Dressing up for Ebola’s unlikely EU epidemic
Unlike some news reports the Ebola virus is not as easily transmitted as influenza or other infections. Still, healthcare and laboratory workers must take precautions to quickly identify those infected and prevent an outbreak.
Report: Lisa Chamoff
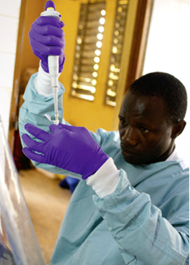
In an October webinar, hosted by the American Association for Clinical Chemistry, Dr Nancy Cornish, a medical officer at the Centers for Disease Control, emphasised that Ebola is transmitted by direct contact with blood and body fluids, and not spread by air or water. However, research laboratories making viral cultures so that pathogens achieve high concentrations, must increase safety precautions.
Anyone testing specimens from a possibly infected patient should wear gloves, water-resistant gowns, and full-face shields, or goggles and masks. Certified class II Biosafety cabinets or Plexiglass splashguards should be used to protect workers’ skin and mucous membranes.
Anyway, medics should anyway ensure minimum infection prevention practices in patient care, including hand washing, using gloves, gowns and masks, safe injection practices and cough etiquette, Cornish said, also stressing that African facilities dealing with Ebola specimens have a different set of challenges, including no reliable running water and limited access to disinfectants.
Dr Sheldon Campbell, Director of laboratories at VA Connecticut Healthcare and Professor of laboratory medicine at Yale School of Medicine, said facilities should come up with plans to include assessing the route and risk of transmission of certain organisms, and determine how common the pathogen is. When developing policies, Campbell said it’s important to balance laboratory staff risk with the possibility of compromising care for 100 or more patients.
‘When planning, plan for what’s reasonable now, and that’s really small numbers of at-risk patients to rule out for Ebola,’ Campbell said. ‘Don’t try to plan yet for 100 patients with Ebola, or even for five. Plan for one and get that in place and watch what happens over the next few months. You might have to plan for more, but start with small numbers of cases and then reassess as time goes by.’
30.10.2014