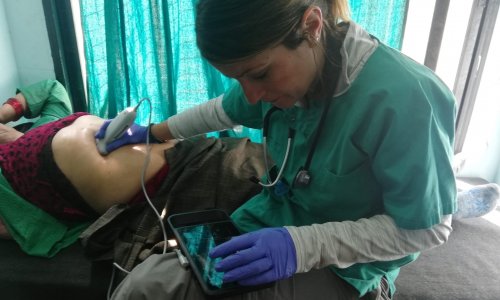
Sponsored • Point-of-care ultrasound
POCUS: Nothing gives so much info so quickly
Doctors working in the eight-bed Paediatric Intensive Care Unit (PICU) at the Ramón y Cajal University Hospital in Madrid extensively use point-of-care ultrasound to evaluate the condition of critically ill children, and they find it essential in their work, as Dr José Luis Vázquez Martínez, Head of PICU at Hospital Ramón y Cajal, with over 25 years’ experience in paediatric intensive care medicine, explained.
'Point-of-care ultrasound (POCUS) is used extensively in our unit, allowing comprehensive, head-to-toe assessment of critically ill children, including respiratory, oncology and post-operative cardiac patients, as well as those being treated for sepsis or multiple trauma. The POCUS approach allows not only an initial diagnosis, but also routine monitoring of treatment to see whether or not a patient’s condition changes, enabling alternative strategies to be implemented if there is no improvement.
POCUS helps paediatric doctors in many ways. For example, ultrasound scans enable evaluation of a patient’s haemodynamic state, looking at their heart function and blood volume to see if these factors are contributing to respiratory failure. Conversely, doctors can see if a lung problem, such as pneumonia, is affecting the heart. For a patient in a coma due to multiple trauma, ultrasound is used to look for signs of bleeding – a potential cause of unexplained anaemia – and to assess the intracranial pressure. It’s also used to monitor kidney function in children with blood pressure problems, and visualise intestinal indications of sepsis. In addition, ultrasound guidance can be used for endotracheal intubation. In short, broader applications that we did not anticipate until very recently. We have used ultrasound in our PICU for more than a decade, and have always had SonoSite systems, upgrading them as new technology is introduced. In the beginning, when my knowledge was more limited, the aim was to perform clinical echocardiography but, when the SonoSite representative showed me the linear probe and the various techniques available, it was as if I was being shown electricity after using candles! It was amazing, a real turning point in the use of ultrasound, and everyone recognised it as a step forward in the paediatric intensive care world.
Our advice to people attending our training courses, who do not have – or have to share – an ultrasound system, is to tell their hospital managers that, just like a ventilator, it is an essential piece of equipment for an intensive care unit
José Luis Vázquez Martínez
For the patients, a major benefit of ultrasound is that exposure to radiation can be reduced. Before ultrasound, X-ray examinations were performed two or three times in the first few days after admission to try to establish the cause of the problem, often with limited success. With ultrasound, we can scan the patient as often as necessary, implementing treatment and monitoring its effect without exposing the child to more radiation.
In PICU, we consider an ultrasound system essential – there is nothing else that gives us so much information, so quickly and non-invasively – and today we have a dedicated Edge II ultrasound system with linear, including hockey stick, and adult and paediatric cardiac transducers. It is in constant demand and is a perfect fit for our work, fulfilling all our expectations. All my colleagues use it, and we are very satisfied with it. The system is high quality and ergonomic, and strikes a good balance between image quality and ease of use. It is also quick to boot up, which is crucial for an instrument that is frequently moved between different beds in the unit. Robustness is vital too; if a patient deteriorates, we may have to move any equipment surrounding the bed very quickly to create space to treat them. However careful you are, there is always the risk of unintentional knocks to the system.

Source: FUJIFILM SonoSite
A while ago someone said to me that they ‘sell ultrasound machines, but don’t offer training’, but this view isn’t enough – it’s very short-sighted – training is very important. Ramón y Cajal pioneered the use of ultrasound in PICUs across Spain, and was the first hospital to offer external training courses for doctors from other facilities, initially focused on clinical echocardiography. Over time, this has expanded to include neuromonitoring, respiratory and abdominal monitoring. I acquired my ultrasound experience through a combination of external training in adult ultrasound and practical, hands-on learning, and am largely self-taught. If courses like these had been available when I started using ultrasound, I would have saved so much time. FUJIFILM SonoSite is clearly committed to organising and supporting ultrasound training, and this is unquestionably a great benefit to the scientific community – long may it last!
Today, we are seeing a boom in the use of ultrasound in paediatric care, as it non-invasively provides immediate information in situations where time is of the essence. Our advice to people attending our training courses, who do not have – or have to share – an ultrasound system, is to tell their hospital managers that, just like a ventilator, it is an essential piece of equipment for an intensive care unit.'
01.09.2018