Born with heart defect but living longer
Adults with congenital heart failure (CHD) are a growing special subset of patients with specific needs; most need lifelong care, but in adulthood many fail to receive it.
By Holger Zorn
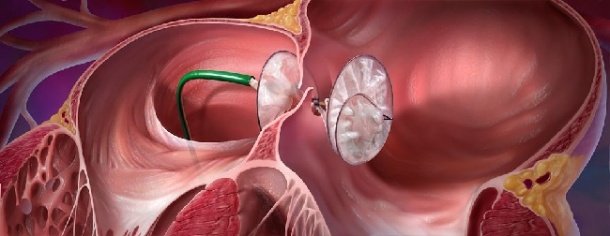
Source: W L Gore
Source: W L Gore
Up to 90% of children with CHD reach youth and adulthood due to progress in diagnostics and therapies in recent decades. Between 200,000 and 300,000 young children, adolescents and adults live with CHD in Germany alone. Highly complicated cardiac defects can be treated surgically with very good results. Interventional cardiac catheterisation techniques have progressed greatly and, by merging paediatric cardiac surgery and cardiology, the life expectancy of CHD newborns and young children has increased.
Atrial septal defect, the second most frequent cardiac problem, is now predominantly treated by intervention, introducing by catheter a two-piece umbrella-like ePTFE membrane prosthesis.
The rare hypoplastic left heart syndrome (HLHS)is fatal without surgery. In the early 80s, a triple surgical intervention strategy was developed -- the Norwood, Glenn and Fontan procedure – usually performed at ages 1-6 days, 3-6 month and 2-4 years. Today, the treated survivors are in their mid-20s, with life-time prognosis unknown.
Since all three procedures are very distressing, a new hybrid strategy has been developed, as Professor Felix Berger at the German Heart Center in Berlin, explains: ‘With the hybrid approach to HLHS, instead of the traditional Norwood I operation we can operate without the need for total circulatory arrest under deep hypothermia, which leads to a significant minimisation of the first surgical step. The complicated comprehensive step II can be postponed to later in life. Although the second step means a major surgical procedure, it’s combined with a significant volume unloading of the heart in one major procedure, since the Glenn anastomosis will be simultaneously established. We all hope that this new strategy will not only improve survival but also bring significant improvement of the entire outcome -- for example, neurodevelopment, ability index, exercise capacity.’
Lifelong care needs
Wiebke Lesch from the German Competence Network for Congenital Heart Defects surveyed 1,372 children, teenagers and young adults with CHD regarding their CHD knowledge and information needs. 52.3% responded, 174 of them were children aged 10-13, and 147 teenagers aged 14-17. Only 33.9% of the children and 44.9% of teenagers could define their CHD. 59.8% of children and 35.4% of teenagers stated that the doctor only talks to their parents. Consequently, only 40.8% of the children and 41.5% of teenagers reported that they fully understand the explanations of their doctor. ‘Young CHD patients have major gaps in their knowledge about their condition,’ Dr Lesch notes. ‘This may have harmful consequences.’
To address this problem, the German Federal Ministry of Education and Research awarded €16 million to a 10-year research project by the German Competence Network, which has established a National Register for CHDs, to provide a basis from scientists and clinicians can assess present CHD levels, carry out epidemiologic studies concerning quality of life and psychosocial aspects, evaluate current studies and exchange knowledge, and produce relevant information for patients and the public.
19.04.2011





