
most recent developments and its plans for the future.
Interview • Abbott cardiovascular
An increasingly dynamic cardiovascular presence
In the world of laboratory diagnostics, ‘Abbott’ is a household name. Few people however are aware of the fact that the company, headquartered in Illinois, USA, is also leading in other fields. A number of innovations in cardiac and vascular diagnostics and therapy might soon put Abbott in the limelight. Dr Angela Germer, Regional Director DACH, and Volker Keller, Head of Marketing DACH, Vascular at Abbott, updated HiE on the company’s most recent developments and the plans for the future.
Interview: Daniela Zimmermann
Abbott’s German cardiovascular business area operates from Wetzlar and Eschborn, in the Frankfurt/Main region, with Vascular und Structural Heart managed in Wetzlar. Whilst the Structural Heart team focuses on the treatment of structural heart disease (SDH), the Vascular team’s expertise lies in diagnosis and treatment of vascular conditions with systems to assess vascular physiology, guide wires, and drug-eluting, as well as non-drug eluting, balloons and stents.
OCT and FFR to avoid unnecessary stents
With this approach we aim to optimise percutaneous coronary interventions, PCI for short, and to increase the likelihood that the right stent is placed at the right location
Angela Germer
Today, some patients receive stents without proven ischaemia, on suspicion so to speak. Usually, two techniques are used to assess ischaemia: either fractional flow reserve (FFR) or resting full-cycle ratio (RFR). A specially designed pressure wire looks for drops in pressure caused by a stenosis. If the pressure drops significantly, the oxygen supply to the heart is impeded, says Dr. Angela Germer.
Abbott uses a two-pronged approach to ensure that stents are implanted when and where clinically needed and to improve patient outcomes: firstly, the guidewire PressureWire X uses wireless data transmission, thus facilitating ischaemia assessment by FFR; secondly, the Abbott-developed imaging solution OCT (optical coherence tomography) which allows precise measurement of vessels. ‘With this approach we aim to optimise percutaneous coronary interventions, PCI for short, and to increase the likelihood that the right stent is placed at the right location,’ Dr Angela Germer explains. OCT delivers high-resolution colour images to monitor vessels prior to the intervention as well as in the follow-up when the stent is checked for correct placement and functionality.
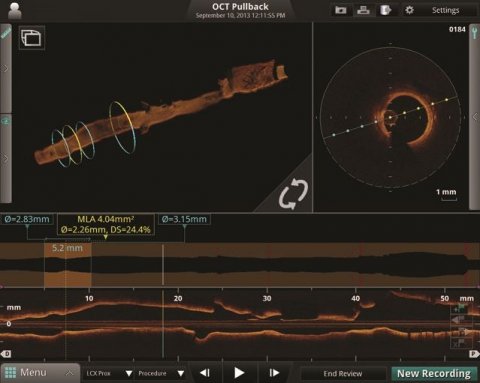
Image source: Abbott
Abbott supports physician training with modern technologies, such as virtual reality (VR). In cooperation with several hospitals, the company recorded catheter-based procedures, such as FFR und OCT, and turned them into 3-D simulations to be used with VR headsets. ‘Thus, interventions can be practised virtually, which increases patient safety during the actual procedure,’ Volker Keller points out. Abbott and the international cardiologist working group (AGIK) jointly organise workshops at trade fairs and congresses, and in hospitals, to provide in-depth training for clinical staff.
Pressure wire detects microvascular disease

Image source: Abbott
The pressure wire is also used to diagnose microvascular heart disease which, in Germany alone, affects 175,000 people, Dr. Germer says: ‘This condition is rather frequent among cardiac patients, but difficult to diagnose. Many patients present several times without the cardiologist being able to detect the root cause. Our PressureWire X, combined with a dedicated software solution, can help detect minute deposits in the vessels and thus identify the disease.’
The highly specialised Abbott stent portfolio covers the many requirements the tiny support structures have to fulfil in the different anatomies. Stents for the femoral artery, for example, must be able to withstand enormous biomechanical forces, such as torsion. ‘The nitriol wires in our Supera stent are not lasered but woven,’ Germer explains. ‘This unique technology makes Supera much sturdier than conventional stents, whilst maintaining its flexibility.’
Closure system accelerates patient mobility
Perclose ProGlide, the tried and tested closure system that deploys suture after endovascular procedures with a femoral puncture larger than 5F without the use of collagen, is now also indicated for the femoral vein. ‘A suture is placed right at the vessel wall and the edges are joined again initiating primary healing. The closure can be tested right after the intervention. Unlike conventional sutures, Perclose ProGlide allows the patient to get up and move around quickly,’ explains Dr. Germer. Thus, hospital length of stay is reduced and accompanying procedures, such as a bladder catheter, can be avoided. Another advantage: If re-access is necessary, which is, in fact, the case with several conditions, the very same site can be used, even right after the initial procedure.
FILVAS: Advanced LVAD improves life in cardiac insufficiency cases
Today, patients benefit hugely from implantable cardiac support systems, such as LVAD (left ventricular assist device). Abbott is currently developing the next-generation of such a device: FILVAS, fully implantable left ventricular assist system. It has no external components, such as battery packs or charging ports, which patients have to carry 24/7. FILVAS was recently designated a Breakthrough Device by the USA’s FDA. ‘Obviously, the new implant has to be charged regularly as well,’ Keller explains, ‘but FILVAS does this by induction via an implanted coil.’ Since energy supply does not require opening the abdomen, patients can bathe, swim, enjoy the sauna – these are activities that are almost, or even entirely, impossible with LVAD. Not to mention the fact that in conventional systems the external energy supply opening is a potential door for infections to enter the body.
AI algorithm calculates infarction risk
Abbott not only uses diagnostic and treatment devices to improve cardiac patient care but also designs solutions based on artificial intelligence (AI). A recently developed AI-based algorithm to assess infarction risk is about to be used in clinical settings. The Abbott R&D team benefited from the in-house lab medical expertise: ‘Our algorithm correlates troponin values with other patient data, such as age, gender or prior disease,’ Keller points out. ‘This allows a detailed assessment of individual infarction risk.’ Prior to the commercial launch of the algorithm, clinical tests need to be concluded but, so far, the studies have yielded very promising results.
With these ambitious projects in the wings, Abbott is well positioned to expand its reputation beyond the lab and have a strong impact in cardiovascular medicine.
30.06.2020





