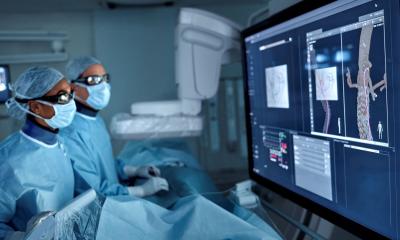
Photo: HiE/Behrends
Article • ECR 2026 imagines the future of the field
Enhanced by AI, but guided by humans: Radiology’s vision for 2050
Diagnostic imaging without actual images, but with sleek and shiny scanners; no more radiology and pathology departments, but virtual patient models and AI-enhanced surgical precision: At this year's European Congress of Radiology (ECR) in Vienna, two leading experts envisioned 2050 as a radically different future of medicine – less Grey's Anatomy, more Star Trek. They made it clear that the real question is not whether this future will arrive, but who will be there to shape it.
Article: Wolfgang Behrends
Prof. Regina Beets-Tan and Prof. Pedro Gouveia made their case on the ECR main stage – not through a conventional lecture, but in dialogue with an AI avatar. And even though the setting was decidedly futuristic, and the tone was generally light-hearted, the underlying issue was clear: radiologists today have to make sure that the technology of tomorrow will be implemented in a way that amplifies their own strengths and benefits their patients.
Digital insights to guide real-world actions
Scrolling through images is a thing of the past. We don't look at images. We explore the patients
Regina Beets-Tan
Prof. Beets-Tan – Chairwoman of the Department of Radiology at The Netherlands Cancer Institute in Amsterdam and former ECR Congress President – envisions a discipline transformed at its core. The radiologist of 2050 no longer produces images. Working from raw data, AI reconstructs the patient as a fully navigable three-dimensional model – organs, tumours, lymph nodes visible from every angle, at every depth. ‘Scrolling through images is a thing of the past. We don't look at images. We explore the patients.’
This fundamental change will see radiologists assuming a new role, which Beets-Tan described as “medical information specialist”, interpreting the imaging data, but also managing information from pathology, lab, from endoscopy – all fused by AI into one integrated report. ‘There are no separate departments anymore,’ predicted the expert. ‘We have merged into one big medical information lab, with advanced imaging and lab systems and massive computing power, all in the same place.’
A platinum portal into a not-too-distant future
Central to this data-driven vision is the digital twin: a continuously updated virtual patient model integrating imaging, genomics, pathology, lifestyle data, and real-time monitoring. Unlike a static dataset, it learns and adapts – simulating how a patient might respond to different treatments, running outcome scenarios, and identifying the pathway that maximises benefit and minimises harm.
Illustrating the imaging suite of the future, the experts presented a sleek, platinum-coated MRI system – a far cry from the bulky, claustrophobia-inducing machines of the past. With body weight and composition measured seamlessly on entry, and vital signs monitored continuously throughout, these scanners essentially become AI-powered digital twin factories. Too futuristic to be feasible? Beets-Tan pondered: ‘I was so lucky to start from conventional imaging and see the evolution into the current scanners. That was maybe 30 years ago – can you imagine that radiology will stay the same?’
Surgery reinvented: Simulation, precision, and the surgical sixth sense
As breast surgeon, Prof. Gouveia from the Champalimaud Foundation in Lisbon offered a different perspective on these developments: Using a patient’s digital twin enables thorough rehearsal of an operation, he ventured, while an AI performs thousands of surgical simulations to optimise the procedure for safety and outcomes: ‘No more surprises.’
We need AI to amplify our work, because our patients need better diagnostics and better treatments. That's the most important thing
Pedro Gouveia
In the OR itself, AI-stabilised smart scalpels respond to tissue in real time – ultrasonically guided, temperature-sensitive, adjusting their behaviour based on what they encounter. ‘Just like having a surgical sixth sense,’ the expert described. This advanced instrument could further be controlled via a neural interface, allowing the surgeon to activate the scalpel via brain signals instead of tapping for foot pedals. Sounds like more far-fetched science fiction? Driven as much by the gaming industry as by medicine, Gouveia predicted that this type of surgery ‘will come in the near future’.
In the 2050 scenario outlined on the ECR stage, surgical training is digitally overhauled as well: ‘Cadavers are out – immersive simulation is in,’ Gouveia said. Using full-sensory virtual reality with real-time feedback, haptics, error tracking, and gamification elements, acquiring surgery skills will be more efficient, he predicted, and – in keeping with the tongue-in-cheek tone of the session – added: ‘Don't worry – we'll still teach them compassion.’
Using technology to make medicine more human again
These aspects of humanity and empathy were at the core of the session’s final segment. The question on the table: what would this high-tech, AI-powered future mean for the individual radiologist? ‘I can assure you, you're not only going to supervise algorithms,’ Beets-Tan stated. Instead, she envisioned her 2050 colleagues to assume the role of “clinical orchestrators”, coordinating the insights gathered across the different specialties and creating a harmonised patient journey.
But instead of treating patients as a collection of data points, the new technology might even make medicine more compassionate again, Gouveia pointed out: ‘Currently we already have some problems with keeping being human while we are talking with our patients in appointment rooms. I do spend a lot of time looking into a small screen, typing on a keyboard, and the patient is looking at me.’ Using an AI assistant to prepare relevant data and take over documentation could enable a more dignified doctor-patient communication.
This aspect of human benefit should serve as guiding principle when adopting new technology, Beets-Tan advised: ‘Do not accept everything. Always ask the AI innovators: how will that improve the workflow that I'm already in?’ She urged her colleagues to take an active part in shaping this evolution to ensure that the future of healthcare is driven by human choices, not technology.
While many medical professionals perceive the increasing competence of AI as a threat, Gouveia drew a striking analogy to dissuade that fear: ‘Do you expect to run faster than your car? Obviously not. So you have to really see it as a tool, to help you.’ Used correctly, he argued, AI could be the solution, absorbing the administrative burden and restoring an increasingly rare commodity in modern medicine: the doctor's time and attention. ‘We need AI to amplify our work,’ he concluded, ‘because our patients need better diagnostics and better treatments. That's the most important thing.’
16.03.2026