Article • Weaning off
These patients need more attention
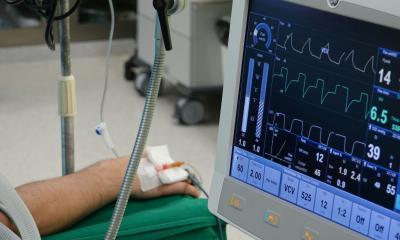
A study on weaning patients in intensive care units (ICUs) has compared those who underwent prolonged weaning off mechanical ventilation (MV) with patients classified as undergoing ‘simple’ or ‘difficult’ weaning. It shows that patients who experienced ‘prolonged’ weaning from mechanical ventilation show significantly higher mortality rates.
Report: Mark Nicholls

Dr Xiu-Ming Xi from the Department of Critical Care Medicine, Fuxing Hospital, Capital Medical University, Beijing, lead researcher of the team in China, explained that the findings indicate that patients who experience prolonged weaning should receive closer attention.
Clinicians treating such patients should, he suggested, place greater emphasis on actively controlling the diseases initiated by MV, to improve cardiopulmonary function and nerve and mental state, and begin functional rehabilitation exercises as early as possible to reduce the mechanical ventilation time. ‘In addition,’ he said, ‘tracheostomy should be considered earlier for patients who suffered from prolonged weaning because tracheostomy improved patients’ comfort and communication, reduced sedative use, and may have contributed to earlier weaning.’
Prolonged weaning occurs in patients who fail at least three weaning attempts or require seven days of weaning after the first Spontaneous Breathing Trial (SBT) and those falling into this area were at greater risk of dying.
Researchers found that patients in the prolonged weaning group had a longer MV duration, with 18% of patients in the prolonged weaning group needing prolonged MV. In addition, incidences of re-intubation, ventilator-related pneumonia, and mortality were significantly increased.
We found that a lower Glasgow score, and hyercapnia at the beginning of the weaning process, were independent risk factors for prolonged weaning.
Dr Xiu-Ming Xi
The study also showed that the patients with a low Glasgow Coma Scale score – a neurological scale giving a reliable and objective way of recording the conscious state of a person for initial and subsequent assessment – at the start of weaning, were more likely to have prolonged weaning, meaning that the patient’s consciousness level and mental status affect the success of weaning. ‘Higher PaCO2 levels at the initial SBT were independently related to prolonged weaning in our study,’ Xi pointed out, ‘Most patients undergoing weaning still have considerable gas exchange disturbances during the weaning process and may develop hypoxemia, hypercapnia, or both, during an SBT.
‘Patients who experience failed weaning are frequently unable to increase their minute ventilation in response to a high PaCO2 because of weakness of the respiratory muscles, altered respiratory mechanics, and other factors.’
The study follows a proposal at the International Consensus Conference to classify weaning of patients in intensive care units from mechanical ventilation into ‘simple’, ‘difficult’, and ‘prolonged’ weaning, based on the difficulty and length of the weaning process.
For the prospective cohort study, the Beijing team examined the incidence and outcome of weaning according to the new categories. Three hundred and forty-three patients were included in the final analysis. The prevalence of simple, difficult, and prolonged weaning was 200 (58%), 99 (29%), and 44 (13%) patients, respectively.
‘Patients who experienced prolonged weaning had a significant increase in both 60-day and hospital mortality compared with patients who experienced either simple or difficult weaning,’ said Xi.
‘We found that a lower Glasgow score, and hyercapnia at the beginning of the weaning process, were independent risk factors for prolonged weaning.’
In the prolonged weaning group, patients were more likely to be from the medical ward and to have pneumonia as the cause for initiation of MV; they were also older and had a higher APACHE II score (Acute Physiology and Chronic Health Evaluation II) - one of several ICU scoring systems to asses ICU patients - on admission to the ICU.
The study was performed at medical-surgical ICUs of 13 municipal hospitals in Beijing and all patients who had been intubated and mechanically ventilated for more than 24 hours were screened.
28.09.2016