countries. Moreover ultrasound-MR fusion guided biopsy increases by a factor of two the examination time.
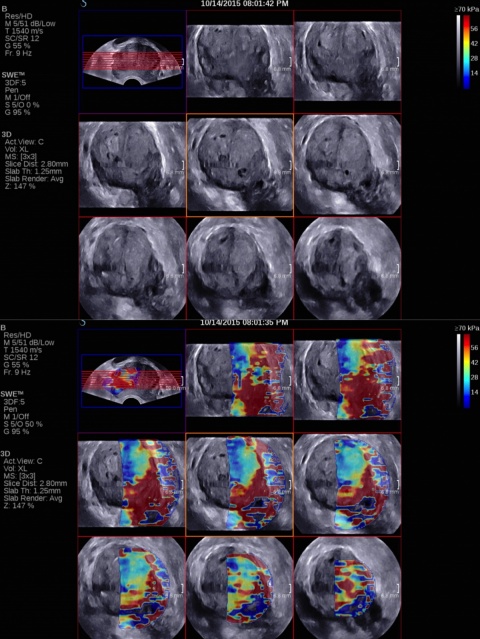
At the European Congress of Radiology in Vienna, Professor Correas will present his recent experiences using a new probe from SuperSonic Imagine, which he says brings a significant improvement to prostate imaging with ultrasound and provides a true alternative to mpMRI imaging targeting for prostate cancer (SuperSonic Imagine’s symposium, March 2nd, 12.30).
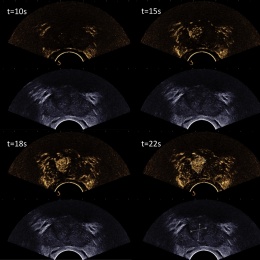
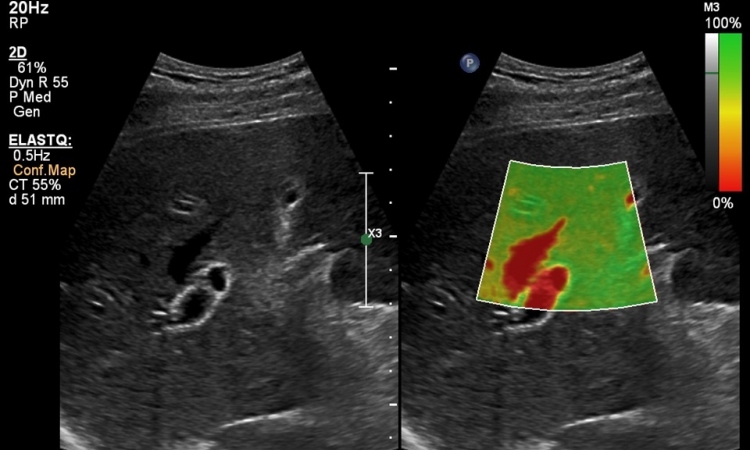
The SEV12-3 3-D Endocavity Transducer allows volumetric acquisitions of the whole prostate, and reconstructions of transversal, sagittal and coronal views not only in B-mode but also in colour Doppler and in ShearWave Elastography. Volumetric ShearWave Elastography enables measuring stiffness everywhere in the prostate in a very rapid manner (full volumetric SWE acquisition of the prostate obtained in a minute or less).
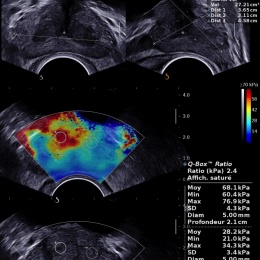
In a recent study performed by Correas with 2-D ShearWave Elastography on a population of 184 patients with biopsy proven cancers, it was shown that prostate tissue with higher stiffness (>35kPa) measured with ShearWave Elastography are at higher risk of malignancy*.
With 3-D ShearWave Elastography, for the first time, we can clearly identify and target suspicious regions of the prostate
Jean-Michel Correas
Another improvement with the new transducer is that ShearWave is now possible across the entire transversal view of the prostate, allowing the visualisation of tissue stiffness on both lobes and therefore enabling the comparison of stiffness of both lobes in 2-D or 3-D.
‘With 3-D ShearWave Elastography, for the first time, we can clearly identify and target suspicious regions of the prostate with an ultrasound based technique and perform targeted and systematic biopsies with the same imaging modality and probe,’ Correas said.
The professor also emphasised that the SEV12-3 3D probe works equally as well as a 2-D transducer with excellent B-mode imaging, which remains a very important modality to guide systematically randomised biopsies, as well as the capability to detect low-flow perfusion with a very sensitive Directional Colour Power Imaging and with contrast enhanced ultrasound (CEUS).
Therefore, prostate lesion detection with TRUS, like for MRI, has become a multiparametric imaging technique combining several TRUS data to identify suspicious lesions. 3-D ShearWave Elastography (combined with B-mode) may be used for detection of lesion because of its high sensitivity (>95%)* while CEUS could be used to further characterise and biopsy the suspicious lesions.
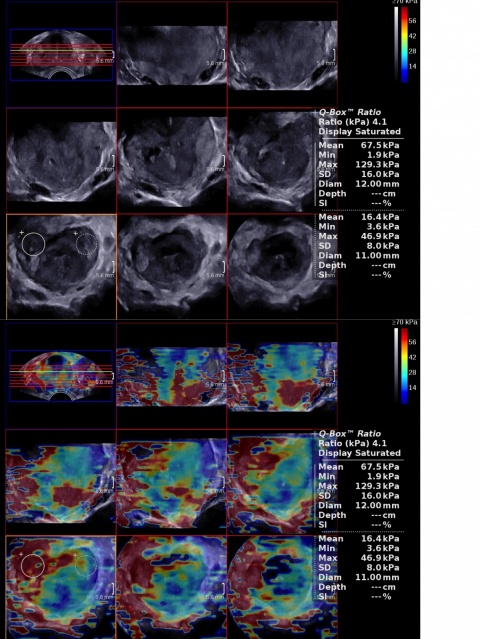
‘In recent years, the concept of focal therapy has gained more and more interest. The aim of partial prostate ablation is to provide treatment to the index prostate cancer (lesion with highest grade) without removing the entire prostate because it would reduce side effects significantly by leaving untouched sensible structures, such as the neurovascular bundle or the urinary sphincter.
The limitations of partial therapy for prostate cancer are the multifocal nature of the disease, as well as the problem of correct identification and localisation of the prostate cancer lesions by prostate biopsy and/or imaging. 3-D ShearWave may help detect this index lesion and would enable partial focal treatment of cancers with, for example, RFA, HIFU or cryo-ablation, Correas concluded.
* Correas JM, Tissier AM, Khairoune A, Vassiliu V, Mejean A, Helenon O, et al. Prostate Cancer: Diagnostic Performance of Real-time Shear-Wave Elastography. Radiology. 2015 Apr;275(1):280-9. PubMed PMID: 25599156.
Profile:
Jean-Michel Correas is Professor of Radiology at the Paris-Descartes University and vice-chairman of the Department of Adult Radiology in Necker University Hospital, Paris. He gained MD PhD degrees from the University of Tours and was Visiting Professor of Radiology at the University of Toronto department of Imaging Research. There he was headed several research projects on ultrasound contrast agents as part of his science doctorate on ultrasound contrast agents. He is deeply involved with the development of interventional uroradiology, and particularly biopsy procedures and guidance as well as minimally invasive treatment of renal tumours.
ECR 2016 - Don't miss
Sunday 6 March, 14:00–15:30 Room F1
Urogenital
05.03.2016