Interview • IT analysis and study
Optimising OR procedures in orthopaedic surgery
Could surgical procedures for hip or knee arthritis be improved?
Interview: Katrin Schreiter
IT specialists at Leipzig University Hospital’s Innovation Center for Computer-Assisted Surgery (ICCAS), and physicians in the Department of Orthopaedic, Trauma and Plastic Surgery department, analysed and optimised the operating room (OR) setup, legwork and instruments handling. We asked project manager Juliane Neumann, at Leipzig University, why and how this developed.
HiE: How did you get on the subject of OR optimisation?

Juliane Neumann: ‘The number of hip and knee replacement surgeries is increasing steadily. Thus it makes sense to have a closer look at workflow efficiency. Physicians at the University Hospital asked us to help to review the intra-surgery processes. Both physicians and OR staff reported high physical stress levels, as well as inefficient workflows.
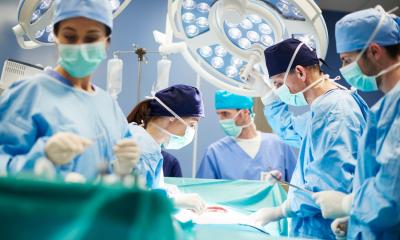
‘In a first step, our team observed several operations. We saw pretty much right away where the problems are. Most of the time the OR setup is far from ideal. This concerns both the way instruments are handed to the surgeon and team and the positioning of team members and the surgical equipment.’
This is where your work, as an IT specialist came in?

‘To date the table layout is based primarily on the personal preferences of the head surgeon, or on established processes. It took uninvolved bystanders to take an objective look at the OR setup. Thus we opted for a computer simulation. We made a 3-D model of the OR and simulated the processes during surgery.
‘Our focus was on mapping the hand-over times of the instruments and legwork of the different people. The position of the team in relation to the table and location of the equipment were other important factors. For each intervention – i.e. hip and knee – and for each side, left or right, we designed different setups which we then tested in the simulation environment. While doing these tests we varied, analysed and evaluated the position of the instrument tables, the OR staff and the instruments used. We used these data to calculate times.’
‘Our goal was to establish an improved OR setup for frequently performed hip and knee replacement surgeries. For knee and hip surgery individual clinical setups were designed for the right and left side. We adjusted the table position as well as of the staff, equipment, etc. to meet all hygiene, functional and spatial needs and requirements. The staff’s feedback was unanimously positive: firstly, average intervention time was reduced by four minutes and, secondly, ergonomics for the OR staff was significantly improved.’
What ergonomic aspects were affected?
‘OR technology is permanently updated, which includes large equipment. Staff must always adapt to each new situation. Let’s take the C-arm: the mobile X-ray system has to be accommodated in the OR and has to be integrated into the workflow. This needs adequate planning.’
Was there an effect on physical stress?
The new OR setup allows better leg positioning, which in turn reduces physical stress for the OR team
Juliane Neumann
‘Indeed, this was an area where we also saw improvements. During knee surgery it can happen that the OR team members have to hold the patient’s leg or medical instruments over an extended period of time in an awkward posture. The new OR setup allows better leg positioning, which in turn reduces physical stress for the OR team.’
Can your insights be transferred to other disciplines?
‘Yes, there are some general best practices for OR setup regarding hygiene, functional, spatial and ergonomics, aspects that apply to many types of ORs. For example the surgeon and the person handing the instruments should be as close as possible to each other to avoid frequent body rotations and to ensure that all the people involved have an unobstructed view of the operative field.’
Now that this project has been completed, what is your current focus?
‘The project to optimise OR processes in orthopaedic surgery ran for two years and is now over. Currently, we are looking at the way implants are being stored and the legwork involved. After all, even during surgery the implants and supplies have to be collected from storage. We aim to save resources. For example we want to avoid opening the wrong or unnecessary supply packages. The entire workflow can also be optimised by storing the supplies in a way that accelerates collection.‘
Profile:
Juliane Neumann is Senior Scientist at the Innovation Center Computer-Assisted Surgery (ICCAS), a research institute at the Medical School in the University of Leipzig, where she studies medical informatics and has been researching surgical and clinical process modelling since 2014. One focus of her work is the improvement of therapy methods and workflow to enhance patient safety and healthcare-related economic efficiency.
21.01.2021