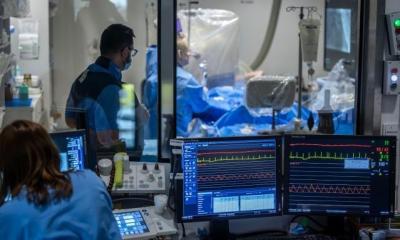
Photo: Mark Nicholls
Article • Emergency care crisis in the UK
Severe impact of ambulance handover delays
Patient care in the UK has hit a massive roadblock as delays in handovers between ambulances and emergency departments put patients at risk of serious harm.
Special report: Mark Nicholls
Delays in handovers between ambulances and NHS hospital emergency departments are impacting patient safety and putting lives at risk. The situation – set to become more severe with the onset of winter – is an indication of the serious emergency care crisis facing the NHS.
Rows of ambulances held in queues outside emergency departments waiting to admit patients to hospital is becoming an increasingly familiar scene in the UK. Senior figures across the health sector are becoming increasingly concerned at the levels of harm this bottleneck is causing patients.
Potential harm for over 40,000 patients
Figures provided by ambulance chiefs across England show that 169,000 hours of ambulance crews’ time was lost due to delays in October. As a result, paramedics could not answer 135,000 calls, a figure representing 23% of ambulance services’ total potential capacity to respond to 999 emergency calls.
The October handover statistics from the Association of Ambulance Chief Executives (AACE)1 also discloses that:
- 18% of ambulance handovers took more than an hour when the NHS target is 15 minutes;
- the average handover time was 42 minutes, up 12 minutes from October 2021; and
- delays exposed an estimated 41,000 patients to potential harm.
Of those, about 5,000 were put at risk of, or experienced ‘severe harm’, including death because they were waiting so long either to be admitted to Accident & Emergency Departments (A&E) or to get an ambulance to turn up to help them.

The bottleneck is being created by hospitals not being able to admit people fast enough from ambulances because of a shortage of beds. As a result, ambulances waiting at hospitals are tied up and not able to respond rapidly to other patients in the community needing emergency care. The latest handover delay findings coincide with a hard-hitting report by the AACE entitled “Delayed Hospital Handovers: Impact Assessment of Patient Harm.”2 It has been drawn up with the aim of assessing the potential harm that patients experience as a result of extended delays in their handover between ambulance and hospital clinicians.
A failing ‘safety net’
These crippling delays are a twin threat – they cause significant harm to patients who are forced to wait in the back of our ambulances, while our crews are stuck and therefore unable to respond to patients who need us out in the community
Martin Flaherty
Ambulance officers warn that patients are dying because of the delays since the service could no longer perform its role as a ‘safety net’ for people needing urgent medical help. ‘The life-saving safety net that NHS ambulance services provide is being severely compromised by these unnecessary delays and patients are dying and coming to harm as a result on a daily basis,’ said Martin Flaherty, managing director of the AACE, which represents the heads of England’s 10 regional NHS ambulance services. ‘These crippling delays are a twin threat – they cause significant harm to patients who are forced to wait in the back of our ambulances, while our crews are stuck and therefore unable to respond to patients who need us out in the community. As the colder winter weather approaches, we have serious concerns that things will get worse in the coming weeks and months.’
The nationally defined target for hospitals included in the NHS Standard Contract states that ‘all handovers between ambulance and A&E must take place within 15 minutes with none waiting more than 30 minutes.’ Since April 2018, an average of 190,000 handovers have missed this target every month (accounting for around half of all handovers). In September 2021, over 208,000 exceeded the 15 minutes target.
The AACE report was conducted as an exploratory exercise to work with all Integrated Care Systems (ICSs) and healthcare providers to work together to reduce the patient safety risks inherent in handover delays. The document warned that the risks of harm being caused by belated access to definitive care are clear and that some patients have died whilst waiting outside A&E departments. During the study, more than 8 out of 10 of those whose handover was delayed beyond 60 minutes were assessed as likely to have experienced some level of harm, with 10% classified as potentially experiencing severe harm. That amounts to 160,000 patients a year experiencing potential harm, with 12,000 potentially experiencing severe harm as a result of delayed handovers.
Clarion call
While acknowledging that ‘many things are changing for the better in the way healthcare is delivered’, handovers of patient at emergency departments remains a ‘significant problem.’ However, while the AACE believes the issue can be resolved, they say that a change in mindset is required, as is a wider awareness of the risks and responsibilities involved. ‘Innovative and collective thinking is required, with more focus on out-of-hospital care provision and care pathways availability, including other services that can take the pressure off EDs,’ the document states.
The experts emphasise the report is not a finger-pointing exercise, with no single sector to blame in an “ever-fluctuating environment” but warn that it is “a clarion call” of the need for improvement. Ambulance chiefs want to see a consistent methodology adopted by ICSs to measure potential and actual harm arising from handover delays and long waits in the community as they strive to tackle the problem.
What they say about the crisis…
Health secretary Steve Barclay has highlighted handover delays as a major challenge facing the NHS, with A&E doctors sharing AACE’s concern. Meanwhile, the GMB, the union which represents 15,000 staff in English ambulance services, say the ambulance service is “close to collapse” as a result of vacancies, underfunding, low morale and demand for ambulance care having doubled to 14m calls a year since 2010. Unions have cited the problems facing the emergency care system as one of the factors motivating members to vote for a walkout.
A Department of Health and Social Care spokesperson said it is investing in the NHS to improve patient flow through hospitals and get ambulances back on the roads quickly and will publish a full recovery plan for urgent and emergency care next year.
The College of Paramedics echoed the handover report figures and chief executive Tracy Nicholls said: ‘We all know patients are coming to harm and in some cases severe harm.’
The Royal College of Emergency Medicine believes disruption to emergency care may account for around a quarter of these deaths.
Matthew Taylor of the NHS Confederation, which represents hospitals, said the data showed the NHS was facing ‘one of the worst winters for decades.’
References:
05.12.2022